ECMO machine on patient takes center stage, this opening passage invites readers to explore a world crafted with good knowledge, ensuring a reading experience that is both absorbing and distinctly original.
Throughout history, ECMO technology has advanced to support patients with cardiac or respiratory failure, and its primary function is to provide cardiopulmonary bypass and oxygenation. An ECMO machine works by circulating a patient’s blood outside the body, removing carbon dioxide and adding oxygen through an artificial circuit.
Introduction to ECMO Machine
ECMO machine, also known as Extracorporeal Membrane Oxygenation, is a life-support device that uses a pump and oxygenation system to temporarily replace the function of the heart and lungs in patients with severe cardiac or respiratory failure. It’s like a mechanical heart and lung that helps these vital organs recover or function properly until the patient can breathe and pump blood on their own again. ECMO has been a crucial tool for medical professionals to save lives and improve outcomes for patients with life-threatening conditions.
Role of ECMO in Supporting Patients

ECMO is a specialized treatment used to support patients with life-threatening cardiac or respiratory conditions that are unresponsive to conventional medical treatment. This includes conditions such as:
ECMO is used in conjunction with other treatments, such as medications, surgery, and mechanical ventilation, to provide comprehensive care for these critically ill patients.
Historical Development of ECMO Technology
The development of ECMO technology has been an evolution of medical advancements and technologies.
* In the 1950s, Dr. John Gibbon invented the first heart-lung machine, which laid the foundation for modern ECMO technology.
* In the 1960s, ECMO was initially used as a bridge to transplantation for patients with end-stage heart or lung disease.
* In the 1980s, ECMO evolved to be used more widely in the ICU setting for patients with severe cardiac or respiratory failure.
* Today, ECMO is used in many hospitals and medical centers around the world to support patients with a range of life-threatening conditions.
Types of ECMO, Ecmo machine on patient
There are several types of ECMO treatments, including:
Cardiopulmonary (or biventilation) ECMO: This type of ECMO supports both heart and lung function in patients with life-threatening cardiac or respiratory failure.
Veno-arterial (or VA) ECMO: This type of ECMO uses a pump to oxygenate the patient’s blood and remove carbon dioxide, but does not use a lung.
Veno-venous (or VV) ECMO: This type of ECMO uses a pump to oxygenate the patient’s blood and remove carbon dioxide, but does not use a lung.
Benefits and Risks of ECMO
While ECMO has revolutionized the treatment of patients with life-threatening cardiac or respiratory conditions, there are also some potential risks and side effects associated with its use:
These risks and side effects highlight the importance of careful patient selection and close monitoring during ECMO treatment.
ECMO and Patient Outcomes
ECMO has been shown to improve patient outcomes and survival rates in multiple clinical studies and trials.
In summary, ECMO machine is a vital tool in the treatment of patients with severe cardiac or respiratory failure. Its historical development, types, benefits, and risks, highlight the importance of this life-saving technology in modern medicine.
Working Mechanism of ECMO Machine
The ECMO machine is a sophisticated device that supports patients with severe cardiopulmonary failure by taking over the functions of the heart and lungs. It works on a circuit that includes a pump, an oxygenator, and a heat exchanger. The primary goal of the ECMO machine is to provide a temporary solution until the patient can recover or receive a transplant.
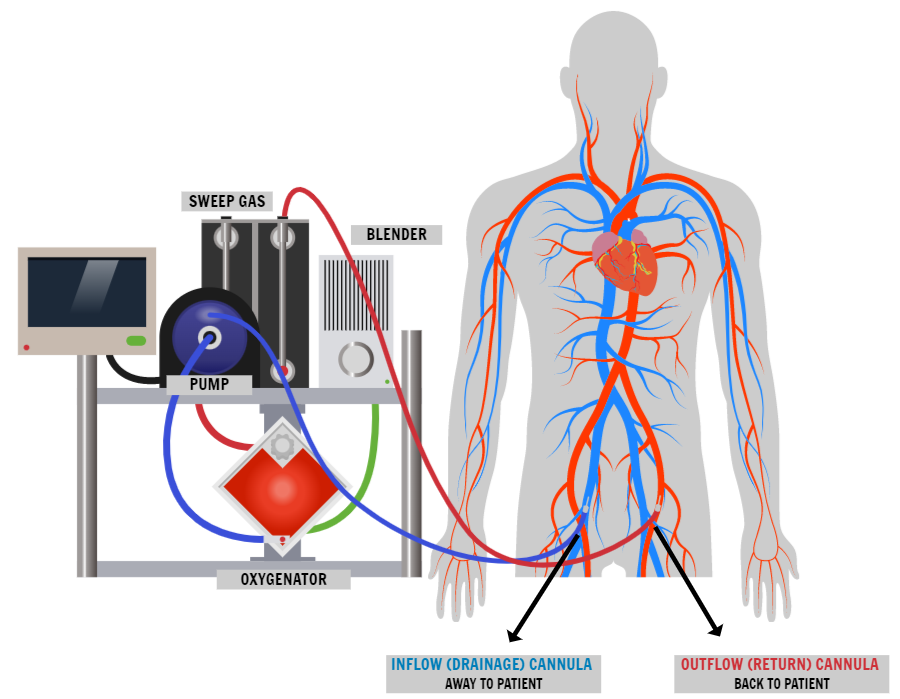
The ECMO Circuit
The ECMO circuit is the main pathway through which the blood travels between the patient and the ECMO machine. It consists of three main components: the cannula, the tubing, and the ECMO console.
Process of Cardiopulmonary Bypass and Oxygenation
Cardiopulmonary bypass is the process by which the ECMO machine takes over the functions of the heart and lungs. This is done by circulating blood through the ECMO circuit, where it is oxygenated, warmed, and cooled as needed. The process can be broken down into the following steps:
- Arterial cannulation: A cannula is inserted into the patient’s artery to withdraw blood from the patient.
- Deoxygenation: The blood is diverted from the patient’s heart and lung and sent to the ECMO machine for processing.
- Oxygenation: The ECMO machine adds oxygen to the blood and removes carbon dioxide through the oxygenator.
- Heat exchange: The ECMO machine warms or cools the blood, depending on the patient’s needs, using the heat exchanger.
- Return to patient: The oxygenated and conditioned blood is then returned to the patient through the venous cannula.
Components and Functions of an ECMO Machine
An ECMO machine consists of several components that work together to provide the necessary support for the patient. These include:
- Pump: The pump is responsible for circulating the blood through the ECMO circuit, providing the necessary flow rate and pressure to support the patient.
- Oxygenator: The oxygenator is responsible for adding oxygen to the blood and removing carbon dioxide.
- Heat exchanger: The heat exchanger is responsible for warming or cooling the blood, depending on the patient’s needs.
- Cannulae: The cannulae are the tubes that connect the patient to the ECMO machine, allowing blood to be drawn from the patient and returned to the patient.
The ECMO machine is a critical tool in the treatment of patients with severe cardiopulmonary failure. It provides a temporary solution until the patient can recover or receive a transplant.
Indications and Contraindications for ECMO
Indications and contraindications are vital to understand ECMO’s effectiveness, ensuring its proper application and avoiding unnecessary complications.
Common Indications for ECMO
Common indications for ECMO include patients experiencing cardiac arrest due to conditions such as myocardial infarction (heart attack) and cardiac surgery complications. In cases of sepsis, ECMO can help by reducing the load on the heart and lungs, giving the patient’s body more time to fight the infection. Respiratory failure caused by conditions such as COVID-19, pneumonia, and acute respiratory distress syndrome (ARDS) is another common indication. Additionally, ECMO can support patients undergoing high-risk surgeries or in need of bridge-to-transplant therapy. A recent surge in COVID-19 patients has driven ECMO’s usage, underscoring its crucial application in life-threatening situations.
Contraindications for ECMO
While ECMO can be life-saving, there are certain conditions that make its application counterproductive and may even exacerbate the patient’s condition.
- Irreversible brain death – ECMO is not useful here since it cannot restore brain function and would be an unnecessary intervention. ECMO relies on the patient’s organs being functional enough to respond to the intervention.
ECMO Indications, Contraindications, and Potential Complications
The following table Artikels ECMO’s common indications, contraindications, and potential complications:
| Indications | Contraindications | Potential Complications |
|---|---|---|
| Cardiac arrest | Irreversible brain death | Bleeding complications, neurological damage, lung injury, and infections |
| Sepsis and organ failure | Severe chronic kidney disease, terminal cancer | Pulmonary edema, stroke, and respiratory failure |
| Respiratory failure (e.g. COVID-19) | Severe trauma with spinal cord injury, severe chronic kidney disease | Lung injury, stroke, and severe sepsis |
Patient Monitoring and Management

Monitoring patients closely during ECMO therapy is crucial for detecting early signs of complications and making timely interventions to prevent severe outcomes. ECMO is a complex treatment, and close monitoring is necessary to balance the delicate balance between supporting life and minimizing the risks associated with the therapy.
Monitoring Equipment and Techniques
ECMO patients require continuous monitoring of their vital signs, laboratory tests, and other parameters to assess the effectiveness of the therapy and detect potential complications. The monitoring equipment used in ECMO patients includes:
- Vital sign monitoring equipment, such as cardiac monitors, blood pressure monitors, and oxygen saturation monitors, to track changes in heart rate, blood pressure, and oxygen saturation.
- Laboratory tests, including blood gas analysis, complete blood counts, and coagulation studies, to assess the patient’s acid-base balance, blood cell counts, and blood clotting status.
- Imaging studies, such as chest X-rays and echocardiograms, to evaluate the patient’s heart and lung function.
- Nutritional monitoring, including monitoring of intravenous nutrition and feeding tubes, to ensure the patient is receiving adequate nutrients.
It is essential to note that the choice of monitoring equipment and techniques may vary depending on the patient’s specific needs and the medical team’s preferences.
Management of Complications
Despite careful monitoring, ECMO patients may still develop complications, such as bleeding, thrombosis, and infection. The management of these complications requires a multidisciplinary approach and prompt intervention to prevent severe outcomes.
- Bleeding complications can occur due to the anticoagulation therapy required for ECMO. Management strategies include:
- Increasing the dose of anticoagulation therapy to prevent clot formation.
- Treating bleeding sites with topical hemostatic agents or surgical intervention.
- Considering the use of tranexamic acid or other hemostatic agents to reduce bleeding.
- Thrombosis complications can occur due to the mechanical stress associated with ECMO. Management strategies include:
- Anticoagulation therapy to reduce clot formation.
- Thrombolytic therapy to dissolve clots.
- Surgical intervention to remove clots or repair damaged blood vessels.
- Infection complications can occur due to the invasive nature of ECMO. Management strategies include:
- Administering antibiotics to treat suspected infections.
- Performing surgical debridement or drainage to remove infected tissue or fluid.
- Using antiseptic solutions to prevent the spread of infection.
The management of complications in ECMO patients requires a team-based approach and prompt intervention to prevent severe outcomes. It is essential to note that the management strategies may vary depending on the patient’s specific needs and the medical team’s preferences.
“Close monitoring and timely intervention are critical in managing ECMO patients to prevent severe complications and ensure optimal outcomes.”
Surgical Preparations and Techniques
Surgical preparations for ECMO are crucial to ensuring a smooth and successful procedure for the patient. This involves careful planning, selection of appropriate cannulation sites, and precise insertion techniques.
Preoperative Preparations
To prepare a patient for ECMO, the following steps are taken:
- Complete history and physical examination to assess the patient’s overall health and identify any potential contraindications for ECMO.
- Order laboratory tests, including blood counts, electrolyte panels, and coagulation studies, to evaluate the patient’s hematologic and coagulation status.
- Perform imaging studies, such as chest X-rays and echocardiograms, to assess the patient’s cardiac function and identify any potential issues with cannulation.
- Administer antibiotics and anti-coagulation medications as necessary to prevent infection and promote hemostasis.
- Ensure that the patient is appropriately sedated and paralyzed to prevent movement during the procedure.
Surgical Techniques for ECMO Cannulation and Insertion
The surgical techniques for ECMO cannulation and insertion involve creating access to the patient’s circulatory system to establish the necessary flow for ECMO support. The primary goals are to achieve optimal cannulation site selection and ensure accurate placement of the cannulae to minimize complications and promote effective cardiopulmonary support.
- The most common cannulation sites are the carotid arteries in the neck and the femoral arteries in the groin.
- Ultrasound guidance is often used to assist in cannula placement and ensure accurate positioning.
- The surgical team carefully prepares the patient’s skin and tissue around the cannulation site to minimize bleeding and promote healing.
- The cannulae are inserted under sterile conditions and secured in place using sutures or other fixation devices.
Postoperative Care and Management of Patients on ECMO
After successful activation of ECMO support, the patient requires careful postoperative care and management to ensure smooth transition and optimal outcomes. This involves close monitoring of the patient’s vital signs, bleeding, and hemostasis.
- Monitor the patient’s blood pressure, heart rate, respiratory rate, and oxygen saturation to assess the effectiveness of ECMO support.
- Regularly check the patient’s bleeding sites for bleeding or oozing and take prompt action to control any bleeding episodes.
- Administer medications as necessary to manage bleeding, maintain hemostasis, and control infection.
- Closely monitor the patient’s laboratory values, including blood counts, electrolyte panels, and coagulation studies, to assess the patient’s response to ECMO support.
ECMO support requires close monitoring and prompt intervention to minimize complications and ensure optimal outcomes.
Complications and Risks Associated with ECMO
Complications associated with ECMO can be categorized into immediate and long-term effects. The immediate risks include bleeding, thrombosis, cardiac dysfunction, and other complications related to the insertion and management of the ECMO circuit. Long-term effects may include changes in the patient’s quality of life, potential for organ dysfunction, and the risk of rehospitalization.
Bleeding Complications
Bleeding is a common complication associated with ECMO, especially in patients receiving anticoagulation therapy. The anticoagulation protocol is typically managed according to the patient’s clinical condition, the type of ECMO circuit used, and laboratory values. However, bleeding complications may still occur, particularly in patients with underlying coagulopathies or those receiving high doses of anticoagulants. Management of bleeding complications may involve reducing the dose of anticoagulants, transfusing clotting factors, or using platelet transfusions as needed.
- Management strategies for bleeding complications should be individualized based on the patient’s clinical condition, ECMO circuit type, and laboratory values.
- Monitoring the patient’s coagulation status and adjust the anticoagulation protocol as necessary is crucial to minimize bleeding risks.
Thrombosis Complications
Thrombosis is another significant risk associated with ECMO, particularly if the ECMO circuit is not properly managed. Thrombosis can occur in the ECMO circuit itself, resulting in the need for circuit changes or thrombectomy. Additionally, thrombosis may occur in other parts of the body, such as the lungs, kidneys, or liver. Prevention strategies for thrombosis include using heparin-free circuits, applying adequate anticoagulation protocols, and carefully monitoring the patient’s coagulation status.
- Thrombosis risk can be minimized by using heparin-free circuits, proper anticoagulation protocols, and meticulous patient monitoring.
- Early detection and management of thrombosis are crucial to prevent further complications and ensure optimal patient outcomes.
Cardiac Dysfunction Complications
Cardiac dysfunction is a serious complication associated with ECMO, particularly if the patient’s cardiac function was already compromised before ECMO initiation. The patient’s cardiac function should be carefully monitored during ECMO support, and adjustments to the ECMO circuit settings or the administration of inotropes may be necessary to maintain optimal cardiac function.
- Cardiac dysfunction risk can be minimized by carefully monitoring the patient’s cardiac function, adjusting ECMO circuit settings as necessary, and using inotropes to support cardiac function.
- Regular echocardiograms and other cardiac monitoring tests may be required to assess cardiac function and guide management decisions.
Long-term Effects on Quality of Life
Long-term effects of ECMO can include changes in the patient’s quality of life, such as muscle weakness, joint pain, and cognitive impairment. These effects may be related to the duration of ECMO support, the presence of underlying chronic illnesses, and the extent of organ dysfunction. Regular follow-up care is essential to identify and manage these long-term effects.
| Potential long-term effects | Frequency and severity |
|---|---|
| Muscle weakness | Common, can be severe |
| Joint pain | Common, can be moderate to severe |
| Cognitive impairment | Rare, can be severe |
Training and Education for ECMO Professionals
To provide high-quality care to patients on ECMO, medical professionals must undergo rigorous training and education. ECMO specialists need to acquire a unique blend of technical knowledge, clinical skills, and emotional intelligence to navigate the complexities of ECMO therapy.
Essential Skills and Knowledge for ECMO Professionals
ECMO professionals should possess a strong foundation in various areas, including:
- Basic life support and critical care medicine skills
- Understanding of cardiac anatomy and physiology
- Knowledge of ECMO circuitry and equipment operation
- Ability to interpret ECMO-related monitoring data
- Skilled in patient assessment and management
- Experience with invasive and non-invasive monitoring techniques
- Familiarity with cardiopulmonary bypass and circulatory support principles
- Understanding of organ dysfunction and failure management
These skills and knowledge areas form the foundation for effective ECMO care and require continuous refinement and updating due to advancements in technology and clinical practices.
Types of Training Programs and Certifications Available for ECMO Professionals
Several training programs and certifications can enhance an ECMO professional’s expertise and stay current with industry developments. These include:
- ECMO certification courses offered by professional organizations like the Extracorporeal Life Support Organization (ELSO) or the Society of Thoracic Surgeons (STS)
- Residency and fellowship programs focusing on critical care, cardiothoracic surgery, or anesthesiology with ECMO training
- Workshops and conference sessions on ECMO-related topics, such as patient management, circuit troubleshooting, and new technology updates
- Maintenance of Certification (MOC) programs for ECMO professionals, ensuring continuous education and professional growth
Regular participation in ongoing education and professional development programs helps ECMO professionals stay up-to-date with the latest clinical practices, improving patient outcomes and enhancing their professional expertise.
Importance of Ongoing Education and Professional Development in ECMO Care
ECMO is a rapidly evolving field, with new technologies, and treatments emerging continuously. ECMO professionals must commit to ongoing education and professional development to stay current with the latest advancements and ensure optimal patient care. This includes:
- Staying informed about new ECMO-related studies and research findings
- Participating in regular conferences, workshops, and online educational sessions
- Engaging with peers and mentors for knowledge sharing and collaboration
- Adopting evidence-based practices and incorporating emerging technologies into clinical care
Ongoing education and professional development enable ECMO professionals to deliver the highest level of care, addressing the complex needs of patients on ECMO therapy.
Conclusive Thoughts
In conclusion, this discussion highlights the importance of ECMO machines in patient care and provides a comprehensive overview of the indications, contraindications, and complications associated with its use. With its ability to support patients with cardiac or respiratory failure, ECMO technology continues to shape the future of healthcare.
Question Bank: Ecmo Machine On Patient
What is ECMO?
ECMO stands for Extracorporeal Membrane Oxygenation, a life-support therapy that provides temporary support for patients with cardiac or respiratory failure.
How does ECMO work?
An ECMO machine works by circulating a patient’s blood outside the body, removing carbon dioxide and adding oxygen through an artificial circuit.
What are the indications for ECMO?
The common indications for ECMO include cardiac arrest, sepsis, and respiratory failure.
What are the risks associated with ECMO?
The common complications and risks associated with ECMO include bleeding, thrombosis, and cardiac dysfunction.