Fetal Heart Rate Machine is a medical device used to monitor the heartbeat of an unborn baby, providing critical information about their well-being and enabling healthcare professionals to make informed decisions during pregnancy, labor, and delivery.
The machine works by using sensors to detect the fetal heart rate and provide real-time data, which can be displayed on an oscilloscope or a digital screen. This data is essential for identifying potential complications and ensuring a healthy outcome for both the mother and the baby.
Types of Fetal Heart Rate Monitoring Systems: Fetal Heart Rate Machine
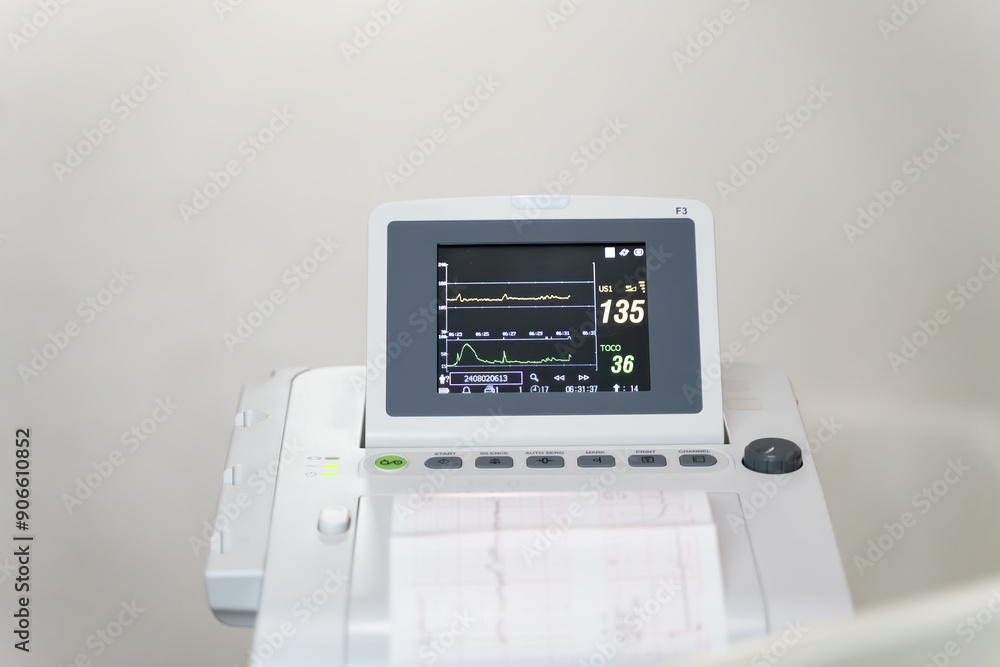
Fetal heart rate monitoring is a crucial aspect of obstetric care during pregnancy, labor, and delivery. The choice of monitoring system depends on the clinical need, patient comfort, and the skill level of the healthcare provider. In this section, we will explore the different types of fetal heart rate monitoring systems, their advantages, and disadvantages.
Electronic Fetal Monitoring (EFM)
Electronic fetal monitoring is a non-invasive method that uses a sensor to record the fetal heart rate in conjunction with the mother’s contractions. EFM is commonly used during labor, especially in low-risk pregnancies. The system consists of two internal sensors attached to the mother’s abdomen, one for measuring the fetal heart rate and the other for detecting contractions. The readings are displayed on a monitor, allowing healthcare providers to assess fetal well-being and identify any potential issues.
Electronic fetal monitoring has both advantages and disadvantages.
- Advantages: provides real-time data, allows for continuous monitoring, and enables healthcare providers to detect early signs of fetal distress.
- Disadvantages: may require hospital admission, can cause discomfort or pain for the mother, and may lead to unnecessary interventions.
Intermittent Auscultation (IA)
Intermittent auscultation is a traditional method that involves listening to the fetal heart rate with a Doppler device or a fetoscope. This technique is often used in low-risk pregnancies and in the early stages of labor. Healthcare providers typically check the fetal heart rate every 30 minutes to 1 hour during the first stage of labor. IA is a less invasive and less expensive method compared to EFM.
Advantages and Disadvantages of Intermittent Auscultation:
| Advantages | Disadvantages |
|---|---|
| Invasive, less expensive, and does not require hospital admission | May not detect early signs of fetal distress, requires skilled healthcare providers |
Internal Fetal Monitoring
Internal fetal monitoring involves inserting sensors or catheters into the woman’s uterus to track the fetal heart rate. This method is typically used in high-risk pregnancies or when the fetal heart rate is difficult to obtain through external methods. Internal monitors provide more accurate readings, but they also carry a higher risk of complications, such as infection or umbilical cord prolapse.
Internal fetal monitoring can be performed in two ways:
- Catheter method: involves inserting a catheter through the cervix into the uterus.
- Transabdominal scalp electrode method: involves inserting a thin electrode into the fetal scalp to measure the heart rate directly.
External Fetal Monitoring
External fetal monitoring is a non-invasive method that uses sensors placed on the mother’s abdomen to record the fetal heart rate and contractions. This technique is commonly used in low-risk pregnancies and during the first stage of labor.
Important Considerations:
When choosing a fetal heart rate monitoring system, healthcare providers should consider the individual needs of each patient, the clinical context, and the potential risks and benefits associated with each method.
Wearable Fetal Heart Rate Monitors
Wearable fetal heart rate monitors are portable devices that record the fetal heart rate remotely using sensors attached to the mother’s clothing or abdomen. These devices offer a non-invasive and comfortable alternative to traditional monitoring methods. Wearable monitors can be used during prenatal appointments, during labor, or at home.
Advantages:
Wearable fetal heart rate monitors enable mothers to track their baby’s heart rate remotely, providing real-time data, and enabling healthcare providers to monitor fetal well-being continuously.
Clinical Applications of Fetal Heart Rate Machines
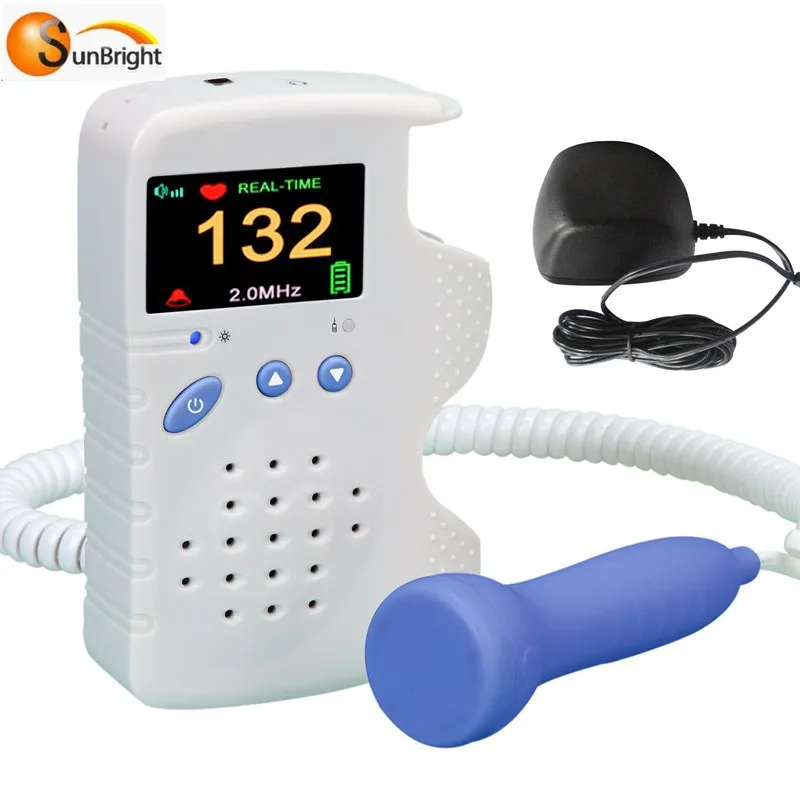
Fetal heart rate machines play a crucial role in monitoring the health and well-being of a fetus during various stages of pregnancy, labor, and delivery. These machines provide healthcare professionals with valuable information about the fetus’s heart rate, allowing them to make informed decisions about the care and treatment of the mother and baby.
Monitoring During Labor and Delivery
———————————
During labor and delivery, fetal heart rate monitoring is essential to ensure the baby’s health and well-being. The machine detects any changes in the baby’s heart rate, providing healthcare professionals with early warnings of potential complications.
Fetal heart rate monitoring during labor typically involves:
- Continuous monitoring of the baby’s heart rate throughout labor
- Monitoring for any changes in the baby’s heart rate, such as decelerations or accelerations
- Assessing the baby’s heart rate in response to different stimuli, such as fetal movement or uterine contractions
Effective fetal heart rate monitoring during labor enables healthcare professionals to identify potential complications, such as fetal distress, and take appropriate action to prevent harm to the baby.
Monitoring During Antepartum and Postpartum Periods
————————————————-
Fetal heart rate monitoring is not limited to labor and delivery. It can also be used during the antepartum (before labor) and postpartum (after labor) periods to monitor the baby’s health and detect any potential complications.
During the antepartum period:
- Fetal heart rate monitoring is used to detect any changes in the baby’s heart rate that may indicate fetal distress or other complications
- It helps healthcare professionals to monitor the baby’s well-being and adjust the mother’s care plan as needed
- It can also be used to monitor the baby’s heart rate in response to different stimuli, such as fetal movement or uterine contractions
During the postpartum period:
Postpartum fetal heart rate monitoring is essential to ensure the baby’s health and well-being after birth.
- Fetal heart rate monitoring during the postpartum period can detect any changes in the baby’s heart rate that may indicate complications, such as infection or blood loss
- It helps healthcare professionals to monitor the baby’s well-being and adjust the baby’s care plan as needed
- It can also be used to monitor the baby’s heart rate in response to different stimuli, such as feeding or crying
Applications During Prenatal Visits or Check-Ups
———————————————–
Fetal heart rate monitoring can also be used during prenatal visits or check-ups to monitor the baby’s health and detect any potential complications.
During prenatal visits:
- Fetal heart rate monitoring can be used to detect any changes in the baby’s heart rate that may indicate fetal distress or other complications
- It helps healthcare professionals to monitor the baby’s well-being and adjust the mother’s care plan as needed
- It can also be used to monitor the baby’s heart rate in response to different stimuli, such as fetal movement or uterine contractions
Examples of Fetal Heart Rate Tracings and Interpretation
Understanding fetal heart rate tracings is a crucial aspect of prenatal care, as it helps healthcare providers monitor the well-being of the fetus and identify any potential issues. Fetal heart rate tracings are a graphical representation of the fetal heart rate over a specific period, often in relation to contractions.
Normal Fetal Heart Rate Tracings
Normal fetal heart rate tracings are typically characterized by a baseline rate of 110-160 beats per minute (bpm), with occasional accelerations and decelerations.
| Fetal Heart Rate Tracing | Baseline Rate | Accelerations | Decelerations |
| — | — | — | — |
| Tracing 1: Normal Fetal Heart Rate Tracing | 120 bpm | Accelerations in fetal heart rate occur in response to fetal movement, which can be seen as increases in heart rate above 15 bpm lasting at least 15 seconds. | Decelerations are typically short-term and may be seen in response to contractions. |
| Tracing 2: Fetal Acceleration | 140 bpm | Fetal accelerations are increases in fetal heart rate that occur above 15 bpm lasting at least 15 seconds and are often seen in the face of fetal movement. | None observed. |
Abnormal Fetal Heart Rate Tracings
Abnormal fetal heart rate tracings can indicate potential issues with fetal well-being. It’s essential for healthcare providers to interpret these tracings carefully and in conjunction with other prenatal information.
| Fetal Heart Rate Tracing | Baseline Rate | Accelerations | Decelerations |
| — | — | — | — |
| Tracing 3: Variable Deceleration | 100 bpm | None observed. | Variable decelerations are seen in response to cord compression, which can be caused by umbilical cord prolapse or vasa previa. These decelerations are often irregular in shape and can vary in duration. |
| Tracing 4: Early Deceleration | 110 bpm | None observed. | Early decelerations are often seen in response to fetal head compression during contractions. They may be a sign of fetal head compression or potential fetal distress. |
Case Studies and Real-Life Scenarios

Fetal heart rate monitoring plays a crucial role in ensuring the well-being and safety of both the mother and the fetus during pregnancy and childbirth. Accurate interpretation of fetal heart rate patterns is essential in timely identification of potential complications, enabling prompt medical intervention when necessary. This section highlights a case study where fetal heart rate monitoring was critical in saving a mother’s and baby’s life.
Case Study: Delayed Fetal Heart Rate Deceleration
A 35-year-old pregnant woman at 37 weeks of gestation presented with symptoms of labor pain. Fetal heart rate monitoring was initiated, and an abnormal baseline shift was detected. The fetal heart rate baseline remained elevated throughout the monitoring period, and frequent late decelerations were observed. These findings indicated potential fetal distress. Prompt medical intervention was required to prevent further complications. The obstetrician performed an immediate cesarean section, and the baby was delivered successfully. Prolonged monitoring and accurate interpretation of fetal heart rate patterns saved the life of both the mother and the baby.
Real-Life Scenario: Fetal Heart Rate Monitoring in a High-Risk Pregnancy
A 28-year-old pregnant woman with a history of gestational diabetes and hypertension presented at 32 weeks of gestation. Fetal heart rate monitoring was initiated due to maternal concerns and symptoms of preterm labor. Continuous electronic fetal monitoring revealed non-reassuring patterns, including frequent variability and late decelerations. The obstetrician and medical team carefully monitored the situation and decided to administer corticosteroids to accelerate fetal lung maturity and prevent preterm birth complications. A subsequent ultrasound and non-stress test revealed a decrease in fetal movement and fetal heart rate decelerations despite steroid administration. As a result, a scheduled cesarean section at 35 weeks was performed, and the baby was delivered in a high-risk, well-equipped neonatal unit, where they received necessary care for their preterm birth.
Potential Consequences of Delayed or Incorrect Interpretation of Fetal Heart Rate Patterns, Fetal heart rate machine
Failure to recognize abnormal fetal heart rate patterns may result in delayed medical intervention. In such cases, potential complications include:
- Birth asphyxia: Prolonged exposure to hypoxia may lead to neurological damage or even death.
- Fetal distress: Unaddressed fetal distress may result in increased risk of fetal demise or severe birth injuries.
- Increased risk of cesarean delivery: Delays in fetal heart rate pattern recognition may necessitate emergency cesarean sections, potentially leading to increased medical and financial burdens for the mother.
- Elevated risk of litigation: Delayed or incorrect interpretation of fetal heart rate patterns may result in malpractice lawsuits, adding to the financial and emotional toll experienced by healthcare providers.
Accurate fetal heart rate monitoring, facilitated by dedicated medical professionals, is a critical component in preventing these complications and ensuring the well-being of mothers and their babies.
Importance of Standardized Fetal Heart Rate Interpretation Guidelines
To prevent misinterpretation and delayed medical intervention, healthcare providers should adhere to standardized guidelines for fetal heart rate pattern assessment. The American College of Obstetricians and Gynecologists (ACOG) recommends utilizing the 5-minute Apgar score, the 30-minute Apgar score, the fetal heart rate monitoring strip, and the non-stress test to evaluate fetal well-being. These guidelines promote consistency in interpreting fetal heart rate patterns and enable healthcare providers to accurately identify fetal distress, allowing prompt medical intervention when necessary.
Limited Research and the Future of Fetal Heart Rate Monitoring
Studies focusing on fetal heart rate monitoring are limited, particularly with regards to real-time, on-the-field applications. Research is needed to improve fetal heart rate monitoring tools and algorithms. Advances in technology and artificial intelligence may aid in automating fetal heart rate interpretation, minimizing the risk of delayed or incorrect diagnoses. Furthermore, more studies should focus on analyzing real-world cases to provide more detailed and nuanced data on fetal heart rate patterns and pregnancy outcomes.
Last Recap
In conclusion, the Fetal Heart Rate Machine plays a vital role in maternal and fetal care, enabling healthcare professionals to monitor the baby’s heart rate and identify potential issues early on. By understanding how these machines work and how to interpret their data, we can promote better health outcomes for mothers and babies alike.
Questions Often Asked
Q: What is the accuracy of fetal heart rate monitoring machines?
A: Fetal heart rate monitoring machines are generally accurate, but their accuracy can be affected by various factors, such as the quality of the sensor and the skill of the healthcare professional using the machine.
Q: Can I use a fetal heart rate monitor at home?
A: While it may be possible to purchase a fetal heart rate monitor for personal use, it is essential to note that these devices are not as accurate as those used in medical settings, and they should not be relied upon for critical fetal monitoring.
Q: How often should I have my fetal heart rate monitored during pregnancy?
A: The frequency of fetal heart rate monitoring depends on various factors, such as the individual’s pregnancy history and any existing medical conditions. Healthcare professionals will determine the optimal frequency of monitoring based on each patient’s needs.