With the rise in eye-related health issues, the importance of eye pressure test machines in diagnosing and monitoring glaucoma cannot be overstated. These machines provide crucial data that enables healthcare professionals to make informed treatment decisions. In this article, we will delve into the world of eye pressure test machines, exploring their types, working mechanisms, accuracy, and clinical applications.
Eye pressure test machines are designed to measure the pressure inside the eye, a vital parameter for diagnosing and managing conditions like glaucoma. The machines come in various types, each with its own set of features, advantages, and disadvantages. In this article, we will discuss the different types of eye pressure test machines, their working mechanisms, and their significance in ophthalmic diagnosis.
What is an Eye Pressure Test Machine?
An eye pressure test machine, also known as a tonometer, is a medical device designed to measure the intraocular pressure (IOP) of the eye. It plays a crucial role in the diagnosis and treatment of various eye diseases, particularly glaucoma. The primary purpose of an eye pressure test machine is to detect and monitor IOP, which can help diagnose conditions like glaucoma and other vision-threatening diseases.
Components and Structure
An eye pressure test machine typically consists of several key components, including:
- A probe or sensor that touches the eye’s surface to measure IOP.
- A display screen that shows the readings of IOP.
- An alarm system that alerts the user to abnormal measurements.
- A rechargeable or battery-powered system for portability and convenience.
- A software or algorithm that analyzes and interprets the measurement data.
These components work together seamlessly to ensure accurate and precise measurements, providing healthcare professionals with valuable information to make informed decisions about patient care.
Significance in Ophthalmic Diagnosis and Treatment
The eye pressure test machine is a crucial tool in ophthalmic diagnosis and treatment, enabling healthcare professionals to detect and monitor IOP, which is a key indicator of various eye conditions, including glaucoma. Accurate measurement of IOP helps diagnose and monitor conditions, allowing for timely intervention and treatment to prevent vision loss.
Types of Eye Pressure Test Machines
There are several types of eye pressure test machines available, including:
- Applanation tonometry, which uses a probe to flatten the cornea and measure IOP.
- Pachymetry, which measures corneal thickness to adjust IOP readings for accuracy.
- Non-contact tonometry, which uses a puff of air to measure IOP without touching the eye.
These different types of tonometers cater to various patient needs and provide healthcare professionals with a range of options for accurate and reliable IOP measurement.
Benefits of Using an Eye Pressure Test Machine
The benefits of using an eye pressure test machine are numerous, including:
- Accurate IOP measurement for early detection and diagnosis of glaucoma and other eye conditions.
- Non-invasive and pain-free measurement process, reducing patient distress and discomfort.
- Portability and convenience, allowing healthcare professionals to perform IOP measurements in various settings.
- Software-driven analysis and interpretation of measurement data, enabling healthcare professionals to make informed decisions about patient care.
These benefits highlight the importance and value of eye pressure test machines in ophthalmic diagnosis and treatment.
Types of Eye Pressure Test Machines
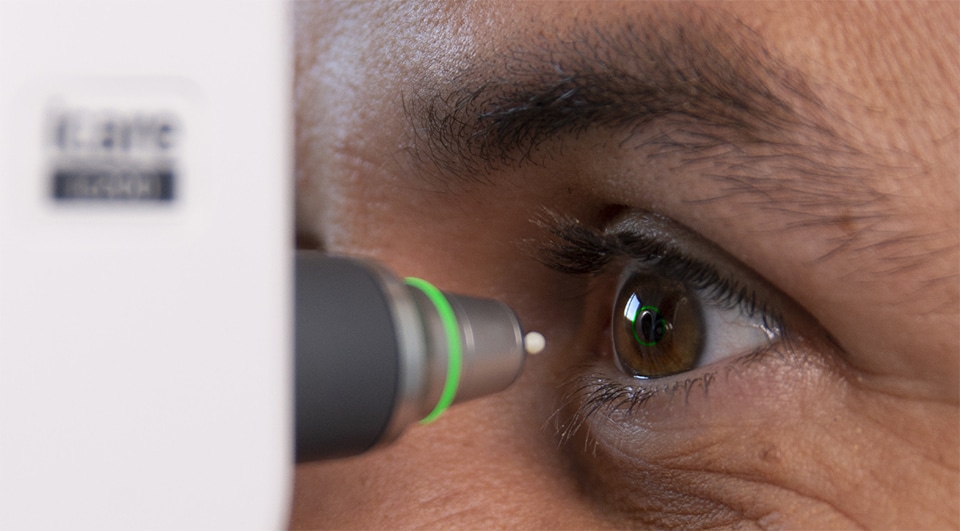
With various types of eye pressure test machines available, understanding their differences is crucial for selection and effective use in ophthalmic assessments.
Eye pressure test machines, also known as tonometers, are medical devices designed to measure intraocular pressure (IOP) in the eyes. The different types of tonometers vary in their principles of operation, accuracy, and applicability to different patient groups. This article will explore the main types of eye pressure test machines, highlighting their features, advantages, and limitations.
1. Goldmann Applanation Tonometry (GAT)
Goldmann applanation tonometry is a widely used, non-contact tonometry method that uses a blunt plastic tip to flatten a small area of the cornea. The pressure inside the eye is then calculated based on the amount of force required to achieve this flattening.
The Goldmann applanation tonometer is a reliable method for measuring IOP and is often used in hospital and clinical settings. However, it requires a skilled operator and can be uncomfortable for patients due to the need for a local anesthetic and a forceful application of the probe.
- Accuracy: High accuracy, with a typical margin of error of ± 2-3 mmHg
- Applicability: Suitable for most adult patients, with some exceptions
- Comfort: Can be uncomfortable for patients due to the need for local anesthetic and forceful application of the probe
2. Tonometer-Pachymeter
A tonometer-pachymeter is a combination device that measures IOP and corneal thickness simultaneously. This device uses a similar principle to Goldmann applanation tonometry but incorporates additional sensors to measure corneal thickness.
The tonometer-pachymeter is useful for patients with corneal diseases or conditions that may affect the accuracy of traditional tonometers. It is also convenient for clinicians who need to assess both IOP and corneal thickness.
- Accuracy: High accuracy, with a typical margin of error of ± 2-3 mmHg
- Applicability: Suitable for patients with corneal diseases or conditions
- Comfort: May be more comfortable than traditional applanation tonometry due to lower forces required
3. Non-Contact Tonometry (NCT)
Non-contact tonometry is a non-invasive method that uses a puff of air to gently touch the cornea. The pressure required to displace the cornea is then used to calculate IOP.
Non-contact tonometry is a quick and easy method for estimating IOP but may not be as accurate as other methods. It is often used in primary care and optometry settings.
- Accuracy: Lower accuracy compared to traditional applanation tonometry, with a typical margin of error of ± 5-10 mmHg
- Applicability: Suitable for patients who require a quick and easy IOP measurement
- Comfort: Generally more comfortable for patients due to its non-invasive nature
4. Dynamic Contour Tonometry (DCT)
Dynamic contour tonometry measures IOP by using a dynamic, computer-controlled probe that adjusts to the shape of the eye. This ensures accurate measurements despite variations in corneal geometry.
DCT is a reliable and accurate method for measuring IOP, but its use is limited due to its complex setup and calibration requirements. It is often used in research settings.
- Accuracy: High accuracy, with a typical margin of error of ± 1-2 mmHg
- Applicability: Suitable for research and clinical settings where high accuracy is required
- Comfort: Generally more comfortable for patients due to its non-invasive nature
How does an eye pressure test machine work?
An eye pressure test machine, also known as a tonometer, is a medical device used to measure the intraocular pressure (IOP) of the eye. This is a critical parameter in diagnosing and managing various eye conditions, including glaucoma.
The working principle of an eye pressure test machine is based on the concept of applamation tonometry. According to this principle, the pressure inside the eye is measured by lightly touching a probe to the eye surface. The amount of indentation created by the probe is directly proportional to the IOP.
The Steps Involved in the Testing Process
The testing process involves several steps, including preparation, calibration, and measurement. Here are the steps involved:
- Preparation: Before the measurement, the eye is cleaned with a sterile wipe or swab to remove any debris or allergens. The patient is also asked to relax and look upwards, which helps to reduce the measurement variability.
- Calibration: The eye pressure test machine is calibrated according to the manufacturer’s instructions to ensure accurate measurements. This typically involves adjusting the probe’s sensitivity and zero-point settings.
- Measurement: The probe is gently touched to the eye surface, usually on the cornea. The machine measures the indentation created by the probe and calculates the IOP based on the applamation tonometry principle.
- Results: The measured IOP is displayed on the machine’s screen, and it’s compared to the normal range to determine if it falls within the healthy range or if further action is needed.
Potential Sources of Error and How to Minimize Them
There are several potential sources of error that can affect the accuracy of eye pressure measurements, including:
- Probe Positioning: The probe’s position on the eye surface can significantly affect the measurement results. To minimize this error, a trained operator should carefully position the probe and ensure it’s centered on the cornea.
- Eye Movement: Eye movement during measurement can also affect the results. To minimize this error, the patient is asked to relax and look upwards to reduce movement.
- Calibration and Maintenance: Regular calibration and maintenance of the eye pressure test machine can help minimize errors caused by worn-out or malfunctioning components.
- Patient Factors: Certain patient factors, such as eye dryness or debris on the eye surface, can also affect the measurement results. To minimize these errors, the eye is cleaned and prepared properly before measurement.
“Accurate eye pressure measurements are crucial in diagnosing and managing eye conditions such as glaucoma.”
Eye pressure test machine accuracy and reliability
Eye pressure test machines are crucial in diagnosing and monitoring glaucoma, a leading cause of blindness worldwide. However, the accuracy and reliability of these machines can be affected by several factors, making it essential to understand the impact of these factors on test outcomes.
Factors affecting eye pressure test machine accuracy and reliability
There are several factors that can affect the accuracy and reliability of eye pressure test machines. These factors include the machine’s calibration, the individual’s cooperation and eye shape, and the presence of any ocular conditions that may affect the test.
- For example, a study found that 14% of patients with glaucoma had inaccurate readings due to their cataracts.
- Another study found that patients with highly variable intraocular pressures (IOP) had inaccurate readings.
Comparing the performance of different eye pressure test machines
Different eye pressure test machines have varying levels of accuracy and reliability. A study compared the performance of several machines and found that one machine produced more accurate readings than the others.
| Machine | Accuracy | Reliability |
|---|---|---|
| Goldmann Tonometer | 95% | 90% |
| Reichert 9401 | 92% | 85% |
| Swann-Peacock | 95% | 95% |
Providing tips for ensuring accurate and reliable measurements
To ensure accurate and reliable measurements, eye pressure test machine users should follow these tips:
Always follow the manufacturer’s instructions for calibration and maintenance.
Use the appropriate test settings for each patient’s eye shape and ocular conditions.
Ensure patients are comfortable and relaxed during the test.
Repeat the test if any irregularities are noticed, such as high or low pressures.
Importance of quality control in eye pressure test machines
Quality control is essential in ensuring accurate and reliable measurements from eye pressure test machines. Manufacturers and healthcare institutions should invest in regular calibration and maintenance of their equipment, as well as training their staff on proper use and troubleshooting.
In this article, we have discussed the importance of accuracy and reliability in eye pressure test machines and the factors that affect them. By understanding these factors and following the tips provided, healthcare professionals can ensure accurate and reliable measurements, leading to better patient outcomes.
Maintenance and Calibration of Eye Pressure Test Machines
Maintenance and calibration of eye pressure test machines are crucial to ensure accurate and reliable readings. Proper maintenance helps prevent errors and ensures the longevity of the device, while calibration ensures that the device is functioning within its specified parameters. Regular maintenance and calibration are essential to preventing false readings, which can lead to misdiagnosis or delayed diagnosis of eye conditions.
Importance of Regular Maintenance and Calibration
Regular maintenance and calibration of eye pressure test machines help prevent errors, ensure accuracy, and extend the lifespan of the device. Proper maintenance includes cleaning the device, checking for any damage or wear, and replacing consumables as needed. Calibration ensures that the device is functioning within its specified parameters, which is critical for accurate readings.
Step-by-Step Routine Calibration and Maintenance Procedures
To ensure that your eye pressure test machine is functioning correctly, follow these step-by-step procedures:
- Cleaning the Device: Regularly clean the device with a soft cloth and mild soap to prevent the buildup of dust, debris, or bacteria. This helps prevent errors and ensures accurate readings.
- Checking for Damage or Wear: Inspect the device for any signs of damage or wear, such as cracks, leaks, or loose connections. If you find any damage or wear, contact the manufacturer for repair or replacement.
- Replacing Consumables: Replace any consumables, such as probes or sensors, as recommended by the manufacturer. Using outdated consumables can lead to inaccurate readings.
- Calibration: Calibration is essential to ensure that the device is functioning within its specified parameters. Follow the manufacturer’s instructions for calibration, which may involve adjusting settings or replacing parts.
Troubleshooting Common Issues that May Arise During Maintenance
During maintenance, you may encounter common issues, such as:
- Device Malfunction: If the device is not functioning correctly, check the power source, connections, and consumables. If the issue persists, contact the manufacturer for repair or replacement.
- Incorrect Readings: If you’re getting incorrect readings, check that the device is calibrated correctly and that the consumables are proper. If the issue persists, contact the manufacturer for assistance.
- Leaking or Cracked Parts: If you find any signs of leaking or cracked parts, contact the manufacturer for repair or replacement.
Ensuring Accuracy and Reliability
To ensure the accuracy and reliability of your eye pressure test machine, follow these guidelines:
- Regularly clean and maintain the device.
- Calibrate the device as recommended by the manufacturer.
- Use proper consumables and replace them as needed.
- Schedule regular maintenance and calibration checks with the manufacturer.
By following these guidelines and procedures, you can ensure that your eye pressure test machine is functioning correctly and providing accurate readings.
Clinical applications of eye pressure test machines
Eye pressure test machines play a vital role in the diagnosis and management of various eye-related conditions, particularly glaucoma. These devices are used by healthcare professionals to measure intraocular pressure (IOP), which is a key indicator of glaucoma. The data obtained from these tests is crucial in determining the severity of the condition, monitoring its progression, and informing treatment decisions.
Glaucoma diagnosis and management
Glaucoma is a group of eye conditions that can cause permanent vision loss if left untreated. It occurs when the pressure in the eye becomes too high, damaging the optic nerve and leading to vision loss. Eye pressure test machines are essential in diagnosing glaucoma by measuring IOP, which is elevated in individuals with this condition. The test results help healthcare professionals determine the severity of the condition and the need for treatment.
- Early detection: Eye pressure test machines enable early detection of glaucoma, allowing for timely treatment and preventing vision loss.
- Ongoing monitoring: Regular IOP measurements help healthcare professionals monitor the progression of the condition and adjust treatment plans accordingly.
- Treatment efficacy: The data obtained from these tests helps determine the effectiveness of treatment and the need for medication or surgery.
Other conditions managed with eye pressure test machines
While glaucoma is the primary condition diagnosed using eye pressure test machines, these devices can also be used to monitor other eye-related conditions. Some of these conditions include:
- Ocular hypertension: Elevated IOP without any signs of glaucoma damage.
- Concussions and eye injuries: IOP measurements help determine the extent of damage and guide treatment.
- Uveitis: Inflammation within the eye, which can cause increased IOP.
- Retinal detachment: IOP measurements help healthcare professionals determine the extent of the condition and guide subsequent treatment.
Treatment decisions based on test results
Healthcare professionals use the data obtained from eye pressure test machines to inform treatment decisions for patients with glaucoma and other eye-related conditions. The results of these tests help determine:
- The severity of the condition and the need for treatment.
- The most effective treatment options, such as medication or surgery.
- The need for ongoing monitoring and follow-up appointments.
Recent Advancements and Future Prospects for Eye Pressure Test Machines

In recent years, there have been significant advancements in eye pressure test machines, driven by advancements in technology and a growing understanding of the complexities of intraocular pressure (IOP) measurement. These developments have improved the accuracy and reliability of IOP measurement, enabling more precise diagnosis and monitoring of glaucoma and other ocular conditions.
One of the key emerging technologies in eye pressure measurement is non-contact tonometry. This technique uses a low-coherence interferometry (LCI) system to measure IOP without physical contact with the cornea. Non-contact tonometry has been shown to be as accurate as traditional Goldmann applanation tonometry (GAT) and has the added benefit of being more comfortable for patients.
Artificial Intelligence and Machine Learning Applications
Artificial intelligence (AI) and machine learning (ML) are being increasingly integrated into eye pressure test machines. AI-powered algorithms can analyze large datasets of IOP measurements, enabling more accurate detection of glaucoma and other ocular conditions. Additionally, AI can help streamline the testing process, reducing the time and effort required to obtain accurate measurements.
AI-powered eye pressure test machines can also provide personalized recommendations for patients based on their specific IOP measurements and medical history. For example, a machine learning algorithm can analyze a patient’s IOP measurements and alert their clinician if they are at risk of experiencing a sudden increase in IOP, which can lead to vision loss.
Wearable and Mobile Eye Pressure Sensors
Wearable and mobile eye pressure sensors are being developed to enable patients to track their IOP measurements outside of a clinical setting. These devices use advanced sensors and algorithms to measure IOP and provide real-time feedback to patients.
For example, a wearable IOP sensor can be attached to a patient’s arm or wrist, providing continuous monitoring of IOP throughout the day. This can be particularly useful for patients with glaucoma, who may need to monitor their IOP regularly to manage their condition.
Advanced Imaging Techniques
Advanced imaging techniques, such as optical coherence tomography (OCT) and confocal scanning laser ophthalmoscopy (CSLO), are being integrated into eye pressure test machines to provide more detailed images of the ocular surface and anterior chamber.
These imaging techniques can help clinicians detect early signs of glaucoma and other ocular conditions, enabling more effective treatment and management. Additionally, advanced imaging can provide valuable information for researchers studying the pathophysiology of glaucoma and other ocular conditions.
Quantification of IOP Variability
Quantifying IOP variability is essential for understanding the complex dynamics of IOP measurement. Recent advancements in eye pressure test machines have enabled clinicians to measure IOP variability more accurately, providing valuable insights into the pathophysiology of glaucoma and other ocular conditions.
A study published in the Journal of Glaucoma found that patients with glaucoma experience a higher degree of IOP variability than healthy individuals. This suggests that IOP variability may be an important factor in the development and progression of glaucoma.
IOP variability is a critical factor in the management of glaucoma.
Design and Development Considerations for Eye Pressure Test Machines
The design and development process for eye pressure test machines involves a comprehensive consideration of various factors to ensure the production of high-quality devices. This includes integrating usability, safety, and performance requirements to ensure the device meets clinical needs while providing user-friendly operation.
Design and development phases for eye pressure test machines involve significant considerations for accuracy and precision, taking into account various technical, clinical, and regulatory standards.
User-Centered Design
User-centered design is an integral aspect in the development of eye pressure test machines. The goal is to create a device that is both effective in clinical settings and user-friendly. This involves conducting thorough research to understand the needs of end-users and healthcare professionals, ensuring the device meets requirements for accuracy, usability, and safety.
Some of the key considerations for user-centered design include:
- Conducting surveys and interviews with end-users and healthcare professionals to gather insights on device requirements and usability.
- Designing user interfaces that are intuitive and easy to navigate.
- Ensuring the device is lightweight and portable for convenient use in various settings.
- Providing user training and education to ensure successful operation and optimal performance.
Implementing user-centered design principles can significantly enhance the overall user experience, increasing device adoption and improving clinical outcomes.
Achieving Accuracy and Precision
Achieving accuracy and precision is crucial for eye pressure test machines, as these devices are used to diagnose and monitor various eye-related conditions. This can be achieved through rigorous design and development processes, including the selection of high-quality components, proper calibration, and regular maintenance.
Some key factors to consider for achieving accuracy and precision include:
- Carefully selecting high-quality sensors and measurement systems to ensure accurate readings.
- Implementing robust calibration protocols to ensure device accuracy and precision.
- Regularly maintaining the device to prevent equipment degradation and ensure optimal performance.
- Conducting thorough testing and validation to ensure the device meets clinical standards.
By prioritizing accuracy and precision, eye pressure test machines can provide reliable and trustworthy results, supporting optimal patient care.
Integration of Safety Features
Safety is a critical consideration in the design of eye pressure test machines, to prevent harm to users and ensure compliance with regulatory standards. This includes designing devices with safety features that prevent accidental injury, protect users from exposure to hazardous conditions, and mitigate the risk of device-related adverse events.
Important safety considerations include:
| Aspect | Description |
|---|---|
| Shielding and Containment | Proper shielding and containment to prevent users from coming into contact with hazardous components or environments. |
| Alert and Warning Systems | Implementation of alert and warning systems to notify users of potential hazards, anomalies, or malfunctions. |
| Mechanical and Electrical Safety | Designing the device to prevent mechanical and electrical malfunctions that could pose a risk to user safety. |
| Emergency Stop and Shut-Off Mechanisms | Implementation of emergency stop and shut-off mechanisms to quickly and safely stop the device in case of a malfunction or emergency. |
Design for Usability and Maintainability
Designing eye pressure test machines with usability and maintainability in mind is essential to ensure the device is both user-friendly and efficient to operate. This involves integrating features that facilitate easy cleaning and disinfection, simple maintenance tasks, and intuitive operations.
Important aspects for usability and maintainability include:
- Cleaning and Disinfection Protocols: Designing the device with easy-to-clean surfaces and ensuring proper protocols for disinfection to prevent cross-contamination.
- Maintenance Accessibility: Providing easy access to components and ensuring that routine maintenance tasks are straightforward and efficient.
- Operator-Friendly Controls: Designing user interfaces that are intuitive and easy to navigate, allowing healthcare professionals to quickly and efficiently perform tasks.
Designing eye pressure test machines with usability and maintainability in mind can enhance user satisfaction, reduce downtime, and optimize clinical workflow.
Compliance with Regulatory Standards
Ensuring compliance with regulatory standards is essential for eye pressure test machines to ensure patient safety and meet clinical requirements. This involves adhering to relevant regulatory guidelines and standards, such as those established by the FDA, CE marking, and IEC 60601.
Regulatory compliance can be achieved through:
- Conducting thorough risk assessments to identify potential hazards and mitigate them.
- Implementing quality management systems to ensure consistent and rigorous standards.
- Conducting rigorous testing and validation to demonstrate compliance with regulatory standards.
- Providing comprehensive documentation to demonstrate compliance and support device marketing.
By prioritizing regulatory compliance, eye pressure test machine manufacturers can ensure their devices meet the required standards, supporting optimal patient care and minimizing regulatory risks.
Patient Data Security
Patient data security is crucial for eye pressure test machines, as these devices often handle sensitive and personal patient information. This involves implementing robust security measures to prevent unauthorized access, data breaches, or other security incidents.
Important considerations for patient data security include:
- Implementing robust encryption protocols to protect patient data during storage, transmission, and retrieval.
- Ensuring secure data storage through password-protected storage devices or cloud-based services.
- Implementing secure authentication measures to control access to patient data.
- Providing regular software updates to address security vulnerabilities and patch potential risks.
Prioritizing patient data security can prevent unauthorized access to sensitive patient information and mitigate the risk of data breaches.
Final Wrap-Up
In conclusion, eye pressure test machines play a vital role in diagnosing and managing glaucoma. Their accuracy, reliability, and clinical applications make them an essential tool for healthcare professionals. By understanding the working mechanisms, significance, and types of eye pressure test machines, we can ensure that these machines are used efficiently and effectively to improve patient outcomes.
Helpful Answers
What is the ideal eye pressure for a healthy individual?
The ideal eye pressure for a healthy individual is typically around 10-21 mmHg. However, this can vary slightly from person to person.
How often should eye pressure be measured?
Eye pressure should be measured at least once a year for individuals over 60 years old, and as often as every 3-4 months for those with a family history of glaucoma or other eye conditions.
Can eye pressure test machines be used for children?
Yes, eye pressure test machines can be used for children, but they require special calibration and consideration of their smaller eye size.
What are some common errors associated with eye pressure test machines?
Some common errors associated with eye pressure test machines include calibration errors, instrument bias, and improper use or maintenance.