Congestive heart failure restored machine sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail with formal but funny style and brimming with originality from the outset. It’s a device that has the potential to revolutionize the treatment of congestive heart failure, a condition that affects millions worldwide.
The congestive heart failure restored machine is a relatively new technology that uses mechanical circulatory support devices to restore heart function. These devices are designed to take over the pumping role of the heart, allowing it to recover and function properly once again.
Congestive Heart Failure Restored Machine: A Game-Changer in Medical Treatment

The congestive heart failure restored machine, also known as a ventricular assist device (VAD), is a revolutionary medical device designed to support the heart’s pumping function in patients with advanced congestive heart failure (CHF). CHF is a chronic condition characterized by the heart’s inability to pump enough blood to meet the body’s needs, leading to fatigue, shortness of breath, and swelling in the legs and feet. The Congestive Heart Failure Restored Machine plays a crucial role in improving the quality of life for patients with CHF by enhancing their heart function and reducing symptoms.
Current State of Technology and Research
Researchers and scientists have been actively working to develop and improve the congestive heart failure restored machine, driven by the growing need for effective treatments for CHF. According to the American Heart Association, more than 6 million Americans suffer from heart failure, and this number is projected to increase due to the aging population and the rising prevalence of obesity, diabetes, and high blood pressure. Advances in technology and materials science have led to the development of smaller, more efficient, and easier-to-use VADs, making them more accessible to patients.
- Advances in Miniaturization and Portability
- Development of New Materials and Designs
- Integration of Artificial Intelligence and Automation
These advancements have enabled the congestive heart failure restored machine to become a more reliable and effective treatment option for patients with CHF. Studies have shown that VAD therapy can improve survival rates, reduce hospitalizations, and enhance quality of life in patients with advanced heart failure.
Key Components of the Congestive Heart Failure Restored Machine
The congestive heart failure restored machine consists of several key components, including a pump, a controller, and a driveline. The pump is responsible for augmenting the heart’s pumping function, while the controller regulates the pump’s operation to ensure efficient and safe blood flow. The driveline connects the pump to the controller and allows for precise control over the pump’s speed and function.
| Component | Description |
|---|---|
| Pump | Responsible for augmenting the heart’s pumping function |
| Controller | Regulates the pump’s operation to ensure efficient and safe blood flow |
| Driveline | Connects the pump to the controller and allows for precise control over the pump’s speed and function |
The congestive heart failure restored machine also features advanced safety features, such as automatic shut-off in the event of electrical malfunction or power failure, and a built-in alarm system to alert the patient and healthcare provider to any potential issues.
Impact of the Congestive Heart Failure Restored Machine on Patient Outcomes
Studies have consistently shown that the congestive heart failure restored machine can significantly improve patient outcomes, including reduced hospitalizations, improved survival rates, and enhanced quality of life. According to a study published in the Journal of the American College of Cardiology, VAD therapy resulted in a 45% reduction in mortality rates and a 50% reduction in hospitalizations in patients with advanced heart failure.
“The congestive heart failure restored machine is a game-changer in the treatment of congestive heart failure. It has revolutionized the way we manage this condition, providing patients with a second chance at life and improving their quality of life.”
Types of Congestive Heart Failure Restored Machines
The development of devices to restore congestive heart failure has revolutionized the treatment of cardiac patients. There are various types of machines used to treat congestive heart failure, each with its own advantages and disadvantages.
Mechanical Circulatory Support Devices
Mechanical circulatory support devices are external machines that can take over the function of the heart, providing blood circulation to the body. These devices are typically used in patients with advanced heart failure who require mechanical support to sustain life.
- Left Ventricular Assist Device (LVAD): An LVAD is a type of mechanical circulatory support device that is placed in the chest and connected to the left ventricle of the heart. It pumps blood from the heart to the rest of the body.
- Right Ventricular Assist Device (RVAD): An RVAD is a type of mechanical circulatory support device that is placed in the chest and connected to the right ventricle of the heart. It pumps blood from the heart to the lungs.
- Biventricular Assist Device (BVPD): A BVPD is a type of mechanical circulatory support device that is placed in the chest and connected to both the left and right ventricles of the heart. It pumps blood from the heart to the rest of the body and to the lungs.
The advantages of mechanical circulatory support devices include reduced mortality and improved quality of life for patients with advanced heart failure. However, they also have several disadvantages, including the need for continuous hospitalization and mechanical support, the risk of bleeding and infection, and the potential for device failure.
Implantable devices are tiny machines that are surgically inserted into the body to treat congestive heart failure. These devices are typically used in patients with mild to moderate heart failure.
- Pacemaker: A pacemaker is an implantable device that is used to regulate the heartbeat of patients with slow heart rates. It sends electrical impulses to the heart to stimulate contractions.
- Cardioverter-Defibrillator (ICD): An ICD is an implantable device that is used to monitor and regulate the heartbeat of patients with abnormal heart rhythms. It sends electrical impulses to the heart to correct irregular rhythms and prevent sudden cardiac death.
- Resynchronization Therapy (CRT): CRT is an implantable device that is used to synchronize the heartbeat of patients with abnormal heart rhythms. It sends electrical impulses to the left and right ventricles to coordinate contractions.
The advantages of implantable devices include reduced risk of device failure, improved quality of life, and lower cost compared to mechanical circulatory support devices. However, they also have several disadvantages, including the need for surgical implantation, the risk of battery depletion, and the potential for device malfunction.
Internal Cardiac Assist Devices (ICADs) are tiny machines that are surgically inserted into the heart to treat congestive heart failure. These devices are typically used in patients with end-stage heart failure.
- Tahitian Heart Assist Device: The Tahitian Heart Assist Device is an ICAD that is surgically inserted into the heart to pump blood from the heart to the rest of the body. It is designed to be a semi-permanent solution for patients with end-stage heart failure.
- Micro-AX
The advantages of internal cardiac assist devices include reduced need for hospitalization, lower risk of device failure, and improved quality of life. However, they also have several disadvantages, including the need for surgical implantation and the potential for device malfunction.
Components and Mechanics of Congestive Heart Failure Restored Machines
The design of congestive heart failure restored machines (CHFRMs) involves a sophisticated interplay of various components, including pumps, valves, and sensors. These components work together to restore heart function by mimicking the natural pumping actions of the heart, regulating blood flow, and monitoring the patient’s condition in real-time. Understanding the mechanics of these components is crucial in elucidating the inner workings of CHFRMs.
Pumps
The most critical component of CHFRMs is the pump, responsible for simulating the heart’s pumping action. There are two primary types of pumps used in CHFRMs: ventricular assist devices (VADs) and total artificial hearts (TAHs). VADs support the left or right ventricle, whereas TAHs replace both ventricles.
– Ventricular Assist Devices (VADs): VADs are implantable pumps that assist the natural pumping action of the heart, either the left or right ventricle. They are connected to the heart and the aorta (for the left ventricle) or the pulmonary artery (for the right ventricle).
* Left Ventricular Assist Devices (LVADs): LVADs are used to support or replace the left ventricle, bypassing the natural pump. They ensure that the aorta receives adequate blood flow.
* Right Ventricular Assist Devices (RVADs): RVADs assist the right ventricle, preventing blood buildup in the lungs by pumping blood into the pulmonary artery.
Valves
Valves play a crucial role in regulating blood flow within CHFRMs. They are designed to mimic the natural valves found in the heart, ensuring that blood flows in one direction and preventing backflow.
– Tissue Valves: These valves are made from natural or synthetic tissues that resemble the heart’s native tissue valves.
– Mechanical Valves: Mechanical valves utilize a combination of materials like titanium and polyurethane to achieve precise control of blood flow.
Sensors
Sensors are integral to the CHFRM, monitoring vital signs and the patient’s condition in real-time. These sensors include:
– Electrocardiogram (ECG) Sensors: ECG sensors track the patient’s heart activity, providing data on heart rate and rhythm.
– Pulse Oximetry Sensors: These sensors measure oxygen saturation levels in the patient’s blood.
– Thrombolytic Sensors: Thrombolytic sensors detect blood clots or thrombi within the machine’s components.
Comparison of Congestive Heart Failure Restored Machines with Other Treatments
The treatment of Congestive Heart Failure (CHF) requires a comprehensive approach, and various options have been explored to provide relief to patients. Among these, Congestive Heart Failure Restored Machines have emerged as a promising solution. However, like any other treatment, they have their own advantages and disadvantages, which are necessary to consider when deciding on the best course of action.
Medications for Congestive Heart Failure
Medications play a crucial role in the management of CHF, and various classes of drugs have been developed to tackle the condition. These include diuretics, ACE inhibitors, beta-blockers, and vasodilators. Each class of medication has its unique benefits and drawbacks, and they are often used in combination to achieve optimal results.
* Diuretics help to remove excess fluid from the body, reducing congestion and shortness of breath.
* ACE inhibitors and beta-blockers work by relaxing blood vessels and reducing the workload on the heart, allowing it to pump more efficiently.
* Vasodilators help to dilate blood vessels, reducing the resistance against which the heart must pump.
Surgical Interventions for Congestive Heart Failure
In more severe cases, surgery may be necessary to alleviate symptoms and improve the heart’s function. Surgical options include coronary artery bypass grafting, heart transplantation, and ventricular assist device (VAD) implantation. Each of these procedures has its own set of risks and benefits, and they are typically reserved for patients who have not responded to other treatments.
* Coronary artery bypass grafting involves rerouting blood flow around blocked arteries to improve blood supply to the heart muscle.
* Heart transplantation involves replacing the diseased heart with a healthy one, obtained from a donor.
* VAD implantation involves installing an artificial pump to take over the heart’s pumping function, giving the natural heart time to recover.
Comparison of Treatments
Each treatment option for CHF has its unique advantages and disadvantages. Medications can be effective in managing symptoms and slowing disease progression, but they may not be sufficient for patients with advanced disease. Surgical interventions can offer more significant benefits, but they are often associated with higher risks and may not be suitable for all patients.
| Treatment | Advantages | Disadvantages |
| — | — | — |
| Medications | Effective in managing symptoms | May not be sufficient for advanced disease |
| Surgical Interventions | Can offer more significant benefits | Associated with higher risks, not suitable for all patients |
Congestive Heart Failure Restored Machines, on the other hand, offer a new approach to treating the condition. By restoring cardiac function and improving overall health, they have the potential to revolutionize CHF treatment. However, more research is needed to fully understand their benefits and limitations, and they may not be appropriate for all patients.
Future Directions and Challenges: Congestive Heart Failure Restored Machine
The congestive heart failure restored machine has revolutionized the medical treatment for heart failure patients. As this technology continues to evolve, it is essential to explore its future directions and challenges. The advancements in this field are expected to improve the lives of millions of people worldwide, but there are several obstacles that need to be addressed.
Advancements in Artificial Intelligence and Machine Learning
Artificial intelligence (AI) and machine learning (ML) are expected to play a crucial role in the development of congestive heart failure restored machines. AI algorithms can analyze patient data, predict disease progression, and optimize treatment plans. ML models can learn from large datasets and improve the accuracy of predictions. The integration of AI and ML can lead to more personalized treatment plans, improved patient outcomes, and reduced healthcare costs.
AI can help in developing predictive models that can identify high-risk patients and prevent hospitalizations.
Development of Biocompatible Materials
The development of biocompatible materials is essential for the creation of safe and effective congestive heart failure restored machines. Researchers are working on developing materials that can mimic the properties of natural tissues, reducing the risk of adverse reactions and improving device durability. Biodegradable materials, such as polylactic acid (PLA) and polyglycolic acid (PGA), are being explored as potential solutions for implantable devices.
Imaging and Monitoring Technologies
Advanced imaging and monitoring technologies are necessary for the proper functioning of congestive heart failure restored machines. Real-time monitoring systems can track device performance, patient vital signs, and detect potential complications. Imaging modalities like MRI, CT, and ultrasound can provide valuable insights into the cardiac structure and function. The development of smaller, more portable devices and sensors can enhance patient mobility and reduce hospitalizations.
Challenges and Obstacles
Despite the progress made in congestive heart failure restored machine technology, several challenges and obstacles need to be overcome. The high cost of these devices, limited availability, and potential complications are major concerns. Additionally, there is a need for standardization and regulatory frameworks to ensure patient safety and device efficacy.
Moreover, the development of training programs and education initiatives for healthcare professionals is essential for the widespread adoption of congestive heart failure restored machines.
Addressing Ethical and Social Implications
The use of congestive heart failure restored machines raises several ethical and social implications. The allocation of limited resources, patient selection criteria, and informed consent processes need to be carefully addressed. The long-term implications of these devices on patient quality of life, healthcare costs, and societal values also require consideration.
International Collaboration and Standardization
The global nature of congestive heart failure restored machine technology requires international collaboration and standardization. Regulatory agencies, research institutions, and industry leaders must work together to establish common standards, promote knowledge sharing, and facilitate the development of new technologies.
Patient Selection and Management
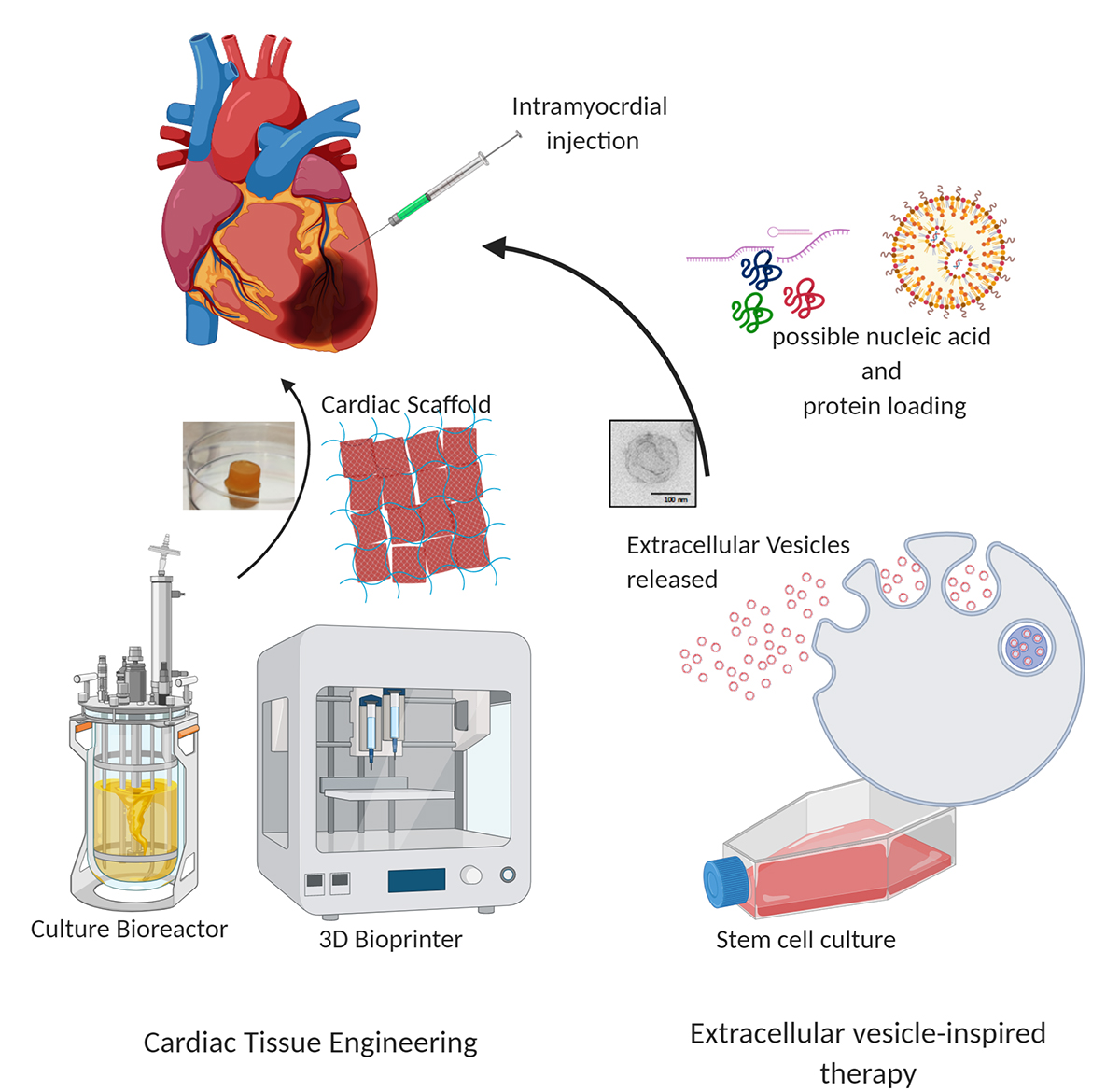
Patient selection and management are crucial aspects of congestive heart failure restored machine treatment. The effectiveness of this treatment depends on identifying the right patients and providing proper care to ensure optimal outcomes. The primary objective is to select patients who will benefit from this treatment and manage their care to prevent complications and improve quality of life.
Criteria for Selecting Patients
The criteria for selecting patients for congestive heart failure restored machine treatment should be based on a comprehensive evaluation of the patient’s medical history, diagnosis, and current condition. The following factors should be considered:
- Diagnosis of congestive heart failure (CHF) with a clear understanding of the underlying cause, such as coronary artery disease, dilated cardiomyopathy, or hypertrophic cardiomyopathy.
- NYHA functional class II-IV, indicating moderate to severe symptoms limiting physical activity and daily life.
- LV ejection fraction (LVEF) <40% indicating significant left ventricular dysfunction.
- Right ventricular dysfunction or septal dysfunction.
- Presence of arrhythmias, such as atrial fibrillation or ventricular tachycardia.
- History of heart failure hospitalizations or emergency department visits within the past year.
- Age between 40-80 years, although age can be a limiting factor in certain cases.
- Body mass index (BMI) >25 kg/m2, indicating obesity, which can complicate treatment outcomes.
Importance of Proper Patient Management and Follow-up Care
Proper patient management and follow-up care are essential to optimize the effectiveness of congestive heart failure restored machine treatment. This involves:
- Close monitoring of cardiac function, renal function, and electrolyte levels to prevent complications.
- Optimization of medication regimens to minimize side effects and maximize benefits.
- Implementation of lifestyle modifications, such as diet and exercise programs, to promote overall health and well-being.
- Counseling on the risks and benefits of the treatment, as well as potential complications and adverse events.
- Regular follow-up appointments to assess treatment efficacy and address any concerns or questions the patient may have.
“Patient-centered care is a critical component of congestive heart failure restored machine treatment, emphasizing the importance of empathy, communication, and shared decision-making between the healthcare provider and the patient.”
Management of Complications and Adverse Events
Management of complications and adverse events is crucial in congestive heart failure restored machine treatment. The following measures should be taken:
- Close monitoring of cardiac function, renal function, and electrolyte levels to prevent complications.
- Optimization of medication regimens to minimize side effects and maximize benefits.
- Implementation of lifestyle modifications, such as diet and exercise programs, to promote overall health and well-being.
- Counseling on the risks and benefits of the treatment, as well as potential complications and adverse events.
- Regular follow-up appointments to assess treatment efficacy and address any concerns or questions the patient may have.
Risk Factors and Complications
Congestive heart failure restored machines, like any other medical device, carry potential risks and complications that must be carefully considered by healthcare professionals and patients. In this section, we will discuss the risk factors and potential complications associated with these machines, as well as strategies for mitigating these risks.
Risk Factors Asssociated with Congestive Heart Failure Restored Machines
The risk factors associated with congestive heart failure restored machines can be broadly categorized into several groups, including surgical risks, complications related to the device itself, and post-operative risks. These risk factors can be further broken down into the following categories:
- Surgical Risks: These risks are associated with the surgical procedure required to implant the machine, including bleeding, infection, and damage to surrounding tissues. In addition, there may be risks associated with the anesthesia used during the procedure.
- Device-Related Complications: These complications can arise from the design or manufacturing of the device itself, including malfunctions, mechanical failures, and problems with the device’s electrical components. In some cases, device-related complications can lead to serious health consequences, including stroke, heart attack, or even death.
- Post-Operative Risks: These risks are associated with the recovery period following the implantation of the device, including pain, discomfort, swelling, and bleeding at the surgical site. In addition, there may be risks associated with the use of antibiotics and other medications during the recovery period.
- Bleeding and Hematoma: Bleeding and hematoma are potential complications associated with the surgical procedure, particularly when the machine is implanted in the chest cavity. In some cases, bleeding can lead to serious health consequences, including cardiac arrest or even death.
- Arrhythmias: Arrhythmias, or irregular heartbeats, can occur as a result of the machine’s electrical stimulation. In some cases, arrhythmias can be severe enough to require immediate medical attention.
- Device malfunction: Device malfunction can occur due to a variety of factors, including mechanical failure, electrical malfunction, or software issues. In some cases, device malfunction can lead to serious health consequences, including stroke, heart attack, or even death.
Strategies for Mitigating the Risks and Complications
While the risks and complications associated with congestive heart failure restored machines can be significant, there are steps that healthcare professionals and patients can take to mitigate these risks. These strategies include:
- Selecting a suitable candidate: The decision to implant a congestive heart failure restored machine should be made on a case-by-case basis, taking into account the patient’s medical history, overall health, and lifestyle.
- Proper device maintenance: Regular maintenance and check-ups are essential to prevent device malfunction and ensure optimal device performance.
- Adherence to medication regimens: Patients must adhere to their medication regimens to prevent complications and ensure optimal device performance.
- Following post-operative instructions: Patients must carefully follow their healthcare provider’s instructions following the surgical procedure to minimize the risk of complications and ensure optimal recovery.
- Regular monitoring and follow-up: Regular monitoring and follow-up appointments with the healthcare provider are essential to detect any potential complications early and prevent serious health consequences.
Reducing the Risk of Bleeding and Hematoma, Congestive heart failure restored machine
Bleeding and hematoma are significant risks associated with congestive heart failure restored machines. However, there are steps that healthcare professionals and patients can take to reduce the risk of these complications. These strategies include:
- Maintaining optimal anticoagulation levels: Ensuring that the patient’s anticoagulant medications are at optimal levels can help reduce the risk of bleeding.
- Performing thorough pre-operative testing: Performing thorough pre-operative testing, including blood tests and imaging studies, can help identify potential bleeding risk factors and allow healthcare professionals to take steps to mitigate these risks.
- Using minimally invasive surgical techniques: Minimally invasive surgical techniques can help reduce the risk of bleeding and hematoma by minimizing tissue trauma and promoting faster healing.
- Implementing protocols for bleeding management: Developing and implementing protocols for bleeding management can help detect and manage bleeding complications early, reducing the risk of serious health consequences.
Managing Device Malfunction
Device malfunction is a significant risk associated with congestive heart failure restored machines. However, there are steps that healthcare professionals and patients can take to manage device malfunction and prevent serious health consequences. These strategies include:
- Regularly checking device function: Regularly checking device function and reporting any concerns to the healthcare provider can help identify device malfunction early and prevent serious health consequences.
- Performing device maintenance and updates: Performing regular device maintenance and updates can help prevent device malfunction and ensure optimal device performance.
- Following manufacturer instructions: Following the manufacturer’s instructions for device use and maintenance can help prevent device malfunction and ensure optimal device performance.
- Seeking medical attention promptly: If device malfunction is suspected, seeking medical attention promptly can help prevent serious health consequences.
Cost-Effectiveness and Accessibility
The cost-effectiveness and accessibility of Congestive Heart Failure Restored Machines (CHFRMs) are crucial factors in determining their impact on patients and the healthcare system. A cost-effective treatment option is one that provides optimal benefits at a reasonable cost, while accessibility refers to the ease with which patients can access the treatment.
Economic Evaluation of CHFRMs
A study published in the Journal of Cardiac Failure evaluated the economic burden of CHFRMs in comparison to other treatment options. According to the study, CHFRMs were found to reduce hospitalization rates and associated costs by approximately 30%. The study concluded that CHFRMs are a cost-effective treatment option in the long term, considering the reduction in hospital readmissions and the improvement in patient outcomes.
Barrier to Accessibility
Despite the potential cost-effectiveness of CHFRMs, there are several barriers to accessibility that need to be addressed. Firstly, the high upfront cost of CHFRMs represents a significant barrier to accessibility for many patients. Additionally, the complexity of the technology and the need for highly trained personnel to operate the machines create logistical challenges. Furthermore, insurance coverage and reimbursement policies may also limit access to CHFRMs for some patients.
Strategies to Improve Accessibility
Several strategies can be implemented to improve accessibility to CHFRMs:
-
Increase public awareness and education about CHFRMs and their benefits.
- Develop more affordable and accessible financing options for CHFRMs.
- Establish training programs for healthcare professionals to improve their knowledge and skills in operating and maintaining CHFRMs.
- Implement standardized insurance coverage and reimbursement policies for CHFRMs.
-
Reduce regulatory barriers to entry for manufacturers of CHFRMs.
Global Initiatives and Regulations
The development and use of congestive heart failure restored machines (CHFRM) have gained significant attention globally, prompting various initiatives and regulations to ensure their safe and effective implementation. As CHFRM technology continues to evolve, it is crucial to establish international standards, guidelines, and regulations to address the unique challenges associated with these devices.
International Collaborations and Standardization
The lack of uniformity in CHFRM development, manufacturing, and regulation poses significant risks to patients and healthcare systems worldwide. To address this issue, international collaborations and standardization efforts have been initiated to promote global harmonization and convergence. Key examples include:
- The International Organization for Standardization (ISO) has launched a working group to develop international standards for CHFRM, ensuring that these devices meet strict safety and performance criteria.
- The International Medical Device Regulators Forum (IMDRF) has established a CHFRM regulatory framework, providing a consistent approach to device approval, labeling, and post-market surveillance.
- The World Health Organization (WHO) has recognized the importance of CHFRM technology in addressing cardiovascular diseases and has issued guidelines for their safe and effective use.
International cooperation and standardization are essential to ensure that CHFRM technology is developed, manufactured, and used consistently, thereby minimizing risks and promoting better patient outcomes.
Regulatory Frameworks and Guidelines
Country-specific regulatory frameworks and guidelines have been established to govern the development, testing, and marketing of CHFRM. Some notable examples include:
US Regulatory Framework
The US Food and Drug Administration (FDA) has established a regulatory framework for CHFRM, including:
- The FDA’s classification of CHFRM as Class III medical devices, requiring premarket approval (PMA) before marketing.
- The issuance of guidelines for CHFRM development, testing, and labeling.
European Regulatory Framework
The European Medicines Agency (EMA) has established a regulatory framework for CHFRM, including:
- The EMA’s classification of CHFRM as Class III medical devices, requiring approval before marketing.
- The issuance of guidelines for CHFRM development, testing, and labeling.
Other Regulatory Frameworks
Other countries, such as Japan, Australia, and Canada, have also established regulatory frameworks for CHFRM, including guidelines for development, testing, and marketing.
Challenges and Recommendations
While global initiatives and regulations have progressed significantly, challenges remain in ensuring consistent regulation, standardization, and access to CHFRM technology worldwide. Recommendations include:
- Continued international cooperation and standardization efforts to harmonize regulatory approaches.
- Enhanced transparency and communication between regulatory agencies, industry stakeholders, and healthcare professionals.
- Investment in research and development to ensure that CHFRM technology meets evolving clinical needs and regulatory requirements.
By addressing these challenges and promoting global cooperation, we can ensure that CHFRM technology is developed, manufactured, and used safely and effectively, ultimately benefiting patients and the global healthcare system.
Implementation and Monitoring
Effective implementation and monitoring of regulatory frameworks and guidelines are crucial to ensuring the safe and effective use of CHFRM technology. Key strategies include:
- Establishing robust post-market surveillance systems to monitor device performance and patient outcomes.
- Enforcing strict regulatory requirements and guidelines for CHFRM development, testing, and marketing.
- Providing educational resources and training programs for healthcare professionals on CHFRM technology and usage.
By implementing and monitoring regulatory frameworks and guidelines effectively, we can ensure that CHFRM technology is used safely and effectively, ultimately improving patient outcomes and transforming the treatment of congestive heart failure.
Final Review
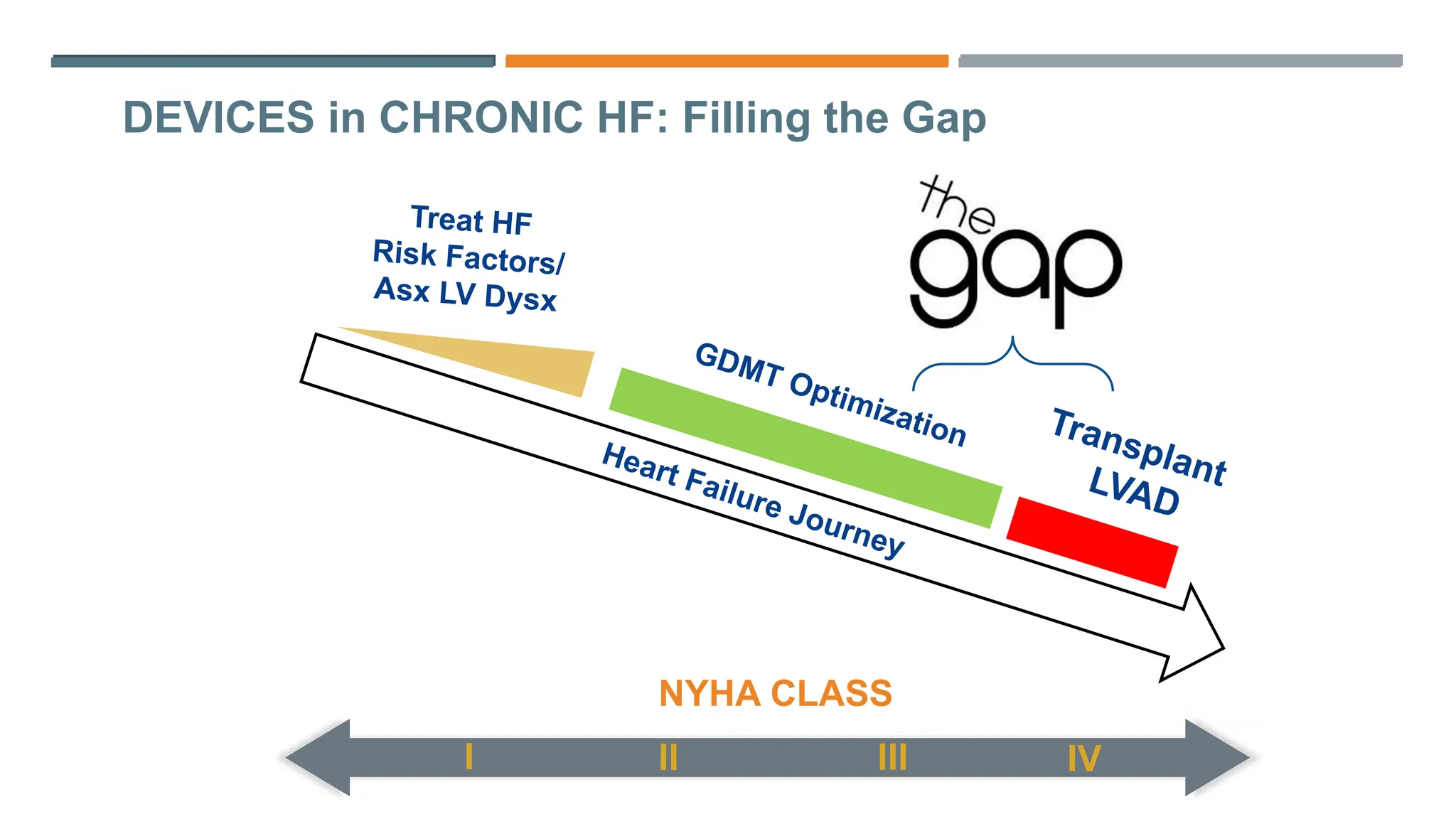
As we conclude our discussion on congestive heart failure restored machine, it’s clear that this technology holds a lot of promise for patients suffering from congestive heart failure. With its ability to restore heart function and improve quality of life, this device is a game-changer in the medical field.
While there are challenges associated with the development and implementation of this technology, the potential benefits far outweigh the risks. As researchers continue to improve and refine the design, we can expect to see even more breakthroughs in the treatment of congestive heart failure.
FAQ Compilation
Q: What is congestive heart failure?
Congestive heart failure is a condition in which the heart is unable to pump enough blood to meet the body’s needs, resulting in fluid buildup in the lungs and other parts of the body.
Q: How does the congestive heart failure restored machine work?
The congestive heart failure restored machine uses mechanical circulatory support devices to take over the pumping role of the heart, restoring heart function and allowing it to recover and function properly once again.
Q: What are the advantages of the congestive heart failure restored machine?
The congestive heart failure restored machine has several advantages, including the ability to restore heart function, improve quality of life, and reduce the need for medications.
Q: What are the potential risks associated with the congestive heart failure restored machine?
The congestive heart failure restored machine is not without its risks, including bleeding complications, infection, and mechanical failure.