As how does a dialysis machine work takes center stage, this passage explores the intricacies of the dialysis process, ensuring a comprehensive understanding of the topic.
Dialysis machines play a crucial role in treating patients with renal failure by filtering waste products and excess fluids from the blood. The development of dialysis machines has a rich history, dating back to the early 20th century, with ongoing advancements aimed at improving efficiency and effectiveness.
Introduction to Dialysis Machines

Dialysis machines have revolutionized the treatment of renal failure, allowing patients to recover from the devastating effects of kidney disease. Renal failure, also known as end-stage renal disease (ESRD), occurs when the kidneys are no longer able to properly filter waste and excess fluids from the blood. This can lead to a range of serious complications, including electrolyte imbalances, fluid buildup, and potentially life-threatening conditions such as heart failure and stroke. Dialysis machines have become a lifeline for millions of people worldwide, providing a vital connection between the patient and the outside world.
The Purpose of Kidney Dialysis Machines
Dialysis machines are designed to perform the same functions as healthy kidneys, removing waste products and excess fluids from the blood. This is achieved through a process called dialysis, which involves the use of a semi-permeable membrane to filter the blood. There are several types of dialysis machines, each with its own unique design and functionality. In-center hemodialysis, peritoneal dialysis, and home hemodialysis are the primary types of dialysis used in modern medicine.
Dialysis machines are used to treat patients with acute or chronic kidney disease, including patients with kidney failure due to diabetes, high blood pressure, or other underlying conditions. The machines are designed to be adaptable to individual patient needs, with adjustable settings and parameters for optimal treatment.
A Brief History of Dialysis Machine Development
The development of dialysis machines dates back to the early 20th century, when Dr. Gustaf Hylander in 1904 began experimenting with dialysis to treat patients with kidney disease. The first dialysis machine was developed in 1943 by a team of scientists led by Dr. Willem J. Kolff. The machine used a rotating drum to filter the blood, and it was able to remove waste products and excess fluids from the blood.
Over the years, dialysis machines have undergone significant advancements in terms of design, technology, and functionality. Modern machines are designed for greater efficiency, comfort, and safety, with features such as:
- Microprocessors for precision control and monitoring
- Sensors for continuous monitoring of blood flow and pH levels
- Automated fluid management systems for accurate fluid removal
- Advanced software for personalized treatment plans
The Importance of Dialysis in Modern Medicine
Dialysis machines have become an essential tool in modern medicine, providing life-saving treatment for patients with kidney disease. Dialysis has improved the quality of life and reduced mortality rates for patients with renal failure, extending their life expectancy and improving their overall well-being.
In addition to its therapeutic benefits, dialysis has also contributed to significant advancements in the field of nephrology, leading to better understanding and management of kidney disease. The use of dialysis has enabled researchers and clinicians to study the pathophysiology of kidney disease, identify new therapeutic targets, and develop effective treatments.
Dialysis machines have also been used in research and development of new treatments for other diseases, including cardiovascular disease, diabetes, and obesity. The technology and expertise developed in dialysis research have paved the way for innovations in other fields of medicine, making a significant impact on human health and well-being.
Future Directions in Dialysis Machine Development
The development of dialysis machines continues to be an active area of research, with a focus on improving efficiency, comfort, and safety. New technologies such as continuous renal replacement therapy (CRRT) and portable dialysis devices are being developed to provide more flexible and effective treatment options for patients.
Advances in nanotechnology and biomaterials are also being explored for use in dialysis machines, enabling the development of smaller, more efficient devices with improved biocompatibility and biostability.
Conclusion
In conclusion, dialysis machines have revolutionized the treatment of renal failure, providing a lifeline for millions of people worldwide. With ongoing advancements in technology, design, and functionality, dialysis machines continue to play a vital role in modern medicine, improving the quality of life and reducing mortality rates for patients with kidney disease.
Basic Components of a Dialysis Machine
Dialysis machines are complex medical devices consisting of key components that work in tandem to facilitate the removal of waste products from the blood. The primary components of a dialysis machine include pumps, filters, and fluid reservoirs, each playing a vital role in the dialysis process.
The pumps, typically rotary or peristaltic, work to circulate the blood and dialysate (a solution infused with water and substances that help remove waste products) through the dialysis circuit. The pumps are designed to operate at precise rates to ensure optimal flow rates and minimize the risk of complications.
The filters, also known as dialyzers, are the heart of the dialysis process, responsible for removing waste products and excess fluids from the blood. These filters are designed to allow waste products to pass through while keeping blood cells intact. Hemodialysis machines use high-flux filters, which can effectively remove waste products and excess fluids from the blood.
Fluid reservoirs hold the dialysate solution that is infused into the dialysis circuit. These reservoirs are typically large containers that can hold several liters of solution, which are replenished as needed.
Dialysis machines can be broadly categorized as either hemodialysis or peritoneal dialysis machines. Hemodialysis machines use a dialyzer to filter the blood, while peritoneal dialysis machines utilize the peritoneal membrane in the abdomen as a natural filter.
Sub-type Comparison
===============
### Hemodialysis Machines
Hemodialysis machines typically use an extracorporeal circuit to remove waste products from the blood. This process occurs outside the body where a filter, called a dialyzer, separates waste products from the blood. They are commonly used for both acute and chronic dialysis.
### Peritoneal Dialysis Machines
Peritoneal dialysis machines, on the other hand, use the peritoneum in the patient’s abdomen as a filter to remove waste products. The dialysate solution is infused into the peritoneum and absorbed back into a collection bag. Continuous ambulatory peritoneal dialysis (CAPD) and automated peritoneal dialysis (APD) are common types of peritoneal dialysis.
Pumps in Dialysis Machines
Dialysis machines use two main types of pumps for controlling blood and dialysate flow rates: rotary and peristaltic.
###
-
#### Rotary Pumps
- Blood Flow: Adequate blood flow is essential for efficient water removal during dialysis. Increased blood flow can enhance the rate of water removal and improve the overall effectiveness of the treatment.
- Membrane Permeability: The permeability of the dialysis membrane affects the rate of water and solute removal. More permeable membranes enable faster removal of waste products and excess fluids.
- Osmotic Gradient: The osmotic gradient across the membrane influences the rate of water removal. An increased osmotic gradient drives more water across the membrane, resulting in faster water removal.
- Reduce Fluid Overload: Excess fluids can lead to fluid overload, which increases the risk of cardiovascular complications, hypertension, and pulmonary edema.
- Prevent Electrolyte Imbalances: Effective removal of waste products helps to maintain electrolyte balance, reducing the risk of complications such as arrhythmias and muscle weakness.
- Improve Nutritional Status: Adequate water removal enables patients to maintain a healthy nutritional status, reducing the risk of malnutrition and related complications.
-
Membrane-Based Dialysis Systems
The development of membrane-based dialysis systems has increased the efficiency of solute transport across the dialyzer membrane. These systems utilize semipermeable membranes to remove waste products from the blood, resulting in improved solute clearance rates.
-
Silicon Chip-Based Controllers
The integration of silicon chip-based controllers has enabled real-time monitoring of patient parameters and automated adjustments to dialysis settings. This has improved the precision and safety of therapy, reducing the risk of adverse events.
-
Closed-Loop Dialysis Systems
Closed-loop dialysis systems utilize real-time feedback from sensors to adjust dialysis settings and maintain optimal fluid balances within the blood. This technology allows for more efficient and personalized treatment.
-
Portable Dialysis Machines
The development of portable dialysis machines has expanded treatment options for patients requiring dialysis outside of clinical settings. These machines are designed for ease of use and transportation, enhancing the quality of life for patients.
- Enhanced solute clearance rates, reducing the risk of cardiovascular complications
- Improved fluid management, minimizing the risk of fluid overload and associated comorbidities
- Increased treatment efficiency, allowing for more sessions per week and improved overall patient well-being
- Enhanced patient comfort, reducing the risk of complications associated with prolonged dialysis sessions
-
Artificial Intelligence (AI)-Integrated Systems
AI-integrated systems will further enhance treatment efficiency and patient outcomes by analyzing complex data sets and optimizing therapy settings in real-time.
-
Biomimetic Devices
Biomimetic devices will mimic the natural filtration process of the kidneys, potentially reducing the need for dialysis or improving treatment outcomes.
-
Nanotechnology-Based Solutions
Nanotechnology-based solutions will enhance solute removal efficiency, improve membrane durability, and reduce treatment time.
Rotary pumps are widely used in dialysis machines due to their precision and reliability in managing flow rates. These pumps consist of rotating vanes or a rotor that drives fluid through the tubing. They are known for their ability to provide precise flow rates while using less energy compared to peristaltic pumps.
#### Peristaltic Pumps
Peristaltic pumps are another common type of pump used in dialysis machines. They are often preferred for their simplicity and low maintenance requirements. These pumps use rollers or rollers to compress a portion of tubing to push fluid forward. They require more energy than rotary pumps but are cost-effective.
Filters in Dialysis Machines
Dialysis machines use filters, known as dialyzers, to remove waste products from the blood. The primary function of a dialyzer is to allow waste products to be washed away while keeping blood cells intact. Hemodialysis and peritoneal dialysis machines employ different types of filters tailored to their specific requirements.
###
-
#### Haemodialysis (HD) Filters
HD Filters primarily function by using a semi-permeable membrane to remove waste products from the blood. High-flux dialyzers are designed for effective removal of waste products and excess fluids. Haemodiafiltration (HDF) dialyzers combine both diffusion and convection mechanisms to enhance the removal of waste products from the blood.
#### Peritoneal (PD) Filters
PD Filters make use of the peritoneum as a natural filter for waste product removal. The dialysate solution is infused into the peritoneum and absorbed back into a collection bag. PD Filters must be carefully prepared and handled to prevent peritonitis or other complications.
Fluid Reservoirs in Dialysis Machines
Dialysis machines require fluid reservoirs to hold the dialysate solution that is infused into the dialysis circuit. The primary function of these reservoirs is to contain and manage the dialysate solution until it is infused into the patient’s body. The fluid reservoirs are designed to maintain optimal temperature and chemical properties to ensure efficacy and patient safety.
Water Removal Mechanisms in Dialysis

Dialysis is a life-saving treatment that uses two mechanisms to remove excess fluids and waste products from the blood: osmosis and diffusion. Understanding these mechanisms is crucial for optimizing the dialysis process and maintaining patient well-being. Osmosis involves the passive movement of water molecules from an area of high concentration to an area of low concentration through a semipermeable membrane, while diffusion is the random movement of particles from an area of high concentration to an area of low concentration until equilibrium is achieved.
Ultrafiltration
Ultrafiltration is a critical mechanism in dialysis that involves the use of pressure to remove excess fluids from the blood. This process occurs when a semipermeable membrane separates the blood from an osmotic solution, allowing water and small molecules to pass through while larger molecules, such as proteins and blood cells, remain in the blood. The increased pressure across the membrane drives the movement of water and waste products from the blood into the osmotic solution.
Diffusion, How does a dialysis machine work
Diffusion plays a vital role in the removal of waste products, including urea, creatinine, and other toxins, from the blood during dialysis. This process relies on the concentration gradient between the blood and the dialysate to enable the movement of waste products from the blood into the dialysate. The rate of diffusion depends on several factors, including the concentration gradient, membrane permeability, and blood flow.
Factors Affecting Water Removal
Several factors influence the rate of water removal during dialysis, including:
Impact on Patient Outcomes
Optimizing water removal during dialysis is crucial for maintaining patient well-being and preventing complications. Efficient removal of excess fluids and waste products helps to:
Control Systems in Dialysis Machines
In the realm of dialysis, control systems play a pivotal role in regulating the intricate process of removing waste products from the blood. These sophisticated systems ensure that the dialysis machine functions optimally, maintaining a delicate balance between the patient’s life-sustaining needs and the risk of complications.
Analog vs. Digital Control Systems
Dialysis machines employ either analog or digital control systems, each with its own set of benefits and limitations.
Types of Analog Control Systems
Analog control systems rely on continuous signals to regulate the dialysis process. These systems are often found in older dialysis machines and typically use a series of tubes and valves to control the flow of dialysate.
* Analog control systems are less expensive to implement and maintain.
* They offer a simple and intuitive interface for operators.
However, analog control systems also have several limitations.
* Analog systems can be prone to errors due to signal degradation.
* They often require manual adjustments to achieve optimal results.
Types of Digital Control Systems
Digital control systems, on the other hand, employ discrete signals to regulate the dialysis process. These systems are commonly found in modern dialysis machines and offer numerous advantages over analog systems.
* Digital control systems are highly accurate and repeatable.
* They provide real-time monitoring and feedback to operators.
* Digital systems can be easily integrated with other medical devices.
Digital control systems also offer several benefits in terms of performance.
* They can operate at higher speeds and with greater precision.
* Digital systems are less susceptible to errors and malfunctions.
Despite these advantages, digital control systems also have some limitations.
* Digital systems can be more expensive to implement and maintain.
* They often require a higher level of technical expertise for operation and maintenance.
In conclusion, the choice of control system ultimately depends on the specific needs of the patient and the dialysis machine being used. While analog control systems offer a more traditional and simpler approach, digital control systems provide greater accuracy, precision, and flexibility.
Evolution of Dialysis Machines
The dialysis machine has undergone significant advancements in technology over the years, transforming the treatment process for patients with kidney failure. From the first manual machines to today’s sophisticated, automated systems, these developments have improved efficiency, effectiveness, and patient comfort.
Key Technological Advancements in Dialysis Machine Development
The evolution of dialysis machines has been driven by breakthroughs in materials science, electronics, and software. These innovations have enabled the creation of more efficient, user-friendly, and patient-centered machines.
Impact on Patient Outcomes
The advancements in dialysis machine technology have significantly improved patient outcomes, including:
Current Trends and Future Directions in Dialysis Machine Technology
As the field of dialysis continues to evolve, future advancements are expected to focus on:
The evolution of dialysis machine technology has come a long way in improving patient outcomes, and future innovations will continue to push the boundaries of what is possible in dialysis care. By advancing the treatment process, we can enhance the lives of patients with kidney failure.
Final Conclusion: How Does A Dialysis Machine Work
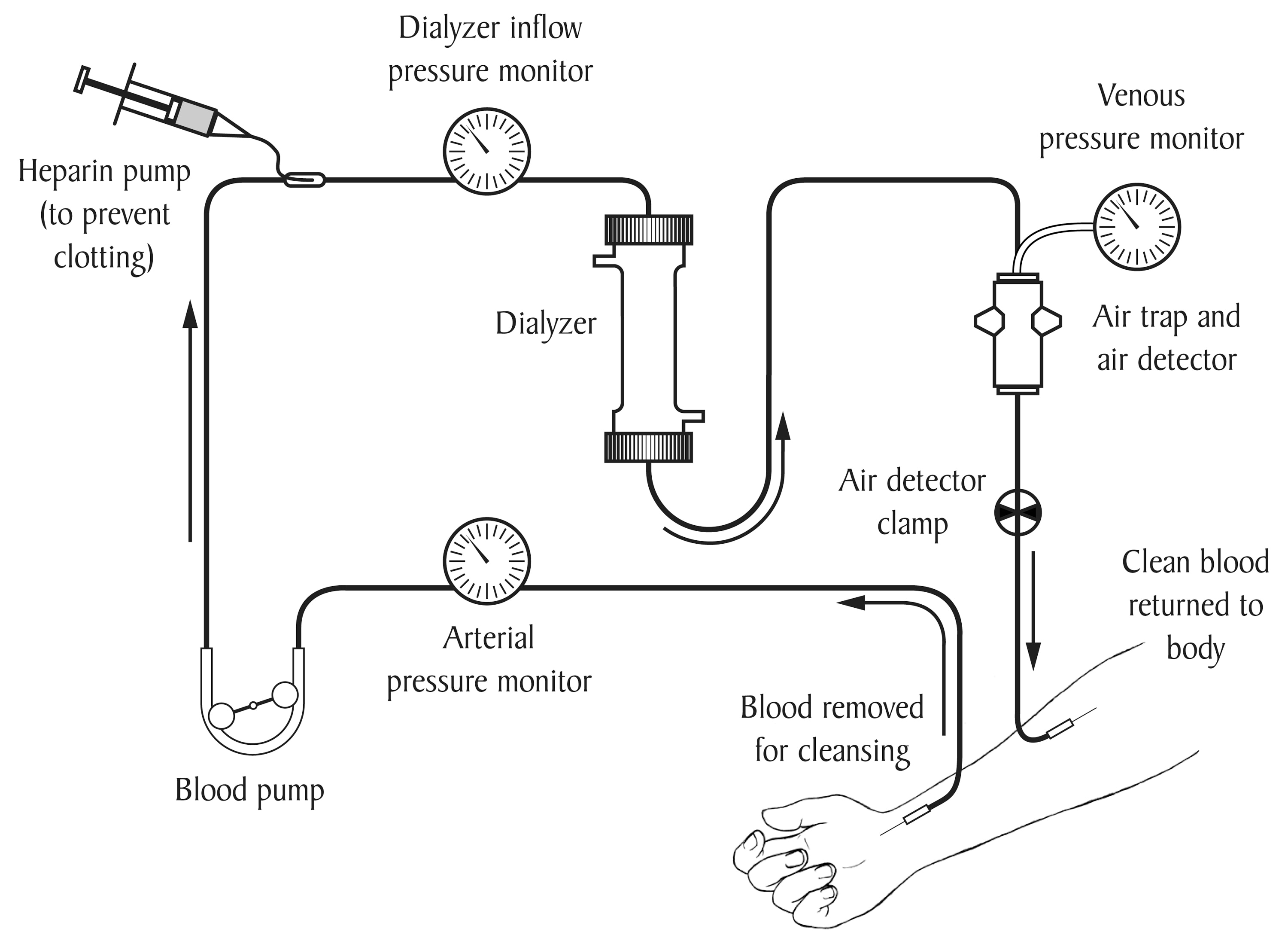
In conclusion, understanding how a dialysis machine works is essential for patients undergoing treatment and healthcare professionals alike. By exploring the various components, processes, and safety features of dialysis machines, we can better appreciate the complexities of renal failure treatment and the importance of dialysis in modern medicine.
FAQ Corner
What are the different types of dialysis machines?
Hemodialysis and peritoneal dialysis are the two primary types of dialysis machines, each with its own set of components and processes.
How often must a person use a dialysis machine?
Dialysis treatment is typically required three times a week, with each session lasting several hours, although this may vary depending on individual factors.
What are the benefits of dialysis machines?
Dialysis machines enable patients with renal failure to lead relatively normal lives, free from the burden of excessive waste products and excess fluids in their blood.
Are dialysis machines safe?
Dialysis machines are designed with safety features, including alarms and interlocks, to prevent accidents and ensure a secure treatment experience.