With radiation machine for breast cancer at the forefront, innovative technology has opened doors to treatment options like never before. From targeted radiation therapy to advanced radiation machines, we’re diving into the world of breast cancer treatment to explore the latest advancements and what they mean for patients.
The journey to beating breast cancer involves more than just surgery – it also requires precise radiation therapy to eliminate cancer cells. In this article, we’ll delve into the principles of radiation therapy, the types of radiation machines used for breast cancer treatment, and the importance of radiation oncologists and oncology nurses in planning and delivering radiation therapy.
Radiotherapy Machines for Breast Cancer Treatment
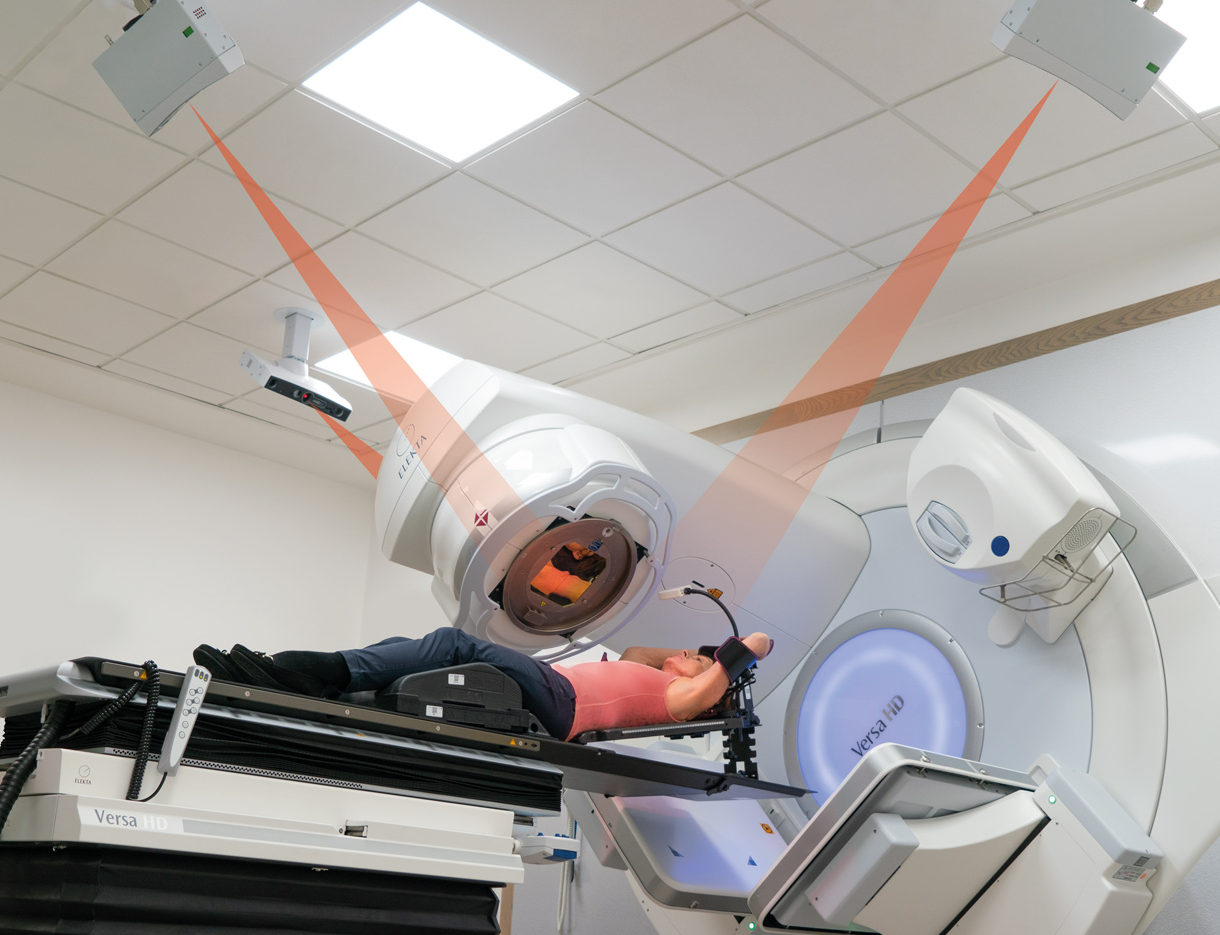
Breast cancer treatment often involves the use of radiation therapy to kill cancer cells and shrink tumors. Radiotherapy machines, such as linear accelerators and X-ray machines, play a crucial role in this process by delivering precise doses of radiation to target areas.
Types of Radiotherapy Machines Used for Breast Cancer Treatment
There are two main types of radiotherapy machines used for breast cancer treatment: linear accelerators and X-ray machines. Here’s a comparison of their advantages and disadvantages.
Linear Accelerators
Linear accelerators are the most commonly used radiotherapy machines for breast cancer treatment. They accelerate electrons to high speeds, which are then used to create intense radiation beams. Linear accelerators offer several advantages over X-ray machines, including:
- High precision and accuracy in delivering radiation doses
- Flexibility in treating various types of breast cancer, including tumors located close to the heart or lungs
- Ability to treat multiple cancer sites simultaneously
- Short treatment duration, typically lasting several weeks
However, linear accelerators also have some disadvantages, including:
- High costs of purchase and maintenance
- Requires skilled personnel to operate and maintain
- May cause skin reactions and other side effects due to high doses of radiation
X-ray Machines
X-ray machines use electrons accelerated by the X-ray machine’s vacuum tube to produce radiation. X-ray machines have the following advantages:
- Low costs of purchase and maintenance compared to linear accelerators
- Easier operation and maintenance due to simpler design
- Faster treatment delivery, typically lasting several minutes
However, X-ray machines also have some disadvantages, including:
- Lower precision and accuracy in delivering radiation doses compared to linear accelerators
- Limited flexibility in treating breast cancer, particularly tumors located near the heart or lungs
- Higher risk of skin reactions and other side effects due to high doses of radiation
How Radiotherapy Machines Target Cancer Cells
Radiotherapy machines work by targeting cancer cells with precise doses of radiation. The process involves several steps:
- Accurate localization of the tumor using imaging techniques such as CT scans or mammograms
- Positioning the patient in the correct position using a customized immobilization device
- Delivery of radiation doses to the tumor using the radiotherapy machine
- Monitoring and adjusting the radiation dose as needed to ensure maximum cancer cell killing while minimizing side effects
By targeting cancer cells with precise doses of radiation, radiotherapy machines play a crucial role in breast cancer treatment, helping to improve patient outcomes and quality of life.
Radiotherapy Techniques, Radiation machine for breast cancer
Radiotherapy machines can use various techniques to deliver radiation doses to the tumor, including:
- Intensity-modulated radiation therapy (IMRT): allows for precise dose delivery to the tumor while minimizing exposure to surrounding healthy tissues
- Stereotactic body radiation therapy (SBRT): delivers high doses of radiation to the tumor in a small number of fractions, minimizing treatment duration
- Adaptive radiation therapy (ART): allows for real-time adjustments to the radiation plan based on patient movement and tumor size
These techniques have revolutionized radiotherapy by enabling more precise and effective treatment delivery, resulting in improved patient outcomes and reduced side effects.
Biological Effects of Radiation
Radiation therapy works by damaging the DNA of cancer cells, leading to cell death or inhibition of cell division. The biological effects of radiation on cancer cells include:
- DNA damage: radiation can cause double-strand breaks in DNA, leading to cell death or mutations
- Proliferation inhibition: radiation can inhibit cell division, leading to tumor shrinkage and cell death
- Apoptosis: radiation can induce programmed cell death, leading to tumor regression
Treatment Planning and Simulation
Treatment planning and simulation are critical components of radiotherapy, involving the creation of a customized radiation plan based on patient anatomy and tumor location. This plan is then simulated to ensure accurate delivery of radiation doses and to minimize side effects.
Principles of Radiation Therapy
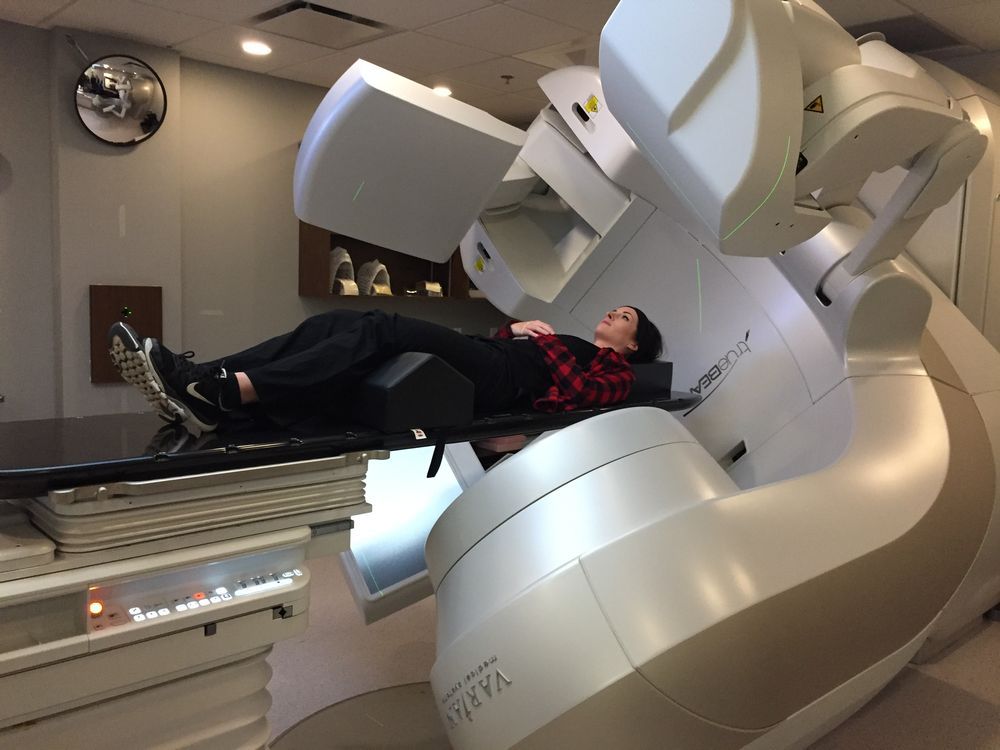
Radiation therapy is a vital treatment option for breast cancer patients, using high-energy rays to kill or control cancer cells. The process is meticulously planned and implemented by a team of radiation oncologists, physicists, and dosimetrists. Radiation machines are designed to deliver precise doses of radiation to cancer cells while sparing surrounding healthy tissues.
Radiation machines work on the principle of high-energy particle acceleration, where a linear accelerator (linac) produces a beam of radiation that is directed at the tumor site. This beam is shaped to conform to the tumor’s size and location, ensuring maximum destruction of cancer cells while minimizing damage to surrounding tissues.
Types of Radiation Modalities
Breast cancer treatment often employs various radiation modalities to maximize effectiveness. Some common modalities include:
3D Conformal Radiation Therapy (3D-CRT)
This is a technique where the radiation beam is shaped to conform to the 3D shape of the tumor, allowing for precise targeting of cancer cells. Advanced imaging techniques, such as CT or MRI scans, are used to create precise 3D images of the tumor. The radiation beam is then shaped to match the tumor’s contours, ensuring maximum radiation delivery to the cancer cells.
Intensity-Modulated Radiation Therapy (IMRT)
A type of 3D-CRT that allows for the modulation of radiation intensity across the tumor. This means that the radiation beam can be customized to deliver higher doses to certain areas of the tumor while sparing surrounding tissues.
Stereotactic Body Radiation Therapy (SBRT)
This is a type of radiation therapy that uses multiple high-dose beams to target specific areas of the tumor. SBRT is often used for smaller tumors and can lead to fewer side effects compared to traditional radiation therapy.
Role of Radiation Oncologists
Radiation oncologists play a crucial role in planning and delivering radiation therapy for breast cancer patients. They work closely with the patient and their team to develop an individualized treatment plan, taking into account the patient’s specific needs and medical history. Radiation oncologists use advanced imaging technologies to create precise 3D images of the tumor, which are then used to plan the radiation treatment.
Planning and Delivery
The planning process involves creating a customized radiation plan, which takes into account the patient’s specific needs, tumor size and location, and surrounding tissues. The plan is then implemented using a linear accelerator (linac) or other specialized equipment. Radiation oncologists continuously monitor the patient’s response to treatment and make adjustments as needed to ensure the best possible outcome.
Targeted Radiation Treatments for Breast Cancer
Targeted radiation treatments have revolutionized the field of cancer care by providing more precise and effective ways to destroy cancer cells while minimizing damage to surrounding healthy tissue. Stereotactic body radiation therapy (SBRT) and intensity-modulated radiation therapy (IMRT) are two such treatments that have gained significant attention in recent years.
Stereotactic Body Radiation Therapy (SBRT)
SBRT involves delivering high doses of radiation to a specific tumor site over a period of one to five fractions. This treatment is ideal for early-stage breast cancer and can be administered in just a few days. SBRT uses advanced imaging technology, such as CT scans and MRI, to create a precise map of the tumor and surrounding healthy tissue. This map helps the radiation oncologist to deliver high doses of radiation to the tumor while minimizing damage to nearby structures.
Intensity-Modulated Radiation Therapy (IMRT)
IMRT is a highly precise form of radiation therapy that involves delivering radiation beams of varying intensities to a tumor from different angles. This treatment allows for the creation of a customized radiation plan that can be tailored to the individual needs of each patient. IMRT is particularly useful for treating tumors that are close to critical structures, such as the heart or lungs.
Benefits of Targeted Radiation Treatments
Targeted radiation treatments offer numerous benefits to patients, including:
- Reduced side effects: Targeted radiation treatments minimize damage to surrounding healthy tissue, resulting in fewer side effects compared to traditional radiation therapy.
- Improved tumor control: Stereotactic and intensity-modulated radiation therapies can deliver high doses of radiation to the tumor, making them effective in controlling tumor growth and recurrence.
- Increased precision: Advanced imaging technology and precise radiation planning enable radiation oncologists to deliver radiation with high accuracy and precision.
Eligibility for Targeted Radiation Treatments
Not all patients with breast cancer are eligible for targeted radiation treatments. The following factors determine eligibility:
- Tumor size and location: SBRT and IMRT are typically reserved for early-stage breast cancer or tumors that are not amenable to surgical resection.
- Overall health: Patients with significant medical comorbidities or compromised lung function may not be good candidates for SBRT or IMRT.
- Radiation tolerance: Some patients may have a higher radiation tolerance than others, making them better candidates for SBRT or IMRT.
Radiation Oncologist Expertise
Radiation oncologists play a critical role in delivering targeted radiation treatments. They must have extensive training and experience in advanced radiation therapy techniques, such as SBRT and IMRT. Patients seeking targeted radiation treatments should consult with a board-certified radiation oncologist to determine if they are a suitable candidate for these treatments.
By leveraging cutting-edge technology and expert radiation oncology care, targeted radiation treatments offer a promising solution for breast cancer patients seeking effective and minimally invasive treatment options.
Brachytherapy for Breast Cancer
Brachytherapy is a type of internal radiation therapy where a small amount of radioactive material is placed inside or close to the tumor. This allows for a precise delivery of radiation to the cancer cells, reducing the risk of damage to healthy tissues. Brachytherapy for breast cancer has gained popularity in recent years due to its effectiveness in controlling the growth of tumors and reducing the risk of recurrence.
Brachytherapy for breast cancer typically involves the placement of small radioactive seeds, wires, or catheters in or around the tumor. These radioactive materials emit high-energy rays that kill cancer cells and damage their DNA, preventing them from dividing and growing. The duration and intensity of the radiation exposure can be adjusted depending on the type and stage of the cancer, as well as the patient’s overall health.
Types of Brachytherapy for Breast Cancer
There are two main types of brachytherapy for breast cancer: temporary and permanent. Temporary brachytherapy involves the placement of radioactive material that is left in place for a few minutes to several hours, while permanent brachytherapy involves the implantation of radioactive seeds that remain in the body permanently.
Benefits of Brachytherapy for Breast Cancer
Brachytherapy for breast cancer offers several benefits over traditional radiation therapy, including reduced side effects and improved cosmetic outcomes. Because the radioactive material is placed directly in or around the tumor, the risk of damage to surrounding healthy tissues is minimized. This results in fewer side effects, such as fatigue, skin changes, and lymphedema.
How Brachytherapy Fits into the Overall Treatment Plan
Brachytherapy is often used in combination with external beam radiation therapy and surgery to treat breast cancer. The treatment plan is tailored to the individual patient’s needs, taking into account the size, location, and stage of the tumor, as well as the patient’s overall health. Brachytherapy can be used to treat early-stage cancers, as well as more advanced tumors that have recurred or are refractory to other treatments.
Common Brachytherapy Techniques Used in Breast Cancer
There are several common brachytherapy techniques used in breast cancer, including:
- Interstitial brachytherapy, where radioactive seeds or wires are placed directly into the tumor.
- Intraoperative brachytherapy, where radioactive seeds or wires are placed into the tumor during surgery.
- Permanent seed implantation, where small radioactive seeds are implanted into the tumor.
- Temporary wire implantation, where radioactive wires are placed into the tumor for a period of time.
These techniques can be used alone or in combination to deliver the optimal dose of radiation to the tumor while minimizing damage to surrounding healthy tissues.
Risks and Complications of Brachytherapy for Breast Cancer
While brachytherapy is an effective treatment for breast cancer, it is not without risks and complications. Some potential risks include:
- temporary changes in skin color or texture
- temporary numbness or tingling in the breast or surrounding tissues
- infection or inflammation at the site of the implant
- radioactive material migration or leakage
However, with proper selection and careful planning, the risks associated with brachytherapy can be minimized, and the benefits of this treatment can be fully realized.
Future Directions in Brachytherapy for Breast Cancer
Brachytherapy for breast cancer continues to evolve, with ongoing research focused on improving the accuracy and efficacy of this treatment. Some potential future directions include:
- Developing more precise and targeted radiation delivery systems
- Improving the accuracy of tumor dosing and treatment planning
- Using brachytherapy to treat smaller or earlier-stage cancers
These advancements will help to further reduce the risks associated with brachytherapy and enhance the benefits of this treatment for breast cancer patients.
Radiation Machine Maintenance and Quality Assurance
Radiation machine maintenance and quality assurance are crucial for ensuring the accuracy and safety of breast cancer treatment. Regular maintenance and quality assurance procedures help prevent equipment failures, ensure radiation doses are delivered accurately, and minimize the risk of side effects for patients.
Importance of Regular Maintenance
Radiation machines used in breast cancer treatment require regular maintenance to function properly. This includes daily, weekly, and monthly checks to ensure the machine is functioning within specified limits. If maintenance is neglected, it can lead to equipment failures, inaccurate radiation doses, and compromised patient safety.
- Prevent equipment failures: Regular maintenance helps identify and address potential issues before they cause equipment failures.
- Ensure accurate radiation doses: Maintenance procedures help ensure that radiation doses are delivered accurately, which is critical for effective treatment.
- Minimize patient risk: Neglecting maintenance can lead to inaccurate radiation doses, which can increase the risk of side effects and complications for patients.
Procedures for Quality Assurance
Quality assurance procedures are essential for ensuring that radiation machines are functioning within specified limits. This includes calibration and verification of radiation doses, as well as daily checks on machine performance.
Calibration and Verification of Radiation Doses
Calibration and verification of radiation doses involve checking that the machine is delivering the specified dose of radiation to the treatment area. This is critical for ensuring that treatment is effective and safe.
| Procedure | Description |
|---|---|
| Calibration | A process that ensures the machine is delivering the specified dose of radiation. |
| Verification | A process that checks that the machine is delivering the correct dose of radiation. |
Consequences of Neglecting Radiation Machine Maintenance and Quality Assurance
Neglecting radiation machine maintenance and quality assurance can have serious consequences for patients and healthcare institutions. This includes increased risk of side effects, equipment failures, and compromised patient safety.
- Increased risk of side effects: Neglecting maintenance can lead to inaccurate radiation doses, which can increase the risk of side effects and complications for patients.
- Equipment failures: Neglecting maintenance can lead to equipment failures, which can result in treatment being delayed or canceled.
- Compromised patient safety: Neglecting quality assurance procedures can compromise patient safety, leading to unnecessary risks and harm.
The consequences of neglecting radiation machine maintenance and quality assurance can be severe, and it is essential that healthcare institutions prioritize these procedures to ensure patient safety and effective treatment.
Clinical Trials and Ongoing Research: Radiation Machine For Breast Cancer
Ongoing clinical trials play a vital role in advancing the treatment and management of breast cancer using radiation. These trials aim to evaluate new radiation modalities or techniques for breast cancer treatment, with the ultimate goal of improving patient outcomes. By participating in clinical trials, researchers can gather valuable insights into the safety, efficacy, and potential benefits of novel radiation approaches.
“Every volunteer who participates in a clinical trial contributes to the advancement of medical science and improves the care available to future patients.” – National Cancer Institute
Ongoing Clinical Trials Evaluating New Radiation Modalities
Several ongoing clinical trials are investigating new radiation modalities for breast cancer treatment, including:
- The use of hypofractionated radiation therapy, which involves delivering higher doses of radiation in fewer fractions, leading to reduced treatment duration and improved patient convenience.
- The application of stereotactic body radiation therapy (SBRT), a technique that delivers precise, high doses of radiation to small tumors using multiple beams.
- The investigation of particle therapy, such as proton or carbon ion therapy, which can offer improved targeting and reduced side effects compared to conventional radiation.
To participate in clinical trials, patients can search for ongoing studies through the National Cancer Institute’s (NCI) clinical trials finder (
Emerging Trends in Radiation Therapy for Breast Cancer
Researchers are also exploring emerging trends and potential advancements in radiation therapy for breast cancer, including:
- The development of AI-powered radiation therapy, which can help personalize treatment plans and optimize dose delivery.
- The use of radiation therapy in combination with immunotherapy, a type of treatment that harnesses the body’s immune system to fight cancer.
- The investigation of novel radiation-induced gene expression biomarkers, which can provide valuable insights into treatment response and patient prognosis.
These emerging trends hold promise for improving patient outcomes and reducing side effects associated with breast cancer treatment.
Patient Participation in Clinical Trials
Patient participation in clinical trials is crucial for advancing medical research and improving treatment options. By participating, patients can benefit from:
- Access to cutting-edge treatments and innovative therapies.
- The potential for improved outcomes and longer survival rates.
- The contribution to the advancement of medical knowledge and future treatment options.
Researchers emphasize that patient participation is voluntary and patients must provide informed consent before joining a clinical trial. Participating patients will be closely monitored by healthcare professionals and receive regular updates on their treatment and progress.
Future Directions in Radiation Therapy Research
As research continues to advance, future directions in radiation therapy for breast cancer may include:
- The development of more precise and personalized radiation therapy approaches.
- The expansion of radiation oncology capabilities to treat more complex cases and rare tumor types.
- The integration of radiation therapy with other treatment modalities, such as surgery and immunotherapy.
These future directions hold promise for improving patient outcomes and reducing the burden of breast cancer worldwide.
Final Wrap-Up

As we wrap up our discussion on radiation machine for breast cancer, it’s clear that there’s still much to be discovered. From ongoing clinical trials to emerging trends in radiation therapy, the future of breast cancer treatment holds great promise for patients and medical professionals alike.
Thanks for joining us on this journey into the world of radiation machine for breast cancer – we hope you’ve gained valuable insights and a deeper understanding of this complex and ever-evolving field. Remember, knowledge is power, and education is key to making informed decisions about your health.
FAQ Corner
Q: What is the most effective type of radiation machine for breast cancer treatment?
A: The most effective type of radiation machine for breast cancer treatment varies depending on the individual case. Common types include linear accelerators, X-ray machines, and stereotactic body radiation therapy (SBRT) machines.
Q: How do radiation oncologists plan radiation therapy for breast cancer patients?
A: Radiation oncologists use advanced imaging technologies and computer simulations to plan radiation therapy, taking into account the size and location of the tumor, as well as the individual patient’s anatomy.
Q: What are the most common side effects of radiation therapy for breast cancer?
A: Common side effects of radiation therapy for breast cancer include skin changes, fatigue, and lymphedema. Radiation oncology nurses play a crucial role in monitoring patient side effects and providing guidance on managing them.