Ecg Machine 12 Lead is a medical device used to diagnose heart-related problems by recording the electrical activity of the heart through 12 leads. This device has revolutionized the field of cardiology by providing accurate and reliable information about heart function. With its rich history and advanced technology, the Ecg Machine 12 Lead has become an essential tool for medical professionals worldwide.
The 12-lead Ecg Machine works by placing electrodes on the patient’s chest to record the electrical signals generated by the heart. These signals are then displayed on a monitor, allowing the doctor to interpret the results and make a diagnosis. The device is non-invasive and painless, making it a valuable diagnostic tool for patients of all ages.
Components of an ECG Machine 12 Lead
An ECG machine 12 lead is a sophisticated medical device used to record the electrical activities of the heart. It consists of various components that work together to capture and display the heart’s electrical signals.
Key components of a 12-lead ECG machine include:
Console or Control Panel
This is usually the main front-end interface of the ECG machine where you will find buttons and dials for selecting the type of ECG measurement, setting the display options, and adjusting various parameters of the recording.
ECG Electrodes
A set of 10 electrodes is placed on the patient’s body to detect the electrical signals generated by the heart. These electrodes are connected to the ECG machine via leads to transmit the signals to the machine. The three main types of ECG electrodes are:
- Ag-AgCl (Silver-Silver Chloride) electrodes: These are the most commonly used electrodes in clinical practice due to their excellent conductivity and stability.
- Silver-Disposable electrodes: These are pre-gelled electrodes that are easy to apply and dispose of after use.
- Carbon electrodes: These are used in some high-end ECG machines and offer very high sensitivity and conductivity.
Lead Cables and Connections
The ECG electrodes are connected to the console or control panel via lead cables. These cables carry the electrical signals from the electrodes to the machine, where they are processed and displayed.
ECG Machine Console
This is the main processing unit of the ECG machine where the digital signals are converted into a visual representation (ECG tracing) and displayed on a screen. It also stores the recorded ECG data for future analysis.
Printout or Storage Device
Many ECG machines come with a built-in printer that can print out the recorded ECG data. Others may have USB ports or SD card slots to store the data for later analysis or transfer to a computer.
Power Source and Cables
ECG machines require a power source (electricity or batteries) to operate. They usually come with a power cord or battery pack to connect to the power source.
How to Use an ECG Machine 12 Lead
Using an electrocardiogram (ECG) machine 12 lead requires a series of steps to prepare the patient for the test. This process involves carefully placing electrodes on the patient’s body to capture accurate heart readings. A well-executed procedure ensures optimal results and accurate diagnoses.
Step 1: Prepare the Patient
The patient must be seated comfortably and remain still during the test. Ask them to remove any clothing above the waist and provide a gown to wear. Ensure that the patient’s legs are uncrossed and feet are flat on the floor, with support available if necessary. Also, remove any metal items from the patient’s body, including necklaces, earrings, or glasses.
Step 2: Clean and Prepare the Skin
Cleanse the patient’s skin with an alcohol wipe or soap and water to remove dirt, oils, or lotions. This process should be done gently and carefully to avoid causing discomfort or irritation. Dry the skin completely to prevent any issues with electrode placement.
Applying the Electrodes
Apply the 12 lead ECG electrodes as follows:
–
Lead I:
Place the electrode on the left side of the lower rib cage, just below the left nipple.
–
Lead II:
Place one electrode on the right side of the lower rib cage, just below the right nipple, and another electrode on the left leg, about 4-6 inches below the top of the knee.
–
Lead III:
Place one electrode on the left side of the lower rib cage, just below the left nipple, and another electrode on the left leg, about 4-6 inches below the top of the knee, and still keeping the left arm to the side of the rib cage.
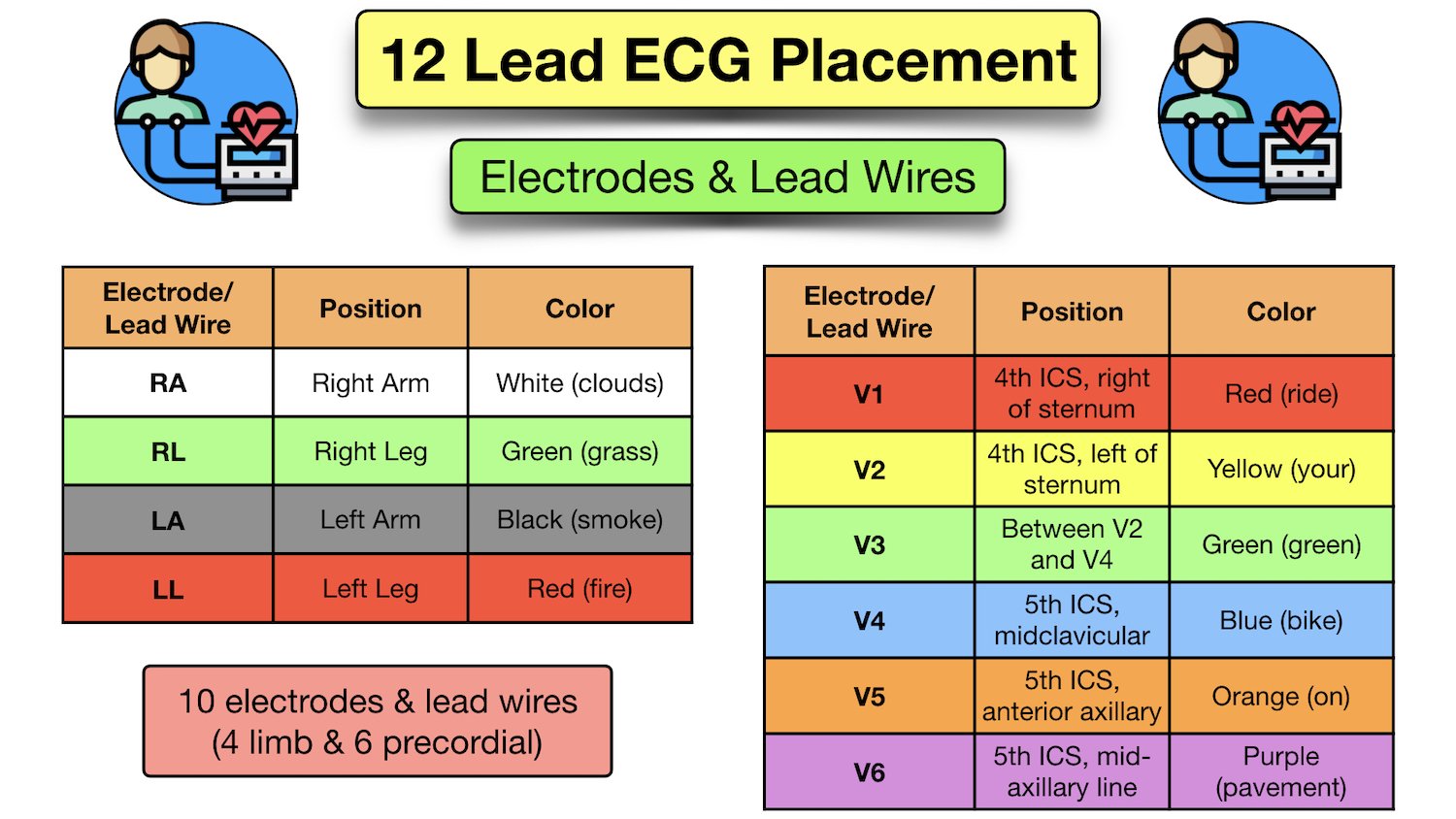
The ECG machine also comes with precordial (chest) leads, labeled V1-V6. These leads are placed on the chest in the following locations (V1-V6):
– V1: 4th intercostal space to the right of the sternum.
– V2: 4th intercostal space to the left of the sternum, near the sternum.
– V3: Midway between V2 and the left nipple.
– V4: 5th intercostal space to the left of the mid-clavicle, about 1-2 cm away from the left nipple.
– V5: Same as V4, just more to the left.
– V6: Same as V5, but more to the left.
For female patients, the chest leads may be placed in the following locations:
– V1: 4th intercostal space to the right of the sternum.
– V2: 4th intercostal space to the left of the sternum, near the sternum.
– V3: Midway between V2 and the left nipple.
– V4: 5th intercostal space to the left of the mid-clavicle, about 1-2 cm away from the left nipple.
– V5: One inch below V4, on an imaginary line that runs from the nipple to the lowest point of the breastbone.
– V6: One inch below V5, still following the breastbone.
Connecting the Leads
After applying the electrodes, gently pull the leads away from the body to prevent pinching the skin. Use the electrode wires to connect the electrodes to the ECG machine. Each lead is connected to a specific channel on the ECG machine. The connections should be labeled to prevent confusion.
Recording the ECG
Press the “record” button to capture the ECG signal. The machine will then display the 12-lead ECG on the screen or print it out on paper. Adjust the display settings as needed to ensure optimal viewing of the ECG signal.
Types of ECG Tracings 12 Lead
In a 12-lead ECG, various types of tracings can be obtained, each providing valuable information about the heart’s electrical activity. These tracings are crucial for diagnosing cardiac conditions, monitoring heart function, and making treatment decisions. A skilled healthcare professional interprets these tracings to identify abnormalities, detect changes, and monitor the heart’s response to treatment.
Normal ECG Tracing
A normal ECG tracing exhibits a characteristic pattern, with distinct waveforms and intervals. In a normal ECG, the waveform segments are:
These waveforms should be uniform, symmetrical, and within normal limits.
Abnormal ECG Tracings
Abnormal ECG tracings may indicate various cardiac conditions, such as arrhythmias, ischemia, or structural changes. Some common abnormal tracings include:
- Atrial fibrillation (AF): an irregular, rapid heart rate resulting from chaotic electrical activity in the atria.
- Bundle branch block: a blockage in one of the pathways that carries electrical impulses from the heart’s ventricles, resulting in an abnormal QRS complex.
- Ischemia: reduced blood flow to the heart muscle, leading to changes in the ECG waveform, such as ST-segment depression or T-wave inversion.
- Heart block: a disorder where the electrical impulses from the atria are delayed or blocked, resulting in a slower heart rate or a drop in blood pressure.
Pre-Excitation Syndromes
Pre-excitation syndromes, including Wolff-Parkinson-White (WPW) syndrome, result from an accessory electrical pathway between the atria and ventricles. This can lead to:
- PR interval shortening: the time interval between the P wave and QRS complex is shortened, usually less than 120 ms.
- Wide QRS complex: the QRS complex is widened due to the aberrant electrical pathway.
Post-Myocardial Infarction ECG
An ECG tracing after a myocardial infarction (MI) may exhibit various changes, including:
- ST-segment elevation: a rise in the ST segment above the baseline, indicating damage to the heart muscle.
- Q waves: a pathological Q wave, typically deep and wide, in leads V1-V3 or II, III, and aVF.
- T-wave inversion: a downward-directed T wave, often in leads V1-V3 or II, III, and aVF.
These changes help diagnose and monitor the healing process after an MI.
Other Abnormal Tracings
Other abnormal ECG tracings include:
- Bradycardia: a slow heart rate (less than 60 beats per minute).
- Tachycardia: a rapid heart rate (more than 100 beats per minute).
- QT interval prolongation: a prolonged QT interval, often associated with life-threatening arrhythmias.
- U waves: small, positive deflections after the T wave, often seen in hypokalemia or digitalis toxicity.
It is essential to recognize these abnormal tracings to diagnose underlying cardiac conditions and guide appropriate treatment.
Interpretation of ECG Tracings 12 Lead: Ecg Machine 12 Lead
The interpretation of 12-lead ECG tracings is a crucial step in diagnosing and managing cardiovascular diseases. It involves analyzing the waveform patterns, durations, and amplitudes to identify abnormalities in the heart’s electrical activity.
Principles of ECG Interpretation
When interpreting a 12-lead ECG, it’s essential to understand the principles of ECG interpretation. These principles include:
- The P wave represents atrial depolarization and should be upright in most leads.
- The QRS complex represents ventricular depolarization and should be narrow and upright in most leads.
- The T wave represents ventricular repolarization and should be upright in most leads.
- The U wave represents the final repolarization of the ventricles and is usually small and peaked.
Understanding these principles helps clinicians identify abnormalities in the heart’s electrical activity, such as arrhythmias, conduction disturbances, and ischemia.
Analysis of a 12-Lead ECG Tracing
Analyzing a 12-lead ECG tracing involves examining the waveform patterns, durations, and amplitudes in each lead. This includes:
- Measuring the PR interval, which is the time between the start of the P wave and the start of the QRS complex.
- Measuring the QRS duration, which is the time between the start and end of the QRS complex.
- Measuring the QT interval, which is the time between the start of the Q wave and the end of the T wave.
- Examining the waveform patterns in each lead for signs of ischemia, infarction, or other abnormalities.
By analyzing these parameters, clinicians can identify potential cardiovascular problems, such as arrhythmias, conduction disturbances, and ischemia.
Interpretation of ECG Abnormalities
Abnormalities in the 12-lead ECG tracing can indicate various cardiovascular conditions. These include:
- Arrhythmias, such as atrial fibrillation or ventricular tachycardia.
- Conduction disturbances, such as first- or second-degree AV block.
- Ischemia or infarction, indicated by ST-segment elevation or depression.
- Cardiomyopathy, which can manifest as changes in the QRS complex or T wave.
Clinicians use these interpretations to guide further testing, treatment, and management of patients with cardiovascular disease.
Importance of Quality and Consistency
The quality and consistency of ECG tracings are crucial for accurate interpretation. Factors that can affect ECG quality include:
- Lead placement, which can affect the amplitude and orientation of the waveform.
- Lead calibration, which can affect the sensitivity and accuracy of the tracing.
- Electrode quality, which can affect the signal-to-noise ratio and waveform clarity.
Clinicians must be aware of these factors and take steps to ensure high-quality ECG tracings to ensure accurate interpretation and effective patient care.
Clinical Applications of ECG Machine 12 Lead
The 12-lead ECG machine is a medical diagnostic tool used to evaluate the electrical activity of the heart. It is an essential tool in the clinical setting, providing valuable information for healthcare professionals to diagnose and manage various cardiac conditions. The 12-lead ECG is widely used in hospitals, clinics, and emergency medical services around the world.
Acute Myocardial Infarction (AMI) Detection
The 12-lead ECG is a critical tool for detecting acute myocardial infarction (AMI), commonly known as a heart attack. During an AMI, the ECG machine can detect the characteristic changes in the heart’s electrical activity, such as ST-segment elevation or depression, and Q-wave formation. These changes can indicate coronary artery occlusion or cardiac ischemia, prompting immediate medical attention.
- ST-segment elevation myocardial infarction (STEMI): Characterized by ST-segment elevation in two or more adjacent leads.
- Non-ST-segment elevation myocardial infarction (NSTEMI): Characterized by subtle ST-segment changes or T-wave inversion.
Arrhythmia Diagnosis and Management
The 12-lead ECG is also used to diagnose and manage various arrhythmias, including atrial fibrillation, atrial flutter, and ventricular tachycardia. Healthcare professionals can use the ECG machine to identify the underlying causes of arrhythmias, such as electrolyte imbalances or structural heart disease.
- Atrial fibrillation: Characterized by rapid, irregular atrial contractions and loss of P-wave activity.
- Atrial flutter: Characterized by rapid, regular atrial contractions and saw-tooth P-wave pattern.
Preoperative and Postoperative Cardiac Risk Assessment
The 12-lead ECG is a valuable tool for evaluating patients preoperatively and postoperatively, particularly for those undergoing non-cardiac surgery. The ECG can identify pre-existing cardiac conditions, such as coronary artery disease or heart failure, and assess the patient’s cardiac risk profile.
Regular ECG Monitoring
Regular ECG monitoring is essential for patients with known cardiac conditions, such as coronary artery disease or heart failure. This monitoring allows healthcare professionals to detect subtle changes in the heart’s electrical activity, enabling timely interventions and adjustments to medication or treatment plans.
The American Heart Association recommends that patients with known cardiac conditions undergo regular ECG monitoring, ideally every 3-6 months, depending on individual risk factors.
Maintenance and Troubleshooting of ECG Machine 12 Lead
Regular maintenance of a 12-lead ECG machine is crucial to ensure accurate and reliable heart rate readings, allowing healthcare professionals to make informed decisions about patient care. Neglecting maintenance may lead to inaccurate readings, equipment failure, or even injury to patients.
Importance of Regular Maintenance
Maintenance of an ECG machine involves regular cleaning, calibration, and replacement of worn-out parts. Failure to maintain the device may result in
- Incorrect or inaccurate readings
- Prolonged downtime or equipment failure
- Costly repairs or replacement
- Potential harm to patients due to inaccurate diagnoses
A well-maintained ECG machine is essential for delivering high-quality patient care and ensuring the confidence of healthcare professionals in their diagnostic readings.
Common Issues and Troubleshooting
Despite regular maintenance, ECG machines may still encounter issues. Some common problems include:
Electrode-Related Issues
Electrode-related problems can be caused by worn-out or damaged electrodes, loose connections, or faulty electrode cables.
ECG Signal Artifact
ECG signal artifacts can be caused by various factors, including interference from nearby electrical devices, faulty leads, or issues with the ECG machine’s electronics.
Maintenance and Calibration
Regular calibration and maintenance are crucial to ensuring the accuracy and reliability of ECG readings. This includes:
- Cleaning the ECG machine and electrodes
- Inspecting and replacing worn-out parts
- Calibrating the ECG machine to ensure accurate readings
The regular maintenance of a 12-lead ECG machine ensures the accuracy of patient readings, prevents equipment failure, and supports healthcare professionals in delivering high-quality care.
Predictable Maintenance Schedules
Maintenance schedules should be developed in consultation with the healthcare provider or service provider. A typical maintenance schedule for an ECG machine may be as follows:
- Every 2-3 months: Perform a cleaning and inspection of the ECG machine and its components.
- Every 6-12 months: Perform a calibration of the ECG machine.
- Every 2-5 years: Replace worn-out or damaged parts of the ECG machine.
The maintenance schedule may vary depending on usage patterns and other factors, ensuring reliable and efficient patient care.
Mechanisms of Maintenance Schedules
Regular inspections of the ECG machine can be accomplished by observing the machine’s performance and monitoring it’s functionality in a normal, day-to-day environment. Monitoring the ECG machine is crucial to recognizing when maintenance is required.
Comparison of ECG Machine 12 Lead with Other Monitoring Devices

The comparison of an ECG machine 12 lead with other monitoring devices is crucial to understand their advantages and disadvantages. This allows clinicians to select the most suitable device for a particular patient or clinical scenario, ensuring accurate detection and monitoring of cardiac rhythms. Among the various monitoring devices available, ECG machines 12 lead are widely used in clinical settings due to their high accuracy and comprehensive assessment of cardiac function.
ECG Machine 12 Lead vs. Holter Monitor
A Holter monitor is a portable device that records the heart’s activity for 24-48 hours, allowing for the detection of irregular heart rhythms and arrhythmias that may not be apparent during a standard ECG test. While both devices can detect cardiac arrhythmias, the ECG machine 12 lead offers more comprehensive and immediate feedback during the procedure. Unlike Holter monitors, ECG machines 12 lead are typically used in clinical settings and require a trained clinician to interpret the results.
- ECG Machine 12 Lead Advantages:
- Immediate feedback and comprehensive assessment of cardiac function
- Higher accuracy in detecting cardiac arrhythmias
- Multichannel recording and simultaneous display of leads
- Holter Monitor Advantages:
- Multiples days of recording and data analysis
- Long-term monitoring of cardiac rhythms
- Ability to detect arrhythmias during daily activities
ECG Machine 12 Lead vs. Cardiac Event Monitor
A cardiac event monitor is a portable device that records the heart’s activity during symptoms or episodes of suspected arrhythmia. This device helps clinicians to identify the underlying cause of symptoms and diagnose cardiac arrhythmias. Similar to Holter monitors, cardiac event monitors are used for long-term monitoring of cardiac rhythms, whereas ECG machines 12 lead are used in clinical settings for immediate assessment and comprehensive evaluation of cardiac function.
- ECG Machine 12 Lead Advantages:
- Multichannel recording and simultaneous display of leads
- Higher accuracy in detecting cardiac arrhythmias
- Comprehensive assessment of cardiac function
- Cardiac Event Monitor Advantages:
- Long-term monitoring of cardiac rhythms during symptoms or episodes
- Multiples days of recording and data analysis
- Ability to detect arrhythmias during daily activities
ECG Machine 12 Lead vs. Pulse Oximeter
A pulse oximeter is a device that measures blood oxygen saturation and heart rate. While both devices can monitor cardiovascular function, the ECG machine 12 lead offers a more comprehensive assessment of cardiac function and detects cardiac arrhythmias. The pulse oximeter is typically used during anesthesia, emergency medicine, and intensive care, whereas the ECG machine 12 lead is used in clinical settings for immediate assessment and comprehensive evaluation of cardiac function.
- ECG Machine 12 Lead Advantages:
- Multichannel recording and simultaneous display of leads
- Higher accuracy in detecting cardiac arrhythmias
- Comprehensive assessment of cardiac function
- Pulse Oximeter Advantages:
- Non-invasive and quick measurement of blood oxygen saturation
- Multiples uses, such as anesthesia, emergency medicine, and intensive care
- Cost-effective and portable
Advantages of Using ECG Machine 12 Lead
The 12-lead ECG machine is a vital diagnostic tool in the field of cardiology, providing a comprehensive view of the heart’s electrical activity. With its unique ability to capture information from multiple angles, the 12-lead ECG offers numerous advantages over other types of ECG machines.
Higher Diagnostic Accuracy
The 12-lead ECG is considered the gold standard due to its ability to detect subtle changes in the heart’s electrical activity. This is achieved through the placement of 12 electrocardiogram leads on the body, allowing the machine to capture information from different angles. As a result, the 12-lead ECG can detect conditions such as myocardial infarction, cardiac arrhythmias, and other cardiomyopathies with greater accuracy.
Wider Range of Applications
The 12-lead ECG is not limited to diagnosing cardiac conditions. It can also be used to monitor patients with respiratory problems, such as pneumonia, and those with neurological disorders, such as stroke. In addition, the 12-lead ECG can be used to monitor patients with electrolyte imbalances and those on life-support systems.
Improved Patient Outcomes, Ecg machine 12 lead
The use of 12-lead ECG machines can lead to improved patient outcomes, particularly in emergency situations. For example, a 12-lead ECG can quickly identify a patient suffering from a myocardial infarction, allowing for prompt treatment and potentially saving the patient’s life.
Reduced Risk of Misdiagnosis
The 12-lead ECG reduces the risk of misdiagnosis by providing a comprehensive view of the heart’s electrical activity. This is particularly important for patients with complex or atypical presentations, where a 12-lead ECG can help differentiate between potential causes of the patient’s symptoms.
Increased Efficiency
The 12-lead ECG can be performed quickly and efficiently, making it an ideal tool for emergency situations. In contrast to other types of ECG machines, the 12-lead ECG can be performed in a matter of minutes, allowing healthcare professionals to quickly diagnose and treat patients.
Cost-Effectiveness
The 12-lead ECG is a cost-effective diagnostic tool, particularly when compared to other imaging modalities such as echocardiography and MRI. Additionally, the 12-lead ECG can be used to monitor patients over time, reducing the need for repeated testing and further reducing costs.
Portability and Ease of Use
12-lead ECG machines are designed to be portable and easy to use, making them ideal for use in various clinical settings. Whether in an emergency department, clinic, or hospital room, the 12-lead ECG can be quickly set up and used to diagnose a wide range of cardiac and non-cardiac conditions.
Long-Term Monitoring
The 12-lead ECG can be used for long-term monitoring of patients, allowing healthcare professionals to track changes in the heart’s electrical activity over time. This is particularly useful for patients with chronic conditions, such as heart failure, and those undergoing treatment for cardiac conditions.
Continuous Quality Improvement
The 12-lead ECG enables healthcare professionals to continuously assess and improve the quality of patient care. By monitoring the heart’s electrical activity over time, healthcare professionals can identify areas for improvement and refine treatment strategies to optimize patient outcomes.
Standardization of Care
The 12-lead ECG promotes standardization of care by providing a common language and framework for diagnosing and treating patients. By using a standardized 12-lead ECG, healthcare professionals can ensure that patients receive consistent and high-quality care, regardless of the clinical setting.
Limitations of ECG Machine 12 Lead
The 12-lead ECG machine is a widely used and effective tool for diagnosing heart conditions. However, like any medical device, it has its limitations. Understanding these limitations is crucial for accurate diagnosis and effective treatment.
Skin Conductance Issues
Skin conductance, or the ability of the skin to conduct an electrical signal, can be a limitation of the 12-lead ECG machine. Thick or dry skin can impede the conduction of the electrical signal, leading to inaccurate readings. This is particularly common in people with conditions such as hyperglycemia, hypothyroidism, or certain skin conditions. In such cases, the ECG machine may struggle to provide a clear and accurate picture of the heart’s electrical activity.
- Inadequate skin preparation can lead to poor signal quality, making it challenging to obtain accurate readings.
- Some individuals may have skin conditions that affect their skin’s conductance properties, such as hyperkeratosis or eczema.
- The use of certain medications, such as some antihistamines or antidepressants, can affect the skin’s moisture levels and contribute to conductance issues.
Patient Movement and Artifact
Patient movement and artifact, or unwanted electrical signals, can also limit the effectiveness of the 12-lead ECG machine. Movement can distort the electrical signal, making it difficult to interpret. This can be particularly problematic in patients who are anxious, restless, or have a pacemaker. In such cases, the ECG machine may struggle to provide a clear and accurate picture of the heart’s electrical activity.
- Patient movement, whether due to anxiety, restlessness, or other factors, can lead to artifact and distort the electrical signal.
- Patients with pacemakers or other implantable devices may experience electrical interference, which can affect ECG readings.
- Certain medical procedures, such as defibrillation or cardioversion, can also interfere with ECG readings.
Electrode Placement Issues
Electrode placement is a critical aspect of obtaining accurate ECG readings. If electrodes are not placed correctly, it can lead to inaccuracies. This can be due to various factors, such as operator error, inadequate training, or equipment failure. In such cases, the ECG machine may struggle to provide a clear and accurate picture of the heart’s electrical activity.
- Inadequate electrode placement can lead to inaccurate readings, as the electrical signal may not be properly captured.
- Operators who are not properly trained may not know how to place electrodes correctly, leading to suboptimal results.
- Equipment failure, such as faulty electrodes or damaged leads, can also contribute to electrode placement issues.
Electromagnetic Interference (EMI)
Electromagnetic interference (EMI) can also limit the effectiveness of the 12-lead ECG machine. EMI involves unwanted electrical signals that can distort the electrical signal being captured by the ECG machine. This can be particularly problematic in patients who undergo medical procedures that involve EMI, such as MRI scans or electrical cardioversion. In such cases, the ECG machine may struggle to provide a clear and accurate picture of the heart’s electrical activity.
- EMI from other medical equipment, such as defibrillators or MRI machines, can distort the electrical signal and affect ECG readings.
- Certain environmental factors, such as fluorescent lighting or high-voltage power lines, can also contribute to EMI.
- Patients with implantable devices, such as pacemakers or neurostimulators, may be particularly vulnerable to EMI.
Age-Related Limitations
Age-related limitations, such as reduced skin conductance and increased electrode impedance, can also affect the accuracy of the ECG machine. Older adults may experience reduced skin conductance due to age-related changes, such as reduced skin thickness and elasticity. This can make it more challenging to obtain accurate ECG readings.
- Reduced skin conductance can make it more difficult to obtain accurate ECG readings in older adults.
- Increased electrode impedance can also contribute to inaccuracies in ECG readings.
- Age-related changes, such as reduced muscle mass and increased body fat, can affect ECG readings.
Closure
In conclusion, the Ecg Machine 12 Lead is a powerful tool that has improved patient care and outcomes. Its accuracy and reliability have made it the gold standard for diagnosing heart-related problems. As technology continues to advance, it’s essential to understand the benefits and limitations of this device to ensure its proper use and maintenance.
By continuing to educate ourselves about the Ecg Machine 12 Lead, we can ensure that patients receive the best possible care and treatment for their heart-related conditions.
FAQ Insights
What is the purpose of an Ecg Machine 12 Lead?
The purpose of an Ecg Machine 12 Lead is to record the electrical activity of the heart through 12 leads, providing accurate and reliable information about heart function.
How does the Ecg Machine 12 Lead work?
The Ecg Machine 12 Lead works by placing electrodes on the patient’s chest to record the electrical signals generated by the heart, which are then displayed on a monitor for interpretation.
What are the benefits of using an Ecg Machine 12 Lead?
The benefits of using an Ecg Machine 12 Lead include its accuracy, reliability, and non-invasive nature, making it a valuable diagnostic tool for patients of all ages.
Can an Ecg Machine 12 Lead be used on patients with a pacemaker?
Yes, an Ecg Machine 12 Lead can be used on patients with a pacemaker, but the device settings may need to be adjusted to ensure accurate results.
How often should an Ecg Machine 12 Lead be calibrated?
An Ecg Machine 12 Lead should be calibrated regularly, typically every 6 months, to ensure accurate and reliable results.