How long can someone live on a Bipap machine sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail and brimming with originality from the outset. As patients rely on Bipap machines for respiratory support, it raises essential questions about the efficacy and long-term use of these machines. The purpose of this discussion is to provide a comprehensive overview of the topic, exploring the benefits and drawbacks of long-term Bipap use, the economic and social implications, and the latest research and developments in the field.
The Bipap machine has become a crucial tool in respiratory therapy, providing support for patients with chronic respiratory conditions, such as sleep apnea and COPD. These machines have the ability to deliver life-supporting ventilation, making them an essential lifeline for many patients. However, the long-term use of Bipap machines has sparked controversy, with some arguing that they can lead to respiratory muscle atrophy and other complications.
Understanding Bipap Machines

In the realm of respiratory therapy, Bipap machines play a crucial role in assisting patients with breathing difficulties. These machines have become a staple in hospitals and homes, providing essential support to individuals suffering from respiratory disorders. The purpose of Bipap machines is to deliver air pressure to help patients breathe more easily, making it possible for them to maintain an optimal level of oxygenation and carbon dioxide removal.
Bipap machines, also known as bilevel positive airway pressure machines, have distinct functions that set them apart from other ventilators. Unlike traditional ventilators, Bipap machines deliver two different levels of air pressure: one for inhalation and another for exhalation. This unique feature allows patients to breathe in and out with greater ease, reducing the workload on their respiratory system.
Basics of Bipap Machines
A Bipap machine typically consists of a control unit, a humidifier, and a mask or nasal tube. The control unit is the brain of the machine, responsible for monitoring the patient’s breathing patterns and adjusting the air pressure accordingly. The humidifier adds moisture to the air, preventing dryness in the patient’s respiratory tract. The mask or nasal tube delivers the pressurized air to the patient, allowing them to breathe comfortably.
Key Features of Bipap Machines
Bipap machines offer several key features that make them highly effective in respiratory therapy:
- Variable Air Pressure: Bipap machines can adjust the air pressure to meet the individual needs of each patient, taking into account factors such as their lung capacity, respiratory rate, and oxygen saturation.
- Spontaneous Breathing: Patients using Bipap machines are allowed to breathe naturally, without the need for artificial ventilation. This feature helps maintain muscle strength and coordination in the diaphragm and other respiratory muscles.
- Continuous Air Pressure: Bipap machines provide constant air pressure during inhalation and exhalation, ensuring a stable flow of oxygen and carbon dioxide exchange.
- Alarm Systems: Modern Bipap machines come equipped with advanced alarm systems that detect potential issues, such as low oxygen saturation or high carbon dioxide levels, alerting healthcare professionals to take prompt action.
- Mobility: Many Bipap machines are lightweight and portable, allowing patients to move around freely while receiving treatment.
Benefits of Bipap Machines
The use of Bipap machines has numerous benefits for patients with respiratory disorders:
- Improved Oxygenation: Bipap machines deliver precise air pressure, ensuring optimal oxygen levels in the blood and tissues.
- Enhanced Respiratory Function: By assisting patients with breathing, Bipap machines help maintain muscle strength and coordination in the diaphragm and other respiratory muscles.
- Reduced Fatigue: Bipap machines alleviate the physical strain on patients, allowing them to rest and conserve energy.
- Increased Mobility: With the freedom to move around while receiving treatment, patients can engage in daily activities and maintain their independence.
Long-term Use and Efficacy: How Long Can Someone Live On A Bipap Machine

Using a BiPAP machine can be a life-changing intervention for patients suffering from chronic respiratory conditions such as sleep apnea and chronic obstructive pulmonary disease (COPD). When used properly, long-term BiPAP therapy has been shown to improve the quality of life, reduce the frequency of hospitalizations, and slow disease progression. However, like any medical treatment, there are benefits and drawbacks to long-term BiPAP use that must be carefully considered.
Clinical Benefits
Regular monitoring and adjustment of BiPAP settings are crucial to maintaining optimal efficacy. A properly calibrated BiPAP machine can provide life-sustaining support, improving breathing patterns, and alleviating symptoms associated with chronic respiratory conditions. For instance, a study published in the Journal of Clinical Sleep Medicine revealed that long-term BiPAP therapy resulted in significant improvements in oxygen saturation and sleep quality among patients with chronic respiratory disease.
- Frequency of hospitalizations
- Quality of life
- Disease progression
- Improved respiratory function
Hospitalization rates have been found to decrease in patients receiving prolonged BiPAP therapy, as this intervention helps regulate their breathing patterns during sleep.
Studies have demonstrated that long-term BiPAP therapy improves overall quality of life by reducing fatigue, anxiety, and depression associated with chronic respiratory conditions.
Research suggests that BiPAP therapy, when used consistently, can slow down disease progression, thereby improving life expectancy for these patients.
A study in the European Respiratory Journal revealed that prolonged BiPAP therapy enhanced lung function and reduced respiratory muscle fatigue in patients with COPD.
Limitations and Safety Concerns
While BiPAP therapy offers numerous benefits, there are also potential limitations and risks associated with long-term use. Some patients may experience issues such as skin irritation from the face mask, claustrophobia, or anxiety related to the unfamiliar sensation of breathing through a non-invasive mask. Additionally, individuals with certain medical conditions, such as cardiac arrhythmias, may need to exercise caution when using BiPAP machines.
- Equipment-related issues
- Muscle disuse atrophy
- Cognitive impairment
- Mental health concerns
Leaks in the mask or tubing can lead to ineffective therapy, necessitating prompt equipment adjustments.
Long-term reliance on BiPAP support may lead to weakened diaphragmatic and thoracic musculature, increasing the risk of future respiratory complications.
Chronic respiratory patients receiving prolonged BiPAP therapy may experience cognitive declines due to reduced oxygenation and chronic sleep disruptions.
Prolonged use of BiPAP machines can lead to dependence or feelings of helplessness, highlighting the importance of regular psychological evaluations and support.
Regular monitoring of BiPAP settings and adjustments as needed are essential to optimize patient outcomes.
Economic and Social Considerations
The economic implications of long-term BiPAP use can be significant, with costs including the price of the equipment, medication, and ongoing maintenance. As patients and their families navigate the costs associated with BiPAP therapy, it’s essential to understand the various resources available to help make this care more accessible.
Treatment Costs
The cost of a BiPAP machine can vary depending on the specific model, brand, and features, ranging from $500 to $2,000 or more. Additionally, patients may need to incur costs for replacement parts, filters, and maintenance. Medications required to supplement BiPAP therapy, such as oxygen and sleep medication, can also contribute to the overall expense. According to the Sleep Health Foundation, the average annual cost of sleep apnea treatment can range from $2,000 to $10,000 or more.
| Cost Components | Ranges |
|---|---|
| BiPAP Machine | $500-$2,000 or more |
| Replacement Parts and Filters | $50-$200 or more |
| Medications (oxygen, sleep aids) | $1,000-$5,000 or more annually |
Financial Assistance Options
Despite the costs associated with BiPAP therapy, several resources are available to help patients and families cover these expenses. Insurers and private companies may offer financial assistance, grants, and patient assistance programs (PAPs) to help offset the costs. Additionally, online resources and support groups provide information on affordable options for BiPAP equipment and care.
- Insurance coverage: Check with your insurer to see if they cover BiPAP equipment and ongoing care.
- Patient Assistance Programs (PAPs): Many manufacturers and private companies offer PAPs to help patients afford their medications and essential equipment.
- Grants and funding: Organizations and online resources provide information on grants and funding opportunities for sleep apnea treatment and BiPAP care.
Support and Resources
In addition to exploring financial assistance options, it’s essential for patients and families to understand the importance of ongoing support and resources. Sleep apnea support groups, online forums, and medical professionals can provide valuable guidance and help patients navigate the complexities of BiPAP therapy.
- Sleep apnea support groups: Local and online support groups connect patients, caregivers, and medical professionals to share experiences and advice.
- Online forums and resources: Websites and online forums provide information on BiPAP equipment, ongoing care, and affordable options.
- Medical professionals: Consult with healthcare providers for personalized guidance on managing BiPAP therapy and addressing related concerns.
Personal Stories and Experiences
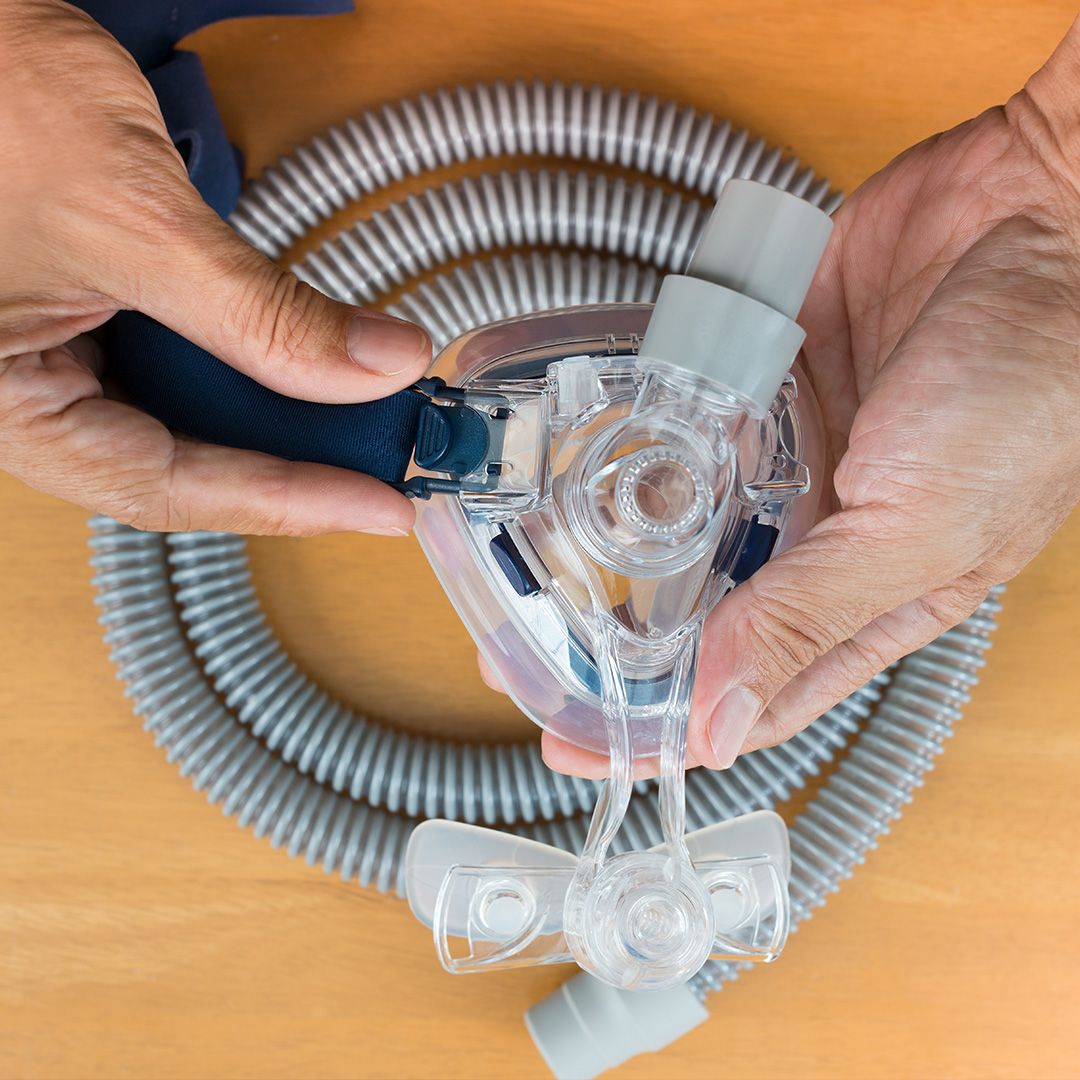
When it comes to long-term use of Bipap machines, personal stories and experiences offer valuable insights into the realities of living with respiratory support. These accounts provide a human perspective, highlighting the triumphs and challenges faced by individuals who rely on Bipap machines for extended periods.
Overcoming Adversity with Bipap Machines
The journey of living with a Bipap machine is often marked by a series of triumphs over adversity. Individuals like Sarah, a 35-year-old mother of two, have found the strength to continue living an active life despite the challenges posed by respiratory conditions. With the support of her loved ones and the assistance of her Bipap machine, Sarah has learned to adapt and overcome obstacles that would have seemed insurmountable in the past.
Redefining Independence with Bipap Technology, How long can someone live on a bipap machine
The benefits of Bipap machines extend beyond their medical applications. For individuals like David, a 50-year-old retired mechanic, the technology has provided a sense of independence that was previously unimaginable. David’s Bipap machine allows him to live a relatively normal life, free from the constraints of restrictive hospital environments. He is now able to pursue his hobbies and interests without fear of exacerbating his respiratory condition.
Building a Support Network through Bipap Patient Communities
Living with a Bipap machine can be a lonely experience, but many patients have found solace in online communities and support groups. For patients like Emily, a 28-year-old artist, these networks have provided a lifeline during times of crisis. By sharing their experiences and advice, Emily and her fellow patients have formed lasting bonds and a sense of belonging that transcends geographical boundaries.
Breaking Down Stigmas Associated with Respiratory Support
The stigma surrounding respiratory conditions and Bipap machines continues to be a major obstacle for many patients. However, individuals like James, a 40-year-old entrepreneur, are working to change this narrative by advocating for greater awareness and acceptance. By sharing his story and highlighting the benefits of Bipap machines, James hopes to inspire others to see beyond the stigmas and focus on the reality of living with respiratory conditions.
Current Research and Developments
Recent studies have been conducted to investigate the long-term effects of BiPAP use on respiratory health and patient outcomes. These investigations have aimed to enhance our understanding of the efficacy and safety of BiPAP therapy, as well as identify areas for potential improvement.
Long-term Effects of BiPAP Use
Research has shown that long-term use of BiPAP can lead to significant improvements in lung function and overall quality of life for patients with respiratory conditions such as COPD, sleep apnea, and neuromuscular disease. However, some studies have also raised concerns about potential long-term side effects, including increased risk of respiratory acidosis, pneumonia, and hospitalization.
According to a study published in the European Respiratory Journal, patients with COPD who used BiPAP therapy for an average of 2 years showed a significant improvement in lung function, as measured by FEV1 (forced expiratory volume in 1 second).
Some researchers have also investigated the impact of BiPAP therapy on patient mortality and morbidity. For example, a study published in the Journal of Sleep Research found that long-term use of BiPAP in patients with obstructive sleep apnea was associated with a significant reduction in mortality risk.
Potential Areas of Innovation in BiPAP Technology
Several areas of innovation have been identified in the development of BiPAP technology, including:
- Advancements in mask design and comfort: Researchers have been working to develop more comfortable and adaptable masks that can accommodate a wide range of patient needs and preferences.
- Improved ventilation algorithms: Newer BiPAP devices are incorporating advanced ventilation algorithms that can better adapt to changing patient conditions and adjust breathing pressure in real-time.
- Integration with other health technologies: BiPAP devices are increasingly being integrated with other health technologies, such as portable oxygen concentrators and pulse oximeters, to provide more comprehensive respiratory support.
- Faster and more efficient setup: Some researchers are exploring ways to simplify the setup process for BiPAP devices, making them easier to use and reducing patient anxiety and stress.
Emerging Trends in BiPAP Design
The design of BiPAP devices is also evolving, with a focus on making them more compact, portable, and user-friendly. This is driven by the need to provide respiratory support in a variety of settings, including home care, long-term care facilities, and emergency medical situations.
Some BiPAP devices are now being designed with compact and lightweight designs, making them easier to transport and store.
In addition to these trends, researchers are also exploring the potential for wearable BiPAP devices that can be integrated into clothing or worn on the body. This could provide patients with greater freedom and flexibility, as well as improved comfort and convenience.
Epilogue
As we delve into the world of Bipap machines, it becomes clear that their use has profound implications for patients, families, and healthcare providers. While they offer hope and support for those in need, they also pose risks and challenges that must be carefully managed. In this discussion, we have explored the benefits and drawbacks of long-term Bipap use, the economic and social implications, and the latest research and developments in the field. Ultimately, the decision to use a Bipap machine should be made with careful consideration and consultation with healthcare professionals.
FAQ Guide
Q: Can I use a Bipap machine at home?
A: Yes, many patients use Bipap machines at home with the guidance of a healthcare provider. However, it is essential to follow the manufacturer’s instructions and take regular cleaning and maintenance to prevent infections.
Q: Are Bipap machines covered by insurance?
A: The coverage of Bipap machines by insurance varies depending on the insurance provider and the individual’s policy. It is essential to check with the insurance provider to determine if coverage is available.
Q: Can I use a Bipap machine if I have a tracheostomy tube?
A: Yes, Bipap machines can be used with a tracheostomy tube. However, it is essential to consult with a healthcare provider to ensure proper set-up and use.
Q: Can I use a Bipap machine if I have a pacemaker or other implantable device?
A: You should consult with your healthcare provider and the pacemaker manufacturer to determine if it is safe to use a Bipap machine with a pacemaker or other implantable device.