Delving into breathing machines in hospitals, this technology plays a vital role in saving lives by providing oxygen and support to patients in need. In this comprehensive overview, we will explore the various types of breathing machines, their mechanisms, functions, and clinical applications.
The complexity and importance of breathing machines in hospitals demand a thorough understanding of their operation and maintenance. From the basics of oxygenation and ventilation to the advanced settings and troubleshooting techniques, our guide will walk you through the ins and outs of breathing machines, providing you with a solid foundation for working with these life-saving devices.
Overview of Breathing Machines in Hospitals
In sterile halls of hospitals, where hope and despair entwine,
Lies a life-supporting marvel, a breathing machine divine.
Its purpose clear, its functionality refined,
To assist fragile lungs, and give life a second shine.
Main Purpose and Functionality
Breathing machines, also known as ventilators or respirators,
Are sophisticated devices, designed to breathe for those who cannot.
Their main purpose is to provide oxygen and remove carbon dioxide,
Aiding patients with respiratory failure, or those recovering from surgery.
These machines work by creating positive pressure in the lungs,
Forcing air to enter and exit, simulating a natural breath.
They can be adjusted to meet individual needs,
From slow, gentle breaths, to rapid, life-saving interventions.
In hospitals, breathing machines are a crucial tool,
For Intensive Care Unit (ICU) patients, where every second counts.
They help manage conditions, such as pneumonia,
Severe asthma, or spinal cord injuries.
Types of Breathing Machines
There are various types of breathing machines available,
Tailored to specific needs, and patient conditions.
- Ventilators: These machines provide mechanical ventilation,
Supporting patients with respiratory failure, or those who require assistance breathing.
They can be used in ICUs, emergency departments, or ward settings. - Respirators: These devices combine ventilation with oxygen therapy,
Delivering a specific mixture of gases, tailored to each patient’s needs.
They are often used for patients with chronic respiratory conditions,
Such as COPD, or those requiring long-term oxygen therapy. - Portable Ventilators: These machines are compact,
Designed for patients who need ventilation outside of a hospital setting.
They can be used in ambulances, or at home, allowing for more flexible care.
These breathing machines are designed to support,
And sometimes save, the lives of those who need it most.
Their importance cannot be overstated,
In the critical care of patients, where every moment counts.
Mechanisms and Components of Breathing Machines
With delicate precision, breathing machines orchestrate life-giving oxygenation, soothing the afflicted lungs of patients, suspended between fate and salvation.
Beneath their metallic skin, subtle mechanisms hum with the promise of resuscitation, their intricacies woven from the threads of innovation and human ingenuity.
The Process of Oxygenation and Ventilation
Within the realm of breathing machines, oxygenation and ventilation form the delicate balance upon which life hangs. Oxygenation is the process of adding oxygen to the breath, while ventilation pertains to the movement of air in and out of the lungs. These processes occur simultaneously, with the machine delicately modulating the proportions. It is a dance, where oxygen and carbon dioxide are exchanged in a gentle ballet, orchestrated so that the delicate balance of the patient’s physiology is preserved.
Key Components of Breathing Machines
Sensory awareness is the precursor to healing in a breathing machine. Sensory inputs inform the control systems that regulate the machines’ behavior, allowing for responsive and adaptive adjustments to meet the dynamic needs of patients. Alarms alert caregivers to emerging threats to the patient’s respiratory stability, a clarion call for immediate action in high-pressure situations. Control systems provide the central nervous system of breathing machines, integrating and orchestrating the functions, ensuring the machine is in harmony with the patient.
The delicate interplay between these components is the very essence of breathing machines’ functionality.
Types of Breathing Machine Modes, Breathing machines in hospitals
A wide range of breathing machine modes exist to suit the unique requirements of each patient. Volume-control mode and pressure-control mode are among the most commonly used modes in hospitals. In volume-control mode, the amount of volume in the breath is set by the machine; in pressure-control mode, the pressure of the breath is predetermined, allowing for varying volumes to be achieved. Both modes are vital tools, offering flexibility and precision in the delicate dance of oxygenation and ventilation.
Clinical Use and Applications of Breathing Machines

In the dimly lit corridors of hospitals, where hope and despair coexist, breathing machines stand as beacons of life. Their clinical use and applications are a testament to human ingenuity in the face of adversity. These machines have revolutionized the treatment of respiratory failure, cardiac arrest, and other life-threatening conditions, giving patients a second chance at life.
Clinical Indications
Breathing machines are employed in various clinical scenarios, including respiratory failure and cardiac arrest. Respiratory failure, a life-threatening condition characterized by inadequate oxygenation or ventilation, is a primary indication for the use of breathing machines. In cardiac arrest, breathing machines play a crucial role in maintaining oxygenation and perfusion of vital organs until cardiac function can be restored.
Breathing machines are also used in the treatment of chronic obstructive pulmonary disease (COPD), asthma, and pneumonia. In these cases, the machines help to alleviate symptoms, improve oxygenation, and prevent further complications.
Methods for Weaning Patients
Weaning patients from breathing machines is a critical step in their recovery. The process involves gradually reducing the support provided by the machine, allowing the patient to take over their breathing. Two common methods used for weaning patients are spontaneous breathing trials and T-piece weaning.
Spontaneous breathing trials involve disconnecting the patient from the breathing machine and allowing them to breathe on their own for a short period. This trial is repeated several times to assess the patient’s ability to sustain breathing. If successful, the patient may be weaned off the breathing machine permanently.
T-piece weaning, on the other hand, involves using a T-piece device to gradually reduce the support provided by the breathing machine. The T-piece device delivers a low level of oxygen and pressure, allowing the patient to breathe more easily.
Importance of Proper Patient Selection and Monitoring
Proper patient selection and monitoring are essential when using breathing machines in clinical practice. Patients who are critically ill, have chronic respiratory disease, or are undergoing surgery may require close monitoring and adjusting of breathing machine settings.
Regular assessments of patient vital signs, lung function, and oxygenation levels are crucial to prevent complications and ensure optimal outcomes. Clinicians must also consider the patient’s overall condition, including their mental status, pain levels, and mobility.
Assessment of Patient Readiness for Weaning
Assessing patient readiness for weaning from breathing machines is a critical step in their recovery. A patient’s readiness to be weaned is determined by their ability to breathe on their own, maintain adequate oxygenation, and sustain adequate ventilation.
Some of the factors that are assessed include:
– Ability to maintain adequate oxygenation
– Ability to sustain adequate ventilation
– Ability to breathe on their own without the need for support
– Presence of underlying respiratory or cardiac disease
– Presence of other comorbidities
– Patient’s overall condition and mental status
Regular assessments of patient readiness for weaning are crucial in preventing complications and ensuring optimal outcomes.
Complications of Breathing Machines
While breathing machines are lifesaving devices, they can also cause complications. Some of the common complications associated with breathing machines include:
– Ventilator-associated pneumonia
– Barotrauma and lung injury
– Cardiac arrhythmias and decreased cardiac output
– Anemia and decreased oxygen-carrying capacity
Patients with underlying respiratory or cardiac disease are at a higher risk of developing complications. Regular monitoring and adjusting of breathing machine settings can help mitigate the risk of complications.
Maintenance and Troubleshooting of Breathing Machines: Breathing Machines In Hospitals
In the realm of life-giving machines, breathing machines stand as steadfast guardians of patients’ airways. Their precision and reliability rely heavily on regular maintenance, a vital task that ensures the machines continue to function as they should, providing the life-sustaining air that patients require. Maintenance and troubleshooting form an integral duo, ensuring that these vital machines operate with ease and efficiency, never faltering in their duty to preserve life.
Regular maintenance keeps breathing machines in optimal condition, preventing potential breakdowns and malfunctions that could harm patients. Calibrating the machines, cleaning the internal components, and checking their functionality all contribute to a robust maintenance routine. Like a skilled musician tuning his instrument, maintenance workers carefully balance the delicate elements, adjusting the settings to achieve harmonious operation. They inspect and service various components, including sensors, valves, and motors, to guarantee the machine’s ability to breathe for patients.
Cleaning and Calibration
Maintenance is not a one-and-done task, but rather a continuous process. Breathing machines require regular cleaning to prevent the buildup of dirt, bacteria, and other contaminants that could compromise patient safety. Cleaning involves disinfecting all exposed surfaces, replacing any disposable components, and checking for signs of damage or wear. Calibrating the machines ensures accuracy in their airflow and oxygen levels, guaranteeing patients receive the precise oxygenation their bodies require.
Maintainers must adhere to strict cleaning protocols to eliminate bacteria and other microorganisms that can infect patients. This involves thorough disinfection of all parts, from the external casing to the delicate tubes and valves. Proper cleaning helps maintain the machine’s integrity, ensuring it remains a safe haven for patients in need.
Troubleshooting Steps
Troubleshooting steps serve as the vital backup to maintenance, helping address any technical issues that may arise with breathing machines. Alarm activation signals a need for urgent attention, as malfunctions can quickly escalate into crises. Sensor failure presents a pressing challenge, as these vital components monitor critical parameters, such as oxygen levels and patient airflow. Troubleshooting requires patience and expertise, as professionals must carefully diagnose the issue, isolate the cause, and implement a solution.
When an alarm sounds, technicians swiftly activate their troubleshooting skills, checking the machine for signs of error. They meticulously evaluate sensor readings, monitor the machine’s performance, and inspect its components. If a sensor fails, maintenance personnel must quickly identify the cause, often requiring extensive technical knowledge and experience.
Importance of Regular Maintenance and Troubleshooting
Maintenance and troubleshooting stand as inseparable partners, working in tandem to keep breathing machines in top working order. Both tasks are essential for ensuring proper functioning, guaranteeing patients receive life-sustaining oxygen. Regular maintenance eliminates potential breakdowns, while troubleshooting steps rapidly address issues when they arise, safeguarding patient health.
Proper maintenance and troubleshooting also help breathe new life into these machines, extending their lifespan and reducing the need for costly repairs. By preventing malfunctions and quickly addressing technical issues, medical technicians safeguard patients’ well-being and ensure that breathing machines continue to deliver the air patients need.
Training and Education for Healthcare Providers
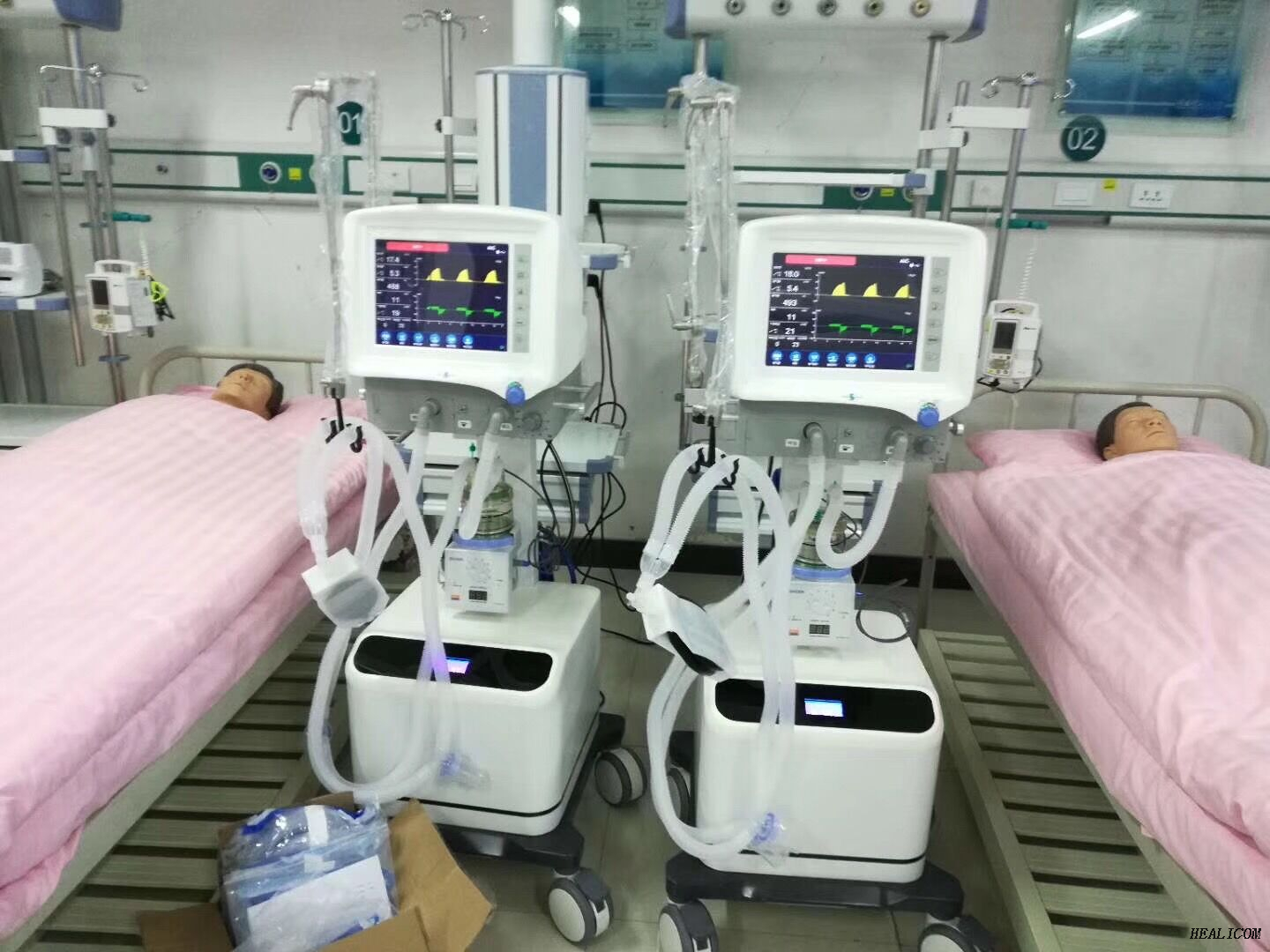
In the realm of medical care, where the delicate balance of life hangs in the balance, the healthcare providers who wield the mighty breathing machines must be prepared to face the challenge. A comprehensive training and education program lays the foundation for competence, as healthcare providers learn to navigate the complexities of life-sustaining technology. As the medical landscape evolves, so too must the training of those who operate within it.
The education of healthcare providers operating breathing machines requires a multifaceted approach, one that addresses both theoretical and practical aspects of their use. A thorough understanding of the underlying physiology, mechanics, and clinical applications of breathing machines is essential for delivering effective care. This foundational knowledge serves as the bedrock upon which healthcare providers can build their skills, allowing them to respond to the unique needs of their patients with confidence and precision.
The Importance of Hands-On Training and Simulation
The art of operating breathing machines demands a level of proficiency that cannot be achieved solely through theoretical knowledge. Hands-on training and simulation allow healthcare providers to develop the essential skills required to operate these complex devices, ensuring a seamless transition from education to practice. By immersing themselves in the simulated environment, healthcare providers can refine their techniques, anticipate challenges, and cultivate the instincts necessary to respond to critical situations.
Ongoing Education and Support
The journey to expertise is far from over once initial training is complete. The dynamic nature of medical technology necessitates ongoing education and support, allowing healthcare providers to stay abreast of the latest advancements, guidelines, and best practices. Regular updates, workshops, and peer-to-peer discussions enable healthcare providers to maintain their proficiency, address questions, and learn from one another’s experiences. This collective effort yields a more efficient, effective, and compassionate care environment, ultimately improving patient outcomes.
Key Training Components
The comprehensive training program for healthcare providers operating breathing machines should include, but not be limited to:
- Foundational knowledge of respiratory physiology, anesthesia, and critical care medicine.
- Hands-on training on a range of breathing machine models and variants.
- Simulation exercises to practice responding to various patient scenarios and system malfunctions.
- Ongoing education and updates on device maintenance, troubleshooting, and best practices.
- Mentorship and peer-to-peer interaction to foster collaboration and knowledge sharing.
Simulation-Based Training
Simulation-based training enables healthcare providers to develop the skills and confidence needed to operate breathing machines in high-stakes situations. By replicating various clinical scenarios, training programs can teach participants to respond effectively to complex situations, fostering a culture of preparedness and competence. The simulation environment allows healthcare providers to learn from mistakes, develop decision-making strategies, and refine their crisis management skills.
Expert-Led Workshops
Expert-led workshops and conferences provide healthcare providers with a wealth of knowledge and experience. Renowned specialists in the field share the latest research, guidelines, and best practices, empowering healthcare providers to deliver exceptional care. By engaging with international experts and peers, healthcare providers can remain informed, inspired, and connected to the global medical community.
Fostering a Culture of Continuous Learning
Healthcare providers operating breathing machines must remain vigilant, committed to ongoing learning and self-improvement. By embracing a culture of continuous learning, they can remain at the forefront of medical advancements, responding to the evolving needs of their patients with confidence and compassion. This dedication to education and expertise has a profound impact on patient care, fostering a safer, more efficient, and more effective healthcare environment.
End of Discussion

As we conclude our exploration of breathing machines in hospitals, it’s clear that these tools are crucial in providing top-notch care and ensuring patient comfort and safety. By understanding the ins and outs of these machines, healthcare professionals can make informed decisions and provide exceptional care to those in need.
FAQ Compilation
What is the primary function of a breathing machine in a hospital?
To provide patients with oxygen and mechanical ventilation support when they are unable to breathe on their own.
What is the difference between a ventilator and a respirator?
While both machines provide breathing support, ventilators are used for long-term oxygenation, and respirators are used for short-term ventilation.
What are some common safety features found on breathing machines?
Alarm systems, oxygen sensors, and fail-safe mechanisms are designed to prevent accidents and ensure patient safety.