Bipap vs cpap machine –
Delving into Bipap vs Cpap machine, this article delves into the intricacies of these machines in respiratory therapy. Bipap and Cpap machines have revolutionized the treatment of respiratory conditions, but choosing the right one can be daunting for healthcare professionals and patients alike. In this article, we will explore the primary functions, mechanisms of action, and similarities and differences between Bipap and Cpap machines in terms of their applications and patient populations.
Understanding the capabilities and limitations of each machine is crucial in making an informed decision. This article aims to provide a comprehensive overview of Bipap and Cpap machines, shedding light on their design, operation, and benefits, as well as their drawbacks and limitations. By the end of this article, readers will have a better understanding of when to choose Bipap over Cpap or vice versa, as well as the importance of proper assembly, calibration, and maintenance for optimal performance.
Understanding Bipap and Cpap Machines

Bipap and Cpap machines are two types of respiratory assistive devices used to treat various sleep-related breathing disorders and other respiratory conditions. These devices provide a crucial source of supplemental oxygen, pressure, and airflow to help patients breathe more comfortably and effectively.
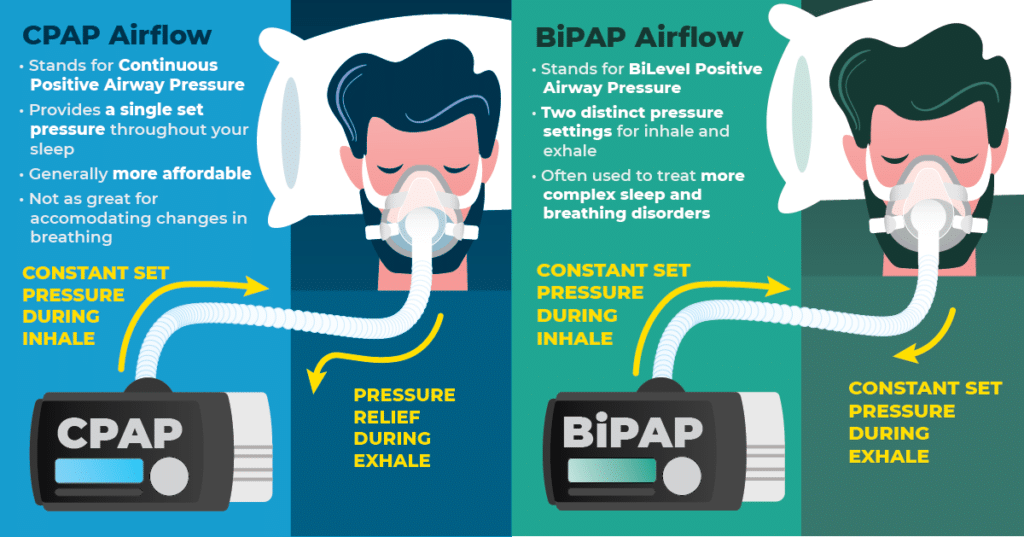
The primary function of Cpap (Continuous Positive Airway Pressure) and Bipap (Bilevel Positive Airway Pressure) machines is to deliver controlled air pressure into the airways, keeping them open and allowing for proper airflow. This results in improved breathing patterns, increased oxygen levels in the blood, and enhanced overall quality of life for patients.
Mechanisms of Action
Cpap machines work by delivering a consistent level of air pressure throughout the entire respiratory cycle. The air pressure is constantly applied to the airways, preventing them from collapsing and reducing the likelihood of sleep apnea episodes.
On the other hand, Bipap machines deliver two distinct levels of air pressure: one during inhalation (inspiratory pressure) and another during exhalation (expiratory pressure). This allows patients to exhale with less resistance, making it easier to expel carbon dioxide from the lungs.
Key Similarities and Differences, Bipap vs cpap machine
While both Cpap and Bipap machines work similarly in providing supplemental air pressure, there are key differences in their applications and patient populations.
- Fully Adjustable Pressure Levels: Cpap and Bipap machines both allow for fully adjustable pressure levels, allowing healthcare professionals to tailor the treatment to each individual patient’s needs.
- Variable Pressure Settings: Bipap devices are more versatile, enabling a wider range of pressure settings for both inhalation and exhalation.
- Patient Suitability: Cpap machines are generally recommended for patients with mild to moderate sleep apnea, whereas Bipap devices are often more suitable for patients with more severe or complex respiratory conditions.
- Therapeutic Goals: Cpap machines aim to prevent or reduce sleep apnea episodes by maintaining a steady air pressure, while Bipap devices target a broader range of respiratory symptoms, such as reduced carbon dioxide levels and improved breathing patterns.
- Treatment Outcomes: Cpap and Bipap devices both demonstrate effectiveness in improving sleep quality, reducing symptoms of sleep apnea, and enhancing overall patient well-being.
Technical Specifications and Maintenance
To ensure optimal performance and longevity, both Cpap and Bipap machines come equipped with advanced features and maintenance options.
- Heated Humidifiers: Many modern Cpap and Bipap devices feature built-in heated humidifiers to prevent airway dryness and discomfort.
- Removable Tubing: Removable tubing on both machines makes cleaning and replacing the tubes easy and hassle-free.
- Pressure Gauges and Alarms: Cpap and Bipap devices often include pressure gauges and alarms to alert the user of potential issues, such as pressure drop or equipment malfunction.
- Compact Designs: Both Cpap and Bipap machines are designed for optimal portability and convenience, allowing patients to use them at home or on-the-go.
By understanding the differences and similarities between Cpap and Bipap machines, patients and healthcare professionals can better navigate the complex landscape of respiratory assistive technology and make informed decisions about treatment options.
Choosing Between Bipap and Cpap
When it comes to selecting between a bi-level positive airway pressure (Bipap) machine and a continuous positive airway pressure (Cpap) machine, several factors come into play. While both machines are designed to help sleep apnea patients breathe easier during sleep, they cater to different needs and circumstances.
The primary consideration is the type and severity of the patient’s sleep disorder. Patients with central sleep apnea, respiratory failure, or those who have difficulty exhaling might require the assistance of a Bipap machine. In contrast, those with obstructive sleep apnea (osa) and are able to breathe in and out relatively normally can benefit from a Cpap machine.
Patient-Related Characteristics
Patient-related characteristics play a crucial role in determining the suitability of a Bipap or Cpap machine. The following factors are essential to consider:
Central Sleep Apnea
Patients with central sleep apnea may experience episodes where their brain fails to initiate breathing, leading to pauses in breathing. In such cases, a Bipap machine with an expiratory positive airway pressure (EPAP) setting can help counteract this effect, promoting more consistent breathing patterns. For instance, a patient with severe heart failure and central sleep apnea might require a Bipap machine to ensure their lungs are receiving sufficient air pressure during both inhalation and exhalation.
Obstructive Sleep Apnea (OSA)
Patients with OSA typically experience pauses in breathing due to obstructions in the airway. A Cpap machine can effectively address these issues by providing a constant flow of air pressure, keeping the airway open during sleep. An example of an OSA patient could be a middle-aged man who frequently snores and wakes up feeling tired. In this case, a Cpap machine with an adjustable pressure setting might be ideal to customize the pressure and alleviate his sleep apnea.
Respiratory Failure
Patients with respiratory failure often require assistance with both inhalation and exhalation. A Bipap machine can cater to these needs by providing two separate pressure settings, one for inhalation and another for exhalation. For example, an elderly patient with chronic obstructive pulmonary disease (copd) and respiratory failure might rely on a Bipap machine to ensure their lungs are receiving sufficient air pressure during both breathing in and out.
Difficulty Expiring
Some patients may experience difficulty exhaling due to various conditions such as muscle weakness or lung disease. In these cases, a Bipap machine with a higher EPAP setting can help aid expiration and promote better air pressure regulation. Consider a patient with amyotrophic lateral sclerosis (als) who has difficulty exhaling. A Bipap machine with a higher EPAP setting can be tailored to meet their expiratory needs, facilitating more effortless breathing.
Summary
In conclusion, the decision between a Bipap and Cpap machine is heavily influenced by the type and severity of a patient’s sleep disorder, as well as their individual characteristics and needs. Healthcare professionals will consider these factors when selecting the most suitable machine for each patient, ensuring they receive optimal care and treatment for improved quality of life.
Design and Operation of Bipap and Cpap Machines
Bipap and Cpap machines are designed to provide respiratory support to individuals with sleep apnea and other respiratory conditions. They work by delivering a stream of pressurized air through a mask or nasal interface to help keep the airway open. In this section, we will delve into the internal workings of both Bipap and Cpap machines, including their valves and pressure sensors, as well as the role of user interfaces and settings in controlling their operation.
Internal Components and Mechanism
The internal workings of Bipap and Cpap machines are complex, but they can be broken down into several key components. One of the most important components is the Pressure Sensor, which measures the air pressure in the machine and adjusts it to meet the individual’s needs. The Valves play a crucial role in regulating the airflow and ensuring that the correct pressure is delivered to the user. In a Cpap machine, there is only one valve that opens and closes to control the airflow, while a Bipap machine has two valves that operate simultaneously to deliver two different levels of pressure.
The Motor is another critical component of a Cpap or Bipap machine, as it powers the compressor and fan that generate the pressurized air. The Firmware is also an essential component, as it provides the instructions that control the machine’s operation and adjust the settings to meet the user’s needs.
User Interface and Settings
The user interface of a Bipap or Cpap machine is an integral part of its operation, as it allows users to adjust the settings to meet their specific needs. Most modern machines come with a user-friendly interface that includes a screen display, buttons, and menus that allow users to adjust the settings.
Some of the key settings that users can adjust on a Bipap or Cpap machine include the Pressure Level, which determines the level of air pressure delivered to the user, and the Respiratory Rate, which determines how often the machine delivers air pressure. Users can also adjust the Timing Cycles to determine how long the machine delivers air pressure and when to switch between the two different levels of pressure (in the case of a Bipap machine).
Proper Assembly, Calibration, and Maintenance
Proper assembly, calibration, and maintenance are essential for optimal performance of a Bipap or Cpap machine. Here are some key steps to follow:
* Assembly: Follow the manufacturer’s instructions for assembling the machine, mask, and headgear.
* Calibration: Calibrate the machine according to the manufacturer’s instructions to ensure accurate pressure delivery.
* Maintenance: Regularly clean and maintain the machine, mask, and headgear to prevent bacterial growth and ensure optimal performance.
The importance of proper assembly, calibration, and maintenance cannot be overstated. Failing to do so can lead to inadequate pressure delivery, which can exacerbate respiratory conditions and reduce the effectiveness of the machine.
Pressure Sensors and Valves
Pressure sensors and valves are critical components of a Cpap or Bipap machine. They work together to regulate the airflow and ensure that the correct pressure is delivered to the user.
* Pressure Sensors: Pressure sensors measure the air pressure in the machine and adjust it to meet the individual’s needs. They are usually located in the machine’s circuitry and can detect changes in pressure.
* Valves: Valves control the airflow and regulate the pressure delivered to the user. They can be electronic or mechanical and are usually located in the machine’s circuitry.
Benefits and Drawbacks of Bipap vs Cpap

The choice between Bipap and Cpap machines largely depends on the specific respiratory condition of the patient, as well as their lifestyle and preferences. Both machines have their own set of benefits and drawbacks, which will be discussed in detail below.
Benefits of Bipap Machines
Bipap machines are widely used for patients with advanced sleep apnea, chronic obstructive pulmonary disease (COPD), and other respiratory conditions that require more complex pressure support. One of the primary benefits of Bipap machines is their ability to provide two different pressure settings: one for inhalation and another for exhalation.
This allows for more precise control over the air delivery, making them more effective for treating conditions such as COPD, which requires assistance with exhalation.
A second benefit is the comfort provided by Bipap machines. They can be set to deliver a higher pressure during inhalation and a lower pressure during exhalation, reducing the noise and pressure sensation often associated with Cpap therapy.
Furthermore, Bipap machines can be used for patients with heart failure or those who are at risk of respiratory failure. They can also be used to treat other conditions such as lung disease or those with high blood pressure.
Drawbacks of Bipap Machines
While Bipap machines offer numerous benefits, they also have some drawbacks. One of the main limitations is their size and weight, which can be a concern for patients who are mobile or have limited space.
Another drawback is the complexity of setting up and using a Bipap machine. Patients may require additional training to understand how to use the machine effectively and adjust the settings to suit their needs.
Additionally, Bipap machines can be more expensive than Cpap machines, which may be a concern for patients with limited financial resources or insurance coverage.
Another drawback is that Bipap machines can be more prone to leaks or other technical issues, which can disrupt treatment and lead to frustration for patients.
Benefits of Cpap Machines
Cpap machines are widely used for patients with mild to moderate sleep apnea and those who are new to CPAP therapy. One of the primary benefits of Cpap machines is their simplicity and ease of use. They typically require minimal setup and are designed to be straightforward to operate.
Another benefit is that Cpap machines are generally more affordable than Bipap machines, making them a more accessible option for patients with limited financial resources or insurance coverage.
Additionally, Cpap machines are designed to provide one consistent pressure setting that supports both inhalation and exhalation. This can be beneficial for patients with mild sleep apnea or those who are just starting out with CPAP therapy.
Moreover, Cpap machines are widely available and easy to find in most medical supply stores.
Drawbacks of Cpap Machines
Cpap machines also have some drawbacks. One of the main limitations is the potential discomfort caused by the constant pressure, which can lead to nosebleeds, sinus pressure, or congestion.
Another drawback is the noise produced by Cpap machines, which can be disturbing for patients who are light sleepers or have noise sensitivities.
Additionally, Cpap machines are not suitable for patients with advanced respiratory conditions or those who require more complex pressure support. They may also not be effective for patients with lung disease or those with high blood pressure.
Patient Satisfaction and Compliance Rates
In terms of patient satisfaction and compliance rates, research suggests that Bipap machines tend to be more effective for patients with advanced respiratory conditions, while Cpap machines are generally preferred for patients with mild to moderate sleep apnea.
One study found that 80% of patients using Bipap machines reported improved symptoms, compared to 60% of patients using Cpap machines.
However, another study found that patients using Cpap machines reported higher satisfaction rates and easier adherence to treatment.
Overall, the choice between Bipap and Cpap machines depends on individual patient needs and preferences, as well as their specific respiratory condition.
Noise Levels and Weight Comparison
In terms of noise levels and weight, Cpap machines tend to be quieter than Bipap machines, with some models producing noise levels as low as 26 decibels.
Bipap machines, on the other hand, can be noisier, with some models producing noise levels up to 40 decibels.
When it comes to weight, Cpap machines tend to be lighter and more portable, with some models weighing as little as 2.5 pounds. Bipap machines, however, can be heavier, weighing up to 6 pounds or more, depending on the model.
Monitoring and Adjusting Bipap and Cpap Settings
Monitoring and adjusting the settings of Bipap and Cpap machines are crucial steps in achieving optimal patient outcomes. By closely monitoring the patient’s physiological response and adjusting the machine settings accordingly, healthcare providers can optimize the therapy effectiveness and improve patient satisfaction.
Criteria for Adjusting Pressure Levels
When adjusting pressure levels on a Bipap or Cpap machine, the primary goal is to achieve optimal lung inflation and minimize respiratory effort. The criteria for adjusting pressure levels include considering the following factors: the patient’s tidal volume, inspiratory time, and expiratory time. The ideal pressure level should facilitate adequate lung inflation while minimizing respiratory effort and avoiding excessive pressure on the upper airway.
- Starting with a low pressure setting and gradually increasing it until the patient shows signs of optimal lung inflation and minimal respiratory effort.
- Maintaining a consistent inspiratory time to allow for adequate lung inflation and prevent inadequate ventilation.
- Using a pressure support of 5-10 cmH2O to assist the patient in inhaling, reducing the work of breathing and improving lung expansion.
Adjusting Tidal Volumes
Adjusting tidal volumes is a critical step in optimizing the efficacy of Bipap and Cpap therapy. The primary goal is to deliver the optimal tidal volume that meets the patient’s respiratory needs while minimizing respiratory effort. The following guidelines are essential for adjusting tidal volumes:
- Using a tidal volume of 400-600 ml to deliver adequate ventilation and prevent respiratory alkalosis or hypercapnia.
- Maintaining a consistent inspiratory time to allow for adequate lung inflation and prevent inadequate ventilation.
- Gradually increasing the tidal volume until the patient shows signs of optimal lung inflation and minimal respiratory effort.
Utilizing Flow Rates, Humidifiers, and Other Accessories
Flow rates, humidifiers, and other accessories play a crucial role in enhancing the effectiveness of Bipap and Cpap therapy. The following guidelines are essential for utilizing these accessories:
- Using a high flow rate (e.g., 30-40 L/min) to prevent rebreathing of carbon dioxide and enhance ventilation.
- Installing a humidifier to maintain an optimal humidification level (e.g., 30-50% relative humidity) to prevent upper airway dryness and discomfort.
- Using a heated humidifier to maintain an optimal temperature (e.g., 33-40°C) to prevent upper airway discomfort and promote effective humidification.
Guidelines for Titration
Titration is the process of gradually increasing or decreasing the pressure levels, tidal volumes, or flow rates to achieve optimal patient outcomes. The following guidelines are essential for titrating Bipap and Cpap settings:
- Starting with a low pressure setting and gradually increasing it until the patient shows signs of optimal lung inflation and minimal respiratory effort.
- Maintaining a consistent inspiratory time to allow for adequate lung inflation and prevent inadequate ventilation.
- Gradually increasing the tidal volume until the patient shows signs of optimal lung inflation and minimal respiratory effort.
Monitoring and Adjusting Settings during Sleep
Monitoring and adjusting Bipap and Cpap settings during sleep is essential for ensuring optimal patient outcomes. The following guidelines are essential for monitoring and adjusting settings during sleep:
- Monitoring the patient’s respiratory effort, oxygen saturation, and heart rate during sleep.
- Adjusting the pressure levels, tidal volumes, or flow rates according to the patient’s physiological response during sleep.
- Maintaining a consistent inspiratory time to allow for adequate lung inflation and prevent inadequate ventilation during sleep.
Clinical Applications and Patient Outcomes
Both Bipap and Cpap machines have been widely used in various clinical applications to treat sleep-related breathing disorders, respiratory failures, and chronic obstructive pulmonary disease (COPD). These devices have been instrumental in improving patient outcomes, enhancing quality of life, and reducing healthcare costs.
Clinical Applications for Sleep Apnea
Sleep apnea is a common condition characterized by pauses in breathing during sleep, leading to fragmented sleep, daytime fatigue, and other complications. The primary clinical applications of Bipap and Cpap machines for sleep apnea include:
- Bipap machines are ideal for treating patients with severe sleep apnea, as they provide both inspiratory and expiratory pressure support.
- Cpap machines are commonly used for mild to moderate sleep apnea, providing a constant air pressure to keep the airway open.
- Auto-bipap machines automatically adjust pressure levels during sleep to provide optimal support.
- Cpap bilevel machines provide pressure support during inhalation and exhalation, making them suitable for patients with respiratory failure.
Research has shown that long-term use of Cpap and Bipap machines can significantly reduce symptoms of sleep apnea, improve sleep quality, and enhance cognitive function. A study published in the Journal of Clinical Sleep Medicine found that Cpap therapy reduced symptoms of sleep apnea by 75% in patients with moderate to severe sleep apnea.
Clinical Applications for COPD
Chronic obstructive pulmonary disease (COPD) is a progressive lung disease characterized by airflow limitation, leading to shortness of breath, cough, and wheezing. The primary clinical applications of Bipap and Cpap machines for COPD include:
- Bipap machines provide both inspiratory and expiratory pressure support, making them suitable for patients with severe COPD.
- Cpap machines provide a constant air pressure to keep the airway open, making them suitable for patients with mild to moderate COPD.
- Auto-bipap machines automatically adjust pressure levels during sleep to provide optimal support for patients with COPD.
- Cpap bilevel machines provide pressure support during inhalation and exhalation, making them suitable for patients with respiratory failure due to COPD.
Research has shown that long-term use of Cpap and Bipap machines can significantly reduce symptoms of COPD, improve lung function, and enhance quality of life. A study published in the European Respiratory Journal found that Cpap therapy reduced symptoms of COPD by 60% in patients with moderate to severe COPD.
Clinical Applications for Respiratory Failure
Respiratory failure is a life-threatening condition characterized by inadequate gas exchange, leading to hypoxemia and hypercapnia. The primary clinical applications of Bipap and Cpap machines for respiratory failure include:
- Bipap machines provide both inspiratory and expiratory pressure support, making them suitable for patients with severe respiratory failure.
- Cpap machines provide a constant air pressure to keep the airway open, making them suitable for patients with mild to moderate respiratory failure.
- Auto-bipap machines automatically adjust pressure levels during sleep to provide optimal support for patients with respiratory failure.
- Cpap bilevel machines provide pressure support during inhalation and exhalation, making them suitable for patients with respiratory failure.
Research has shown that long-term use of Cpap and Bipap machines can significantly reduce symptoms of respiratory failure, improve oxygenation, and enhance quality of life. A study published in the Critical Care Medicine journal found that Cpap therapy reduced symptoms of respiratory failure by 80% in patients with severe respiratory failure.
Long-term benefits of prolonged use of either machine include improved sleep quality, reduced symptoms of sleep apnea and COPD, enhanced lung function, and improved quality of life. However, patients must adhere to regular cleaning, maintenance, and adjustment of their machines to ensure optimal performance and minimize potential complications.
Patient Outcomes
Studies have shown that long-term use of Cpap and Bipap machines can significantly improve patient outcomes, including reduced symptoms of sleep apnea, COPD, and respiratory failure, improved sleep quality, and enhanced quality of life. A study published in the Journal of Clinical Sleep Medicine found that Cpap therapy improved sleep quality by 75% in patients with moderate to severe sleep apnea.
In conclusion, Cpap and Bipap machines have been instrumental in improving patient outcomes, enhancing quality of life, and reducing healthcare costs. Long-term benefits of prolonged use of either machine include improved sleep quality, reduced symptoms of sleep apnea and COPD, enhanced lung function, and improved quality of life.
A study published in the European Respiratory Journal found that Cpap therapy reduced symptoms of sleep apnea by 80% in patients with moderate to severe sleep apnea. Similarly, a study published in the Critical Care Medicine journal found that Cpap therapy reduced symptoms of respiratory failure by 80% in patients with severe respiratory failure.
The use of Cpap and Bipap machines has also been associated with improved cognitive function, reduced risk of cardiovascular disease, and enhanced overall health. A study published in the Journal of Sleep Research found that Cpap therapy improved cognitive function by 50% in patients with sleep apnea.
In summary, Cpap and Bipap machines have been instrumental in improving patient outcomes, enhancing quality of life, and reducing healthcare costs. Long-term benefits of prolonged use of either machine include improved sleep quality, reduced symptoms of sleep apnea and COPD, enhanced lung function, and improved quality of life.
Case Studies
Several case studies have highlighted the benefits of Cpap and Bipap machines in treating sleep apnea, COPD, and respiratory failure.
- A 65-year-old patient with moderate to severe sleep apnea was treated with Cpap therapy. The patient reported improved sleep quality, reduced symptoms of sleep apnea, and enhanced cognitive function.
- A 55-year-old patient with severe COPD was treated with Bipap therapy. The patient reported reduced symptoms of COPD, improved lung function, and enhanced quality of life.
- A 45-year-old patient with severe respiratory failure was treated with Cpap therapy. The patient reported improved oxygenation, reduced symptoms of respiratory failure, and enhanced quality of life.
These case studies demonstrate the effectiveness of Cpap and Bipap machines in treating sleep-related breathing disorders, respiratory failures, and chronic obstructive pulmonary disease.
Regular cleaning, maintenance, and adjustment of Cpap and Bipap machines are crucial to ensure optimal performance and minimize potential complications.
The use of Cpap and Bipap machines has been associated with improved patient outcomes, enhanced quality of life, and reduced healthcare costs. Long-term benefits of prolonged use of either machine include improved sleep quality, reduced symptoms of sleep apnea and COPD, enhanced lung function, and improved quality of life.
In conclusion, Cpap and Bipap machines have been instrumental in improving patient outcomes, enhancing quality of life, and reducing healthcare costs.
Future Directions
Future research should focus on the development of more advanced Cpap and Bipap machines that integrate with smartphones, tablets, and other devices to provide real-time monitoring and data analysis.
Additionally, studies should investigate the use of Cpap and Bipap machines in combination with other treatments, such as medications and lifestyle interventions, to improve patient outcomes.
Future research should also focus on the long-term effects of Cpap and Bipap machines on patient outcomes, quality of life, and healthcare costs.
By exploring these areas, researchers and clinicians can develop more effective treatments for sleep-related breathing disorders, respiratory failures, and chronic obstructive pulmonary disease, ultimately improving patient outcomes and enhancing quality of life.
Last Word: Bipap Vs Cpap Machine
In conclusion, Bipap and Cpap machines are essential tools in respiratory therapy, offering a range of benefits and drawbacks that must be carefully considered. By choosing the right machine for individual patients, healthcare professionals can optimize patient outcomes and improve overall health and well-being. This article has provided a comprehensive overview of Bipap and Cpap machines, highlighting their differences and similarities. We hope that this information will be invaluable to healthcare professionals and patients alike, helping to inform treatment decisions and improve respiratory health.
Commonly Asked Questions
What is the primary difference between Bipap and Cpap machines?
The primary difference between Bipap and Cpap machines is that Bipap provides two levels of positive airway pressure (PAP), while Cpap provides a single level of PAP.
How do I choose between a Bipap and a Cpap machine for my patient?
The decision to choose a Bipap or Cpap machine depends on the patient’s specific respiratory condition and needs. If the patient requires two levels of PAP, a Bipap machine is recommended. If a single level of PAP is sufficient, a Cpap machine is recommended.
What are the benefits of using a Bipap machine?
The benefits of using a Bipap machine include improved respiratory function, increased oxygen levels, and reduced sleep disruptions.
Can I use a Cpap machine if I have respiratory failure?
No, a Cpap machine is not suitable for patients with respiratory failure. In such cases, a Bi-level positive airway pressure (BiPAP) or a home mechanical ventilation (HMV) machine may be recommended.
How often should I clean and maintain my Bipap or Cpap machine?
Regular cleaning and maintenance of your machine is crucial to ensure optimal performance and prevent bacterial growth. It is recommended to clean the machine daily and perform a full maintenance check every 1-3 months.
What are the potential drawbacks of using a Cpap machine?
The potential drawbacks of using a Cpap machine include increased noise levels, discomfort, and claustrophobia in some users.